Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Medicina (Buenos Aires)
versión impresa ISSN 0025-7680
Medicina (B. Aires) vol.71 no.4 Ciudad Autónoma de Buenos Aires jul./ago. 2011
ARTÍCULO ORIGINAL
Neutrophil predominance in induced sputum from asthmatic patients. Therapeutic implications and role of clara cell 16-KD protein
Elisa M. Uribe Echevarría, Cristina A. Maldonado, Agustín M. Uribe Echevarría, Agustín Aoki
Centro de Microscopía Electrónica, Facultad de Ciencias Médicas, Universidad Nacional de Córdoba
Dirección postal: Dra. Elisa M. Uribe Echevarría, Centro de Microscopía Electrónica, Pabellón de Biología Celular, Facultad de Ciencias Médicas, Universidad Nacional de Córdoba, Haya de la Torre y Enrique Barros, 5000 Córdoba, Argentina
Fax (54-351) 4333-2220 e-mail: uribe@cmefcm.uncor.edu
Abstract
Eosinophil is considered to be a main protagonist in asthma; however, often discordances between clinical manifestations and response to treatment are observed. We aimed to determine the occurrence of neutrophil predominance in asthma and to identify its characteristics on the basis of clinical-functional features, induced sputum cellular pattern and soluble molecules, to guide the appropriated anti-inflammatory therapy. A total of 41 patients were included in randomized groups: 21-40 year-old, with stable mild-to-severe asthma, steroid-naïve and non-smokers. An induced sputum sample was obtained under basal conditions, a second one after treatment with budesonide (400 μg b.i.d.) or montelukast (10 mg/d) for six weeks, and a final one after a 4-week washout period. By cytospin we evaluated eosinophil (EP) or neutrophil predominance (NP), and in supernatant we determined LTE4, and CC16. Peak expiratory flow variability (PEFV) was measured. A total of 23/41 patients corresponded to EP and 18/41 patients to NP. The PEFV was higher in EP than in NP. LTE4 was higher with NP than with EP. No difference was found for CC16. Montelukast reduced the predominant cell in both subsets, whereas budesonide only reduced eosinophils in EP. Budesonide and montelukast reduced PEFV in EP but not in NP. Considering the total treated-samples in each subset, CC16 level increased significantly in EP. In conclusion: a NP subset of asthmatic patients was identified. These patients show a lower bronchial lability; the leukotriene pathway is involved which responds to anti-leukotriene treatment. This phenotype shows a poor recovery of CC16 level after treatment.
Key words: Asthma; Neutrophil; CC16; Budesonide; Montelukast
Resumen
Predominio de neutrófilos en esputo inducido de asmáticos. Implicancias terapéuticas y rol de la proteína 16-kD de la célula clara. El eosinófilo es considerado la célula protagonista principal en el asma; sin embargo, a menudo se observan discordancias entre las manifestaciones clínicas y la respuesta de los pacientes al tratamiento. Nos propusimos determinar la ocurrencia de predominio de neutrófilos en el asma e identificar las características clínico-funcionales, el patrón celular y las moléculas solubles del esputo inducido, para guiar el tratamiento apropiado anti-inflamatorio. Se incluyeron 41 pacientes: 21 a 40 años de edad, con asma estable leve a grave, no tratados con esteroides tópicos ni sistémicos y no fumadores. Se obtuvo una muestra de esputo inducido en condiciones basales, una segunda muestra después del tratamiento al azar con budesonida (400 μg dos veces al día) o el montelukast (10 mg/d) durante seis semanas, y una final después de un período de lavado de 4 semanas. En el frotis por citocentrifugado se evaluó el predominio de eosinófilos (EP) o neutrófilos (NP), y en el sobrenadante se determinó LTE4, y CC16. Se midió la variabilidad del flujo espiratorio máximo (PEFV). Un total de 23/41 pacientes correspondieron al EP y 18/41 pacientes con NP. El PEFV fue mayor en el EP que en NP. LTE4 fue mayor en NP que en EP. No se encontraron diferencias de los niveles de CC16 en ambos grupos. Montelukast redujo la célula predominante en ambos subgrupos, mientras que budesonida sólo redujo los eosinófilos en EP. Tanto budesonida como montelukast redujeron PEFV en EP, pero no en NP. El nivel de CC16 aumentó significativamente en el EP luego del tratamiento antiinflamatorio. En conclusión: se identificó un subgrupo de asmáticos NP que presentan una menor labilidad bronquial, la vía de los leucotrienos parece estar involucrada y responde al tratamiento anti-leucotrienos. Este fenotipo muestra una escasa recuperación del nivel de CC16 posterior al tratamiento.
