Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Archivos argentinos de pediatría
versión impresa ISSN 0325-0075
Arch. argent. pediatr. vol.110 no.5 Buenos Aires oct. 2012
ARTÍCULO ORIGINAL
Variabilidad de la actividad física en niños chilenos de 4 a 10 años: estudio por acelerometría
Variability of physical activity in 4 to 10-year-old children: a study by accelerometry
Dr. Claude Godarda, Lic. Melissa Románb, Lic. María del Pilar Rodríguezb, Mg. Bárbara Leytona, Dra. Gabriela Salazara
a. Instituto de Nutrición y Tecnología de Alimentos. Universidad de Chile. Santiago, Chile.
b. Escuela de Nutrición y Dietética. Universidad Santo Tomás. Viña del Mar, Chile.
Correspondencia: Dr. Claude Godard: cgodard@inta.cl
Conflicto de intereses: Ninguno que declarar.
Recibido: 2-2-2012
Aceptado: 16-5-2012
http://dx.doi.org/10.5546/aap.2012.388
RESUMEN
Introducción. Frente a los populares cuestionarios, la acelerometría entrega una información más confiable de la actividad física. Así, el objetivo ha sido documentar la variabilidad de la actividad física de niños chilenos en relación con edad, sexo, estado nutricional y días de la semana, y determinar cuántos de ellos cumplen con la recomendación de tener actividad física moderada y vigorosa por más de una hora diaria.
Población y métodos. Ciento nueve (109) escolares de 4-10 años de edad (67 niños, 42 niñas) llevaron un acelerómetro durante 2, 3 o 4 días consecutivos. Treinta eran obesos (IMC >P95 por edad y sexo). En cada sujeto, los niveles de actividad física fueron expresados en cuentas por minuto (cpm) y promedios (DE) de cpm/hora. La actividad física moderada y vigorosa se definió por la suma diaria de cpm >900.
Resultados. La actividad física diurna tuvo un promedio de 21 697 (662) cmp/hora con variabilidad considerable de un niño a otro, y de un momento a otro del día en un mismo niño. Las cpm/hora individuales estaban significativamente asociadas con actividad física moderada y vigorosa (R= 0,954). Se encontraron diferencias entre niñas y niños (p <0,01) y entre obesos y no obesos (p <0,01). No hubo diferencia entre < 6 años y > 9 años (p= 0,12). Entre semana y fin de semana hubo una leve diferencia. Cincuenta y seis de 67 (83,6%) niños y 24 de 42 (57,1%) niñas cumplieron con la recomendación de realizar actividad física moderada y vigorosa por más de 60 minutos diarios.
Conclusión. Existe déficit de actividad física en escolares chilenos menores de 10 años, particularmente en niñas y en obesos.
Palabras clave: Niños escolares; Actividad física; Acelerometría; Obesidad.
SUMMARY
Introduction. When compared to popular questionnaires, accelerometry provides more reliable information regarding physical activity. Thus, the objective has been to document the variability of physical activity in Chilean children in relation to age, gender, nutritional status and days of the week, and to determine how many of them meet the recommendation for moderate to vigorous physical activity for more than an hour a day.
Population and methods. One hundred and nine (109) school children aged 4-10 (67 boys, 42 girls) wore an accelerometer for 2, 3 or 4 consecutive days. Of them, 30 were obese (BMI >95th percentile by age and gender). In each subject, levels of physical activity were expressed in counts per minute (cpm) and means (SD) of cpm/hour. Moderate to vigorous physical activity was defined by the daily sum of cpm >900.
Results. Daytime physical activity had a mean of 21,697 (662) cpm/hour with considerable variation from one child to another, and from one time of the day to another in the same child. Individual cpm/hour was significantly associated to moderate to vigorous physical activity (R = 0.954). Differences were found between girls and boys (p < 0.01) and between obese and non-obese children (p < 0.01). There were no differences between children <6 years and >9 years (p = 0.12). There was a slight difference between weekdays and weekends. Fifty-six (56) of 67 boys (83.6%) and 24 of 42 girls (57.1%) met the recommendation for moderate to vigorous physical activity for more than 60 minutes a day.
Conclusion. There is a physical activity defcit in Chilean school children under 10 years, particularly in girls and obese kids.
Key words: School children; Physical activity; Accelerometry; Obesity.
¿Para qué repetir los errores antiguos habiendo tantos errores nuevos que cometer?