Palabras clave: Asma; Neutrófilos; CC16; Budesonida; Montelukast
Bronchial asthma, an increasingly prevalent disease worldwide, is characterized by activation of inflammatory mediators and local infiltration of inflammatory cells, such as the eosinophil which is considered to be a main protagonist in asthma pathophysiology. However, daily management of asthmatic patients reveals often discordance between the clinical manifestations and the treatment response. This fact appears to be associated with the existence of varying patterns of inflammatory cells and mediators that require a specific diagnosis and a differential pharmacological treatment.
There is accumulating evidence demonstrating that asthma also occurs with neutrophils as the major inflammatory cell. The occurrence of neutrophils in bronchial secretion has been associated mainly with severe asthma15; neutrophils have also been associated with less severe astha6-9, but these reports did not clarify if neutrophils might actually be a main protagonist in asthma because a strict selection of steroid-naïve and non-smoking patients has not be taken into consideration in these studies. Previous evidences by Gabrijelcic et al10 have shown that platelet-activating factor, a precursor of leukotriene, may be involved in the pathogenesis of bronchial asthma inducing the sequestration of neutrophils in the lung and increment of urine LTE4 level as showed Echazarreta et al11. Therefore, cysteinyl leukotriene could be involved in the pathogenesis of neutrophilic asthma.
On the other hand, bronchiolar Clara cell of respiratory epithelium secrete 16-kD Clara cell protein (CC16) also name CC10, an inmunomodulatory protein2 that has been demonstrated to inhibit neutrophils chemotaxis.
Decreased CC16 levels have been found in serum and bronchoalveolar fluid of patients with chronic obstructive pulmonary disease13 however, the relationship between CC16 content and inflammatory cell pattern in asthma has not been evaluated.
The goal of this study was to determine the occurrence of neutrophil predominance in asthma and identified its characteristics on the basis of clinical-functional features, induced sputum cellular pattern and soluble molecules, to guide the appropriated anti-inflammatory therapy.
Material and Methods
We included male and non-pregnant female patients with mild to severe asthma from our first visit outpatient pneumonology clinic and enrolled for this study. The project was approved by the Ethics Committees of the Facultad de Ciencias Médicas, Universidad Nacional de Córdoba. All patients received detailed information on the risks and potential benefits of this study and provided written consent.
The inclusion criteria were: patients, 21 to 40-year old, with stable, mild to severe asthma according to the definition and classification of severity of National Heart, Lung, and Blood Institute/World Health Organization Global Strategy for Asthma Management and Prevention14; absence of respiratory infections, exacerbation of asthma within the preceding 6 weeks, and no previous treatment with oral or inhaled steroids or leukotriene receptor antagonists; all them were non-smokers, with no systemic or cardiopulmonary disease other than asthma. Atopy was not an entry criteria.
This is a randomized, single-blind, and parallel study. On the first visit, medical history of the patient was recorded following a standard questionnaire, and major aeroallergen skin tests and lung function tests were performed.
On the next visit, a first sample of induced sputum was obtained; selected plug's sputum samples were processed according to a validated protocol15, and the cellular fraction was separated to analyze inflammatory cells, and supernatant was stored at -70° C to further evaluate CC16 and LTE4. Patients with eosinophil/neutrophil (E/N) ratio ≥ 1.4, calculated using absolute sputum cell count and a percentage of eosinophils >3 were classified as eosinophil predominant (EP). To classify patients as neutrophils predominant (NP) two criteria were considered again: a E/N ratio ≤ 0.6, and a percentage of neutrophils ≥ 16 taking into account the percentage of neutrophils found in a previous study with a group of health voluntaries16-17 Patients with E/N ratio between 1.4 and 0.6 were not included in the study The patients were randomly assigned; following a computer-generated schedule, and received either 400 mg b.i.d budesonide inhaled dry powder (Neumotex 400® Phoenix Argentina) or 10 mg montelukast oral tablet (Singulair®, MSD) once a day at bedtime irrespective of food for 6 weeks.
After six weeks' treatment, second sputum was collected and analyzed, and after a four-week washout period, a third induced sputum was studied (Fig. 1). Along the study period, the patients were instructed to complete a daily self-report card.
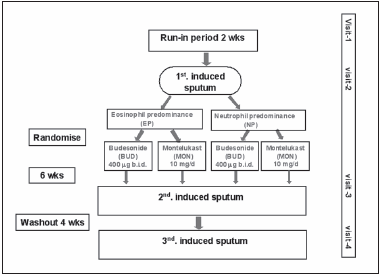
Fig. 1.- Study design. Definition of abbreviations: EP = eosinophil predominance; NP = neutrophil predominance; Wks = weeks; Bud = budesonide; Mon = montelukast.
Baseline spirometric pre-bronchodilator parameters were recorded from the best of three attempts using a Compact Vitalograph spirometer (Compact Vitalograph, Buckingham, U.K.) with measurement variations of less than 5% were considered acceptable. A baseline measurement of forced expiratory volume in one second (FEV1) was carried out according to American Thoracic Society criteria18. Spirometric measurements were performed before each sputum induction. A skin prick-test for the major aeroallergens was implemented in the first visit.
The patient daily self-report card included: A peak expiratory flow rate, a daytime symptom score (DSS) and the use of rescue beta-2 agonist (RS). The peak expiratory flow (PEF) was registered twice daily at 9:00 am and 6:00 pm. Then the PEFV was calculated from the difference between the highest and lowest daily PEF reading divided by the highest PEF value multiplied by 10019. Daytime symptom score including the daytime and night asthma symptom scale, using a range of response categories from 0 to 3: 0= null, 1= mild, 2= moderate, 3= severe, according to Santanello with modifications20. The average was calculated from the number of times the patient used an inhaled β2 agonist per day.
The concentration of CC16 was measured in sputum supernatants by enzyme-linked immunosorbent assay, employing a commercial kit (Diamed Eurogen, Belgium). The minimum detectable concentration for this method is minor than 50 pg/ml.
A additional objective of this study was to determine whether asthma phenotype can be differentiated by the level of cysteinyl leukotrienes. The concentration of leukotriene in the sputum supernatants was quantified with an enzymelinked immunosorbent assay applying a LTE4 commercial kit (Cayman Chemical, California).
Data were expressed as mean and 95% confidence intervals (CI). Descriptive statistics were used to summarize patient clinical and demographic characteristics. A generalized linear model with gamma distribution was used to analyse the two sputum cellular subsets. The group comparisons were conducted applying analysis of variance with Kruskal-Wallis test.
Wilcoxon rank tests analyses were used for between-group analyses at baseline and for the analysis of within-group treatment effect.
The appropriate sample size for both cells in each therapeutic arm was adequately powered (power 0.84%) to detect 0.30 as a minimum absolute change of eosinophil with the treatment, with a α of 0.05. The estimation was based on eosinophils because they exhibited higher variance than neutrophils. A p < 0.05 was considered significant.
Results
A total of 43 patients were examined and 41 patients meeting the strict inclusion criteria were enrolled in two groups according to the predominant cytological profile observed in the sputum. Two were excluded because had not criteria to classify.