Bertrand russell
INTRODUCCIÓN
El grado de actividad física es extremadamente variable de un niño a otro; es función de factores genéticos, de la edad, del sexo, de las condiciones climáticas, de las acciones depromoción existentes, además de la situación social, cultural y económica de la familia, entre otros. En el contexto del aumento global del sedentarismo-característico de nuestra época- los niños son menos activos que en décadas pasadas en condiciones de vida normal. Esto reviste importancia pues la obesidad infantil se ha convertido en un problema mayor de salud en los niños chilenos y porque la inactividad física es un factor determinante del sobrepeso.1,2
En los últimos años, esencialmente en EE.UU. y Europa, se han multiplicado los estudios que analizan la actividad física de los niños, ya sea por: a) calorimetría indirecta o medición de agua doblemente marcada (considerados como patrón de referencia, pero poco apropiados para estudios en terreno, es decir, estudios epidemiológicos); b) por cuestionarios y recordatorios; y, sobre todo, por c) sensores de movimiento, específicamente, los acelerómetros.3 Todas las publicaciones coinciden en que los varones son más activos que las mujeres y los obesos menos activos que los no obesos.
En Chile, los datos se han obtenido esencialmente mediante cuestionarios.4-6 En 2006, un cuestionario sencillo de actividad física habitual asociado con un puntaje de 0 a 10 fue validado en niños de 8 a 13 años, mostrando buena concordancia con la acelerometría.7 En otro trabajo, de Vásquez y cols.,8 se comunicó la actividad física acelerométrica de niños obesos de 3 a 5 años.
La acelerometría, un método objetivo, no reactivo y relativamente fácil de usar, permite cuantificar el movimiento en cualquier momento y detecta diferentes niveles de actividad física, desde la sedentaria hasta la vigorosa. Frente a la amplia cantidad de publicaciones de actividad física en niños con acelerómetros a nivel internacional, y a la recomendación de que los niños deberían dedicar un mínimo de una hora al día en actividades moderadas y vigorosas,9-11 nos parece adecuado seguir midiendo la actividad física de niños chilenos con esta técnica práctica y bien tolerada por los escolares. Un proyecto piloto del Instituto de Nutrición y Tecnología de Alimentos (INTA) de Chile sobre prevención de obesidad en escolares12 nos dio la oportunidad de estudiar la actividad física por acelerometría de niños de 4 a 10 años, con el objetivo de documentar su variabilidad y el cumplimiento de recomendaciones en esta materia.
POBLACIÓN Y MÉTODOS
Los sujetos del presente estudio fueron elegidos por conveniencia debido a limitaciones materiales, como una submuestra tomada de los 586 alumnos de 4 a 10 años que participaban en un proyecto piloto del INTA. Este último, publicado por Kain y cols.12 y titulado "Prevención de obesidad en preescolares y escolares de escuelas municipales de una comuna de Santiago de Chile: proyecto piloto 2006", consistía en la implementación de una intervención educativa a largo plazo a nivel de alumnos y profesores.
El presente estudio fue aprobado por el Comité de Ética del INTA y se desarrolló entre abril y julio de 2006. El protocolo fue explicado a los padres, quienes firmaron un consentimiento informado.
Antropometría: Peso y talla fueron medidos con balanza SECA de precisión 0,1 kg y 0,1 cm para evaluar el índice de masa corporal (IMC). La obesidad fue calificada en caso de IMC =P95 por sexo y edad, de acuerdo con el referente CDCNCHS 2002.
Protocolo: El día jueves en la mañana, al entrar a la jornada escolar y junto con la antropometría, se colocaron los acelerómetros Actiwatch AW64 fijados con un cinturón semielástico sobre la cadera derecha. Los cinturones fueron retirados el lunes siguiente al retorno a clases.
Acelerometría: El Actiwatch AW64 mide 27 x 25 x 9 mm y pesa 16,3 g. Este dispositivo miniaturizado consiste en un traductor piezoeléctrico y un microprocesador que transforma las aceleraciones multidireccionales en señales cuantitativas, que son registradas en la memoria. Los resultados se expresan en cuentas por minuto (cpm). Para considerar un registro de actividad en vigilia como válido se requirió un mínimo de 7,5 h. Siguiendo la recomendación internacional,13 los períodos de cpm igual a cero durante más de 20 minutos fueron excluidos, pues podría el escolar haberse retirado el cinturón. Para el total de los días y para cada día separadamente, la suma de cpm se dividió por el número de horas registradas; se obtuvo así un valor promedio de "cpm/hora". Una reducción similar de datos ha sido empleada por Page y cols.14 y por Pate y cols.15 para uniformizar valores acelerométricos muy disimiles en días y horas/día.
En cada sujeto se calculó también el tiempo empleado en diferentes niveles de intensidad de la actividad física. La cantidad de minutos diarios con cpm >900 se calificó como actividad física moderada y vigorosa según la clasificación de Puyau y cols.,16 y se determinó, por tanto, el número de sujetos que tenían actividad física moderada y vigorosa por 60 minutos o más al día.
Para la actividad física nocturna, se seleccionaron todos los registros que mostraban actividad (cpm >25), durante más de 60 minutos a partir de las 21 h.