A total of 23/41 patients (56%) exhibited eosinophil predominance in their sputum cytology; while in 18/41 (43%) patients the neutrophil was predominant cell. Both groups showed significant statistical differences when total eosinophil and neutrophil numbers were compared (Table 1).
TABLE 1.- Patient characteristics, baseline lung function and cell countaccording to predominant cell
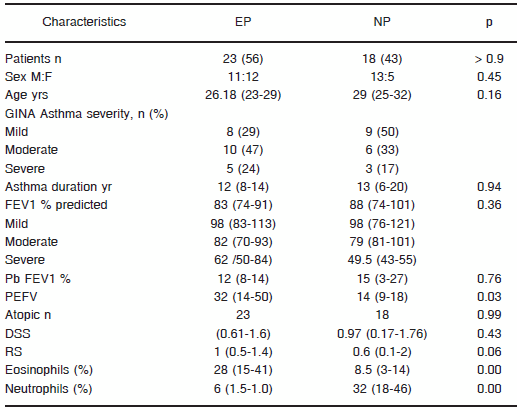
Data are presented as mean and 95% confidence intervals (CI). EP = eosinophil predominance. NP = neutrophil predominance. M = Male; F = Female; GINA = Global Initiative for Asthma; FEV1 = forced expiratory volume in one second; Pb = postbronchodilator; PEFV = peak expiratory flow variability; DSS = daytime symptoms score; RS = rescue beta-2 agonist.
The characteristics of the patients in both groups are summarized in Table 1. They show no difference in mean age and all patients demonstrated to be atopic. Although the FEV1 values in EP and NP were not statistically different, the PEFV values were significantly higher in EP in comparison to the NP group (p = 0.03).
No significant difference was found in baseline level of CC16 between the two subsets.
Thirty three of the 41 patients that started the protocol completed the treatment period. Eight patients were excluded, 6 of these from the EP group: one because of travel, two because of pregnancy before randomization, one because of starting to smoke, and two because of the occurrence of a respiratory infection between the visits. Two subjects in the NP group did not complete the protocol because of travel.
In the EP group, 17 were randomized and 9 placed in the budesonide arm and 8 in the montelukast. Eight out of 16 of the NP group were included to the budesonide arm and 8 to the montelukast. All basal subsets that emerged after randomization, demonstrated no statistical difference when comparing the different parameters here evaluated (not shown).
When analyzing functional respiratory parameters, budesonide and montelukast reduced the PEFV only in the EP group (p = 0.002). Budesonide but not montelukast improved significantly DSS in both EP and NP (p = 0.002) and RS in both EP (p = 0.0001) and in NP patients (p = 0.002) (Table 2 A-B).
TABLE 2.- Clinical and functional characteristics of patients before and after budesonide and montelukast.
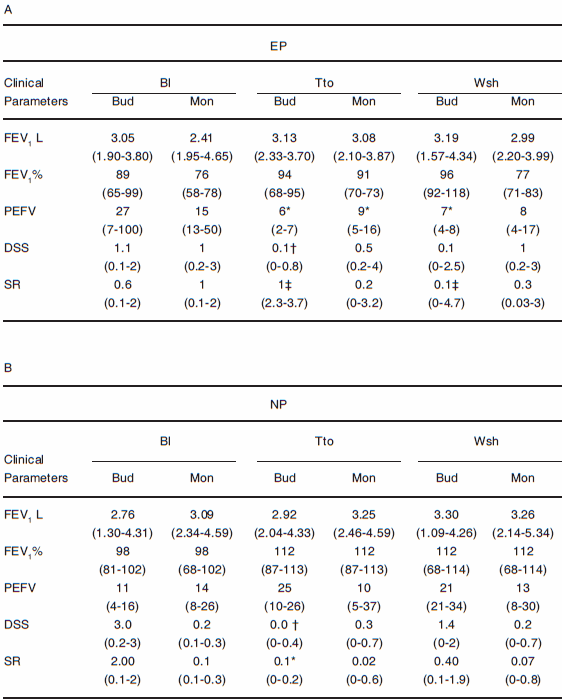
A. EP: Eosinophil Predominance. B. NP: Neutrophil Predominance. Data are presented as mean with (95% CI). BL = baseline. Tto = treatment period; Wsh = washout period, PEFV = Peak expiratory flow rate variability; DSS = Daytime symptoms score; SR = short-acting ß agonist rescue. Bud = budesonide; Mon = montelukast; *:p = 0.0021 compared with BL; †: p = 0.0121 compared with BL; ‡: p = 0.0001, compared with BL.
Budesonide significantly reduced the numbers of eosinophils in EP (p = 0.01) and raised the neutrophils (p = 0.04). Montelukast significantly reduced eosinophils in EP (p = 0.04) and neutrophils in NP (p = 0.01) (Fig. 2). After the washout period, eosinophil numbers remained low in EP compared with the baseline value (p = 0.04), but neutrophils in NP group returned to baseline values when treated with montelukast (p = 0.4) (Fig. 2).
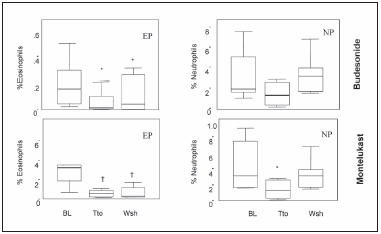
Fig. 2.- Budesonide and mMontelukast effects on cell percentage. Data are presented as mean and 95% CI. EP = eosinophil predominance; NP = neutrophil predominance; BL = baseline Tto = treatment; Wsh = washout; Bud = budesonide; Mon = montelukast. *: p = 0.01 compared with BL; †: p = 0.04 compared with BL.
After six weeks of treatment a significantly increased level of CC16 was found only in EP (p = 0.03) considering the total treated samples in each subset (Fig. 3).
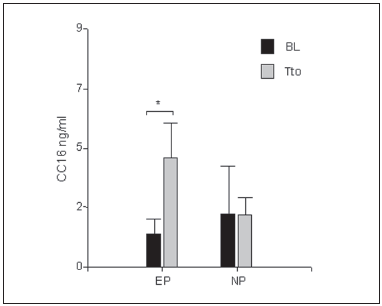
Fig. 3.- CC16 levels in induced sputum supernatant according to predominant cell subset before and after whole treatment. Data are presented as mean with 95% CI. EP = eosinophil predominance; NP = neutrophil predominance; BL = baseline; Tto = treatment period, *: p = 0.05.
Regarding the effects of montelukast on neutrophils, we analyzed the level of LTE4 in supernatant of baseline induced sputum, and found that it was higher in NP than in the EP subset (p = 0.03) as shown in Fig. 4.
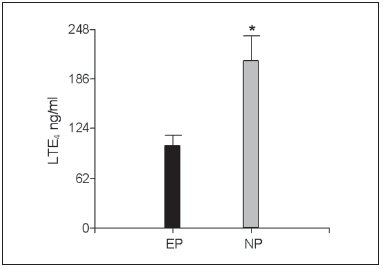
Fig. 4.- Baseline levels of LTE4 of sputum supernatant according predominant cell subset. Values are presented as mean ± SEM. EP = eosinophil predominance. NP = neutrophil predominance *: p = 0.03.
Discussion
In the present study, a neutrophil-predominant subset of stable asthmatic patients was characterized and differentiated from the "classic" eosinophilic asthma. This group showed a lower bronchial lability than eosinophilpredominant group; it exhibited higher leukotriene levels and responded to leukotriene modifier treatment. Only eosinophils predominant group was able to increase epithelial CC16 anti-inflammatory protein after treatment.