Estadística: Los datos fueron procesados mediante Stata 11. Se consideró significativo un p <0,05. Se realizó la prueba de Shapiro-Wilk para verificar la normalidad de los datos, y las diferencias fueron determinadas por la prueba de la t (Student) y ANOVA utilizando la prueba post hoc de Scheffe. Para asociación de datos cuantitativos se usó la correlación de Pearson y para datos cualitativos se empleó la prueba de X2.
RESULTADOS
Ciento veintiocho niños y niñas de 4 a 10 años ingresaron al estudio. Diecinueve fueron excluidos por tener registros diarios incompletos (menos de 7,5 h), fallas técnicas del Actiwatch o abandono después de un día. Los 109 casos restantes se analizaron, 38 con cuatro días de registro (de jueves a domingo) y 26 casos con tres días (de jueves a sábado). Cuarenta y cinco casos tuvieron solo dos días válidos de acelerometría (días variados); sin embargo, se aceptó su incorporación al análisis porque el promedio de horas diarias registradas y de cpm/hora no fue significativamente diferente de los casos con tres o cuatro días de registro.
Los resultados de estos 109 casos se presentan en las Tablas 1, 2 y 3 y la Figura 1. Se encontró que las cpm/hora individuales tuvieron una estrecha asociación con actividad física moderada y vigorosa/día: R= 0,954 (Pearson).
Tabla 1. Valores acelerométricos de actividad física de los 109 participantes (promedio, DE)

Tabla 2. Valores acelerométricos de actividad física: variación según la edad (promedio, DE)

Tabla 3. Valores acelerométricos de actividad física según el estado nutricional (promedio, DE)

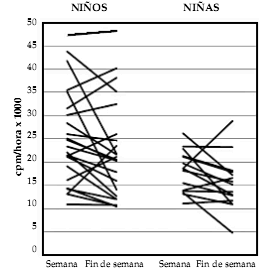
Figura 1. Comparación de las cpm/hora de días de semana (jueves y viernes) con días de fin de semana (sábado y domingo) en 15 niñas y 23 niños (promedios de dos días)
En la Tabla 1 se muestra la cantidad de valores promedio de cpm/hora, actividad física moderada y vigorosa (minutos/día) y cantidad de sujetos con =60 minutos/día de actividad física moderada y vigorosa, con diferencia significativa entre niños y niñas. Las actividades físicas individuales en vigilia exhibieron una variabilidad considerable de un sujeto a otro: la diferencia entre el mayor y el menor valor obtenidos fue de 42 017 cpm/hora.
Como lo describe la Tabla 2, la edad no tuvo influencia sobre la actividad física, pero se detectó una leve tendencia a la baja entre las categorías extremas "<6 años" y ">9 años".
En la Tabla 3, la actividad física se clasifica según el estado nutricional, con diferencia significativa de cpm/hora y actividad física moderada y vigorosa (minutos/día) entre el estado nutricional normal y los obesos. Los 30 niños obesos fueron menos activos que los 63 de estado nutricional normal.
En la Figura 1 se compara la actividad física (cpm/hora) de los días jueves y viernes con la de los días sábado y domingo, en los 38 niños que registraron cuatro días seguidos. Se observa que existe una gran variabilidad individual, con muchos niños y niñas que bajaron su actividad física el fin de semana, mientras otros la subieron. En promedio, la actividad física bajó levemente, pero significativamente (p <0,001), el fin de semana: cpm/hora= 16 210 (8694) contra 22 249 (7743) durante la semana. Sin embargo, hubo cierta correlación entre semana y fin de semana, tanto en el grupo total (R= 0,64) como en los niños (R= 0,66), pero mucho menos en niñas (R= 0,26).
Durante uno a cuatro días, 88 alumnos (53 niños, 35 niñas) fueron a acostarse después de las 22 h; 52 de ellos lo hicieron después de las 23 h, 23 de los cuales lo hicieron después de medianoche. Entre todos ellos, se sumó un total de 184 h "nocturnas", para las cuales la actividad física fue de 17 072 (12 071) cpm/hora. Los días viernes y sábados fueron un poco más activos, pero la diferencia con los días jueves y domingo no fue significativa.
DISCUSIÓN
En este estudio (uno de los primeros en nuestro subcontinente) se mostró que la actividad física de escolares menores de 10 años tiene una importante variabilidad de un sujeto a otro. La información obtenida, objetiva y no reactiva, ha permitido determinar adecuadamente si los niños estudiados cumplían la recomendación de realizar actividad física moderada y vigorosa por más de una hora diaria. Además, al contrario de los cuestionarios, la acelerometría entregó información sobre actividad física durante prácticamente la totalidad del tiempo de vigilia.