Eosinophils in sputum represent a distinctive feature of asthma; however, eosinophilic inflammation alone does not explain the heterogeneity of the disease observed in the daily management of asthmatic patients21, suggesting the existence of alternative inflammatory patterns involving other cell types and chemical mediators as major protagonists. Therefore, their specific diagnoses appear to be critical for a differential pharmacological treatment. A main contribution of the present report is the finding of neutrophils as the major inflammatory cell in a 38% of a strictly selected asthmatic population.
Increase of neutrophils in bronchial lavage was associated to severe asthma22, 23, to chronic asthma8 and to exposure to low molecular weight agents in occupational asthma24. Although neutrophils have also been associated with less severe asthma6-9, in most of these studies the selection of patients was not homogeneous and the critical inclusion criteria such as age, smoking, length of asthma, and the use of inhaled steroids that may per se increase the number of neutrophils, were not taken into consideration. In consequence, in the specialized bibliography25 a standard criterion for classification of neutrophilic asthma has yet to be clearly established.
The population of stable neutrophilic predominant asthmatics identified here, exhibited no differences in FEV1 values compared with the EP subset; however, the PEFV was higher in EP than in NP. In this respect, Virchow26 showed that the level of eosinophil cationic protein in sputum correlates with parameters of airflow hyperactivity.
In our study we have corroborated the effects of budesonide and montelukast in depleting the number of eosinophils as described by others9. However, an important novel observation is that montelukast was able to deplete neutrophils while budesonide did not modify their numbers. It is difficult to explain this montelukast´s effect on neutrophils only through its antagonism of cysteinyl leukotriene receptor without direct effects on LTB4 levels10. A recent publication27 described montelukast as having a specific inhibiting effect on 5-lipoxigenase enzyme and it can thus inhibit the chemotaxis of neutrophils via LTB4. Considering NP group response to cysteinil leucotrien, we evaluated LTE4, the last metabolite of cysteinyl leukotriene, and found it to be significantly higher in this subset, probably associated to its physiopathogenic. The finding that the neutrophil population returned to baseline values after montelukast treatment washout suggests that this inflammatory phenotype is not a transient condition.
Although both treatments reduced the numbers of inflammatory cells, it is important to stress that only budesonide and not montelukast improved DSS and SR, a common finding in clinical practice. Perhaps it results from multiple mechanisms of action of budesonide.
The finding that CC16 baseline levels showed no differences between the groups, indicating a similar inflammatory state due in part to Clara cell metaplasia to mucous cells and the consequent depletion of CC16 content, as has been demonstrated in experimental asthma models28, 29.
The increase of CC6 in EP group after anti-inflammatory treatment could be the result of mucous metaplasia reversion recovering their normal morpho-functional status as was demonstrated by electron microscopy28.
The deficient response of NP patients to anti-inflammatory treatments suggests that the primary defect could lie in the decline Clara cell population or in their secretory capacity30, 31. The lack of secretor response to increase CC16 value is a disadvantage for NP subset.
A recent report32 emphasized the importance of identifying factors which predict the development of severe asthma. In this respect, NP could correspond to an asthma phenotype with a poor prognosis. This hypothesis is supported by the work of Ohchi et al33 who demonstrated that CC16 low expression influences negatively and predicts the risk of progression of the disease in sarcoidosis. These observations reinforced the protector and modulator role of the CC16 in the inflammatory mechanism of the respiratory tract.
One of the major weaknesses of this study was the lack of a control group; however the strict inclusions criteria and ethical considerations prevented us to include a control group. However, the differences found in the two different therapeutic arms let us affirm they were due to the specific effect of the anti-inflammatory treatments and not to a regression to the mean.
The results presented here demonstrate a clearly-defined neutrophil predominate subset in asthma, with distinct clinical-functional characteristics and specific response to treatment. Leukotriene pathway appeared to be involved in the pathofysiology. The anti-inflammatory CC16 protein in the respiratory tract may constitute a useful biomarker for asthma prognosis.
Acknowledgements: The authors thank Elena Pereyra for her technical assistance and Department of Allergy and Immunology, Córdoba Hospital, for referring asthmatic patients.
This study was supported by Grant Boehringer-Ingelheim from the Asociación Argentina de Medicina Respiratoria; Grant PEI 1923/03 from the Consejo National de Investigaciones Científicas y Técnicas (CONICET) and Grant PICT from FONCyT-ANPCyT.
Agustín Aoki and Cristina Maldonado are members of the CONICET scientific career.
Conflict of interest statement: None to declare.
1. Wenzel SE, Szefler SJ, Leung DY, et al. Bronchoscopic evaluation of severe asthma. Persistent inflammation associated with high dose glucocorticoids. Am J Respir Crit Care Med 1997; 156: 737-43. [ Links ]
2. Wenzel SE, Schwartz LB, Langmack EL, et al. Evidence that severe asthma can be divided pathologically into two inflammatory subtypes with distinct physiologic and clinical characteristics. Am J Respir Crit Care Med 1999; 160: 1001-8. [ Links ]
3. Turner MO, Hussack P, Sears MR. Exacerbations of asthma without sputum eosinophilia. Thorax 1995; 50: 1057-61. [ Links ]
4. Fahy JV. Prominent neutrophilic inflammation in sputum from subjects with asthma exacerbation. J Allergy Clin Immunol 1995; 95: 843-52. [ Links ]
5. Sur S, Crotty TB, Kephart GM, et al. Sudden-onset fatal asthma. A distinct entity with few eosinophils and relatively more neutrophils in the airway submucosa? Am Rev Respir Dis 1993; 148: 713-9. [ Links ]
6. Gibson PG, Jodie L, Simpson BS, et al. Heterogeneity of Airway Inflammation in Persistent Asthma. Evidence of Neutrophilic Inflammation and Increased Sputum Interleukin- 8. Chest 2001; 119: 1329-36. [ Links ]
7. Gordon P, Boulet LP, Malo JL, et al. Assessment and evaluation of symptomatic steroid-naive asthmatics without sputum eosinophilia and their response to inhaled corticosteroids. Eur Respir J 2002; 20: 1364-9. [ Links ]
8. Green RH, Brightling CE, Woltmann G, et al. Analysis of induced sputum in adults with asthma: identification of subgroup with isolated sputum neutrophilia and or response to inhaled corticosteroids. Thorax 2002; 57: 875-9. [ Links ]
9. Jayaram L, Pizzichini E, Lemière C, et al. Steroid naive eosinophilic asthma: anti-inflammatory effects of fluticasone and montelukast. Thorax 2005; 60: 100-5. [ Links ]
10. Gabrijelcic J, Acuna A, Profita M, et. al. Neutrophil airway influx by platelet-activating factor in asthma: role of adhesion molecules and LTB4 expression. Eur Respir J 2003; 22: 290-7. [ Links ]
11. Echazarreta AL, Rahman I, Peinado V, et al. Lack of systemic oxidative stress during PAF challenge in mild asthma. Respir Med 2005; 99: 519-23. [ Links ]
12. Pilon AL. Rationale for the development of recombinant human CC10 as a therapeutic for inflammation and fibrotic disease. In: A.B. Mukherjee and B. Chilton, editors. New York Academy of Sciences, Volume on CC10 proteins 2000; p 1-18. [ Links ]
13. Pilette C, Godding V, Kiss R, et al. Reduced epithelial expression of secretory component in small airways correlates with airflow obstruction in chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2001; 163: 185-94. [ Links ]
14. Global strategies for asthma management and prevention, National Institutes of Health, National Heart, Lung, and Blood Institute. NIH Publication No 2-3659. 2002. In: http://www.ginasthma.com. Last updated: continuous. [ Links ]
15. Efthimiadis A, Pizzichini E, Pizzichini MMM, et al. Sputum Examination for Indices of Airway Inflammation: Laboratory Procedures. Ed. Astra. Canadian Thoracic Society 1997; 1-31. [ Links ]
16. Uribe Echevarría E, Pérez P, Bonaterra M, et al. Safety, reproducibility and validity of induced sputum technique. Archivos de Alergia e Inmunologia Clinica 2003; 34: 41-6. [ Links ]
17. Pizzichini E, Pizzichini MMM, Efthimiadis A, et al. Indices of airway inflammation in induced sputum: reproducibility and validity of cell and fluid phase measurements. Am J Respir Crit Care Med 1996; 154: 308-17. [ Links ]
18. American Thoracic Society (statement). Standardization of spirometry- Update. Am Rev Respir Dis 1987; 136: 1285-98. [ Links ]
19. Lim S, Jatakanon A, John M, et al. Effect of inhaled budesonide on lung function and airway inflammation. Assessment by various inflammatory markers in mild asthma. Am J Respir Crit Care Med 1999; 159: 22-30. [ Links ]
20. Santanello NC, Barber BL, Reiss TF, et al. Measurement characteristics of two asthma symptom diary scales for use in clinical trials. Eur Respir J 1997; 10: 646-51. [ Links ]
21. Simpson JL, Scott RJ, Boyle MJ, et al. Differential proteolytic enzyme activity in eosinophilic and neutrophilic asthma. Am Respir Crit Care Med 2005; 172: 559-65. [ Links ]
22. Jatakanon A, Uasuf C, Maziak W, et al. Neutrophilic inflammation in severe persistent asthma. Am J Respir Crit Care Med 1999; 160: 532-9. [ Links ]
23. Ordoñez CI, Shaughnessy TE, Matthay MA, et al. Increased neutrophil numbers and IL-8 levels in airway secretions in acute severe asthma: clinical and biologic significance. Am J Respir Crit Care Med 2000; 161: 1185-90. [ Links ]
24. Lemière C, Chaboillez S, Malo JL, et al. changes in sputum cell counts after exposure to occupational agents: what do they mean? J Allergy Clin Inmunol 2001; 107: 1063-8. [ Links ]
25. Pavord ID, Sterk PJ, Hargreave FE, et al. Clinical applications of assessment of airway inflammation using induced sputum. Eur Respir J 2002; 20: 40-3. [ Links ]
26. Virchow JC Jr, Holscher U, Virchow C Sr. Sputum ECP levels correlate with parameters of airflow obstruction. Am Rev Respir Dis 1992; 146: 604-6. [ Links ]
27. Ramiers R, Caiaffa MF, Tursi A, et al. Novel inhibitory effect on 5-lipoxygenase activity by the anti-asthma drug montelukast. Biochem Biophys Commun 2004; 324: 815-21. [ Links ]
28. Roth FD, Quintar AA, Uribe Echevarria EM, et al. Budesonide effects on Clara cell under normal and allergic inflammatory condition. Histochem Cell Biol 2007; 127: 55-68. [ Links ]
29. Evans CM, Williams OW, Tuvim MJ, et al. Mucin is produced by Clara cells in the proximal airways of antigen- challenged mice. Am J Respir Cell Mol Biol 2004; 31: 382-94. [ Links ]
30. Shijubo N, Itoh Y, Yamaguchi T, et al. Clara cell protein- positive epithelial cells are reduced in small airways of asthmatics. Am J Respir Crit Care Med 1999; 160: 930-3. [ Links ]
31. Shijubo N, Itoh Y, Yamaguchi T, et al. Serum levels of Clara cell 10-kDa protein are decreased in patients with asthma. Lung 1999; 177: 45-52. [ Links ]
32. The ENFUMOSA study group. The ENFUMOSA cross-sectional European multicentre study of the clinical phenotype of chronic severe asthma. Eur Respir J 2003; 22: 470-7. [ Links ]
33. Ohchi T, Shijubo N, Kawabata I, et al. Polymorphism of Clara Cell 10-kD Protein gene of sarcoidosis. Am J Respir and Crit Care Med 2004; 169: 180-6. [ Links ]
Recibido: 7-12-2010
Aceptado: 27-6-2011