Los resultados del presente estudio deben ser interpretados con prudencia, dado el tamaño relativamente pequeño de la muestra. Durante los últimos años se han publicado trabajos de actividad física por acelerometría con mucho más sujetos, hasta más de mil niños, como en el estudio de Nyberg y cols.17 Sin embargo, otros trabajos relevantes comunican un número de casos similar al nuestro.14,18,19
Por otra parte, hemos analizado registros diarios de actividad física de solo dos a cuatro días, habiendo establecido tres días como pauta inicial; sin embargo, los valores de cpm/hora en registros de dos días no fueron significativamente diferentes de los recolectados en mayor número de días. Según Trost y cols., un mínimo de siete días sería necesario para estimar adecuadamente la actividad física habitual de niños, pero, en menores de 10 años, cuatro días podrían ser suficientes.13 Futuros estudios de actividad física en nuestro país serán posibles con empleo de sensores de movimiento por 7 días o más, y con una precaución relativa en la selección de sujetos y familias, sin dejar de tener en cuenta las dificultades en familias de escasos recursos.
De la muestra inicial de 128 participantes, 19 fueron excluidos, lo que representa un 14,8%, valor similar al de un trabajo nuestro anterior, que fue de 17,2%.7 Con períodos de acelerometría prolongados, estas cifras pueden ser considerablemente superiores, como en la publicación de Van Coevering y cols., en EE.UU.20 donde se ha comunicado una deserción de hasta el 55% con, incluso, una pérdida notable de sensores.
Como era de esperar, nuestros resultados muestran que los niños son más activos que las niñas y los escolares obesos son menos activos que los no obesos, lo cual confirma los numerosos datos de la bibliografía mundial. No se observó que la actividad física decline entre los 5 y los 10 años, como ha sido comunicado recientemente en niños y niñas suecas, tanto durante días de escuela como en fin de semana.17 La diferencia entre niños chilenos y niños suecos de las mismas edades (de confirmarse por trabajos futuros) podría explicarse por diferentes hábitos y tradiciones educativas y culturales: en Chile se realizan más juegos libres fuera de casa, menos actividades programadas, tal vez incluso una menor cantidad de horas de clase. Janssens11 ha delineado cómo, entre la edad preescolar (desde los 2 años) y la adolescencia (hasta 16-18 años), lo esencial de la actividad física pasa progresivamente de una actividad libre, espontánea, basada en juegos y conquista de habilidades motoras, a una actividad dirigida, programada con deportes y estudios. La transición parece ser más tardía en niños chilenos que en niños suecos. Por otra parte, los niveles globales de actividad física podrían elevarse entre los 3 y 8 años, como sugiere otro informe del mismo país escandinavo,21 aunque parezca contradictorio con lo anterior.
En la muestra estudiada, la actividad física es globalmente poco diferente entre la semana (días de escuela como jueves y viernes) y el fin de semana, pero con grandes variaciones individuales, tanto en niñas como en niños. En menores de 10 años, hay estudios que han comunicado más actividad física el fin de semana,18,22 menos actividad17 o actividad física similar.19,23 Estas diferencias podrían estar relacionadas con las circunstancias particulares en las cuales se hicieron los registros (estación, hábitos familiares, etc.). La tendencia a menor actividad física el fin de semana se generaliza realmente a partir de los 10-11 años.17,22
Por otra parte, en estos escolares, se evidenció una actividad física apreciable en horas de la noche, pasadas de las 22 h, aunque los datos no sean concluyentes por desconocerse los detalles sobre la ocupación en estas horas nocturnas. Lo que sí puede señalarse es que la pauta de vigilia de estos escolares difiere de la de los niños europeos del norte, cuyo horario para acostarse es más estricto (alrededor de las 21 h).
Finalmente, la acelerometría ha permitido determinar, con mayor exactitud que los cuestionarios, la cantidad de niños que dedican, en promedio, más de 60 minutos al día en actividades moderadas y vigorosas.9-11 Un número apreciable de escolares alcanzó esta meta: 73,4% en total, y hasta 83% en los varones, porcentajes que son superiores a los de niños chilenos de más edad, en los que fue de solo 62%.7 Sin embargo, en comparación, un 93% de niños hispanoamericanos de Texas y 85% de niñas entre 4 y 8 años tienen una actividad física moderada y vigorosa mayor de 60 minutos diarios, en concordancia con la recomendación anglosajona para niños y adolescentes de entre 6 y 18 años.24
Un estudio realizado en tres países europeos (Dinamarca, Estonia y Portugal) concluyó que los niños que realizan un promedio de 90 minutos diarios en actividad física moderada y vigorosa logran tener menor riesgo cardiovascular (medido por un conjunto de siete factores) y una mejor salud.25 Sesenta minutos no sería suficiente según estos autores. Sin embargo, el objetivo de 90 minutos puede parecer utópico y desalentador desde una perspectiva conductual, y la meta de 60 minutos parece ser más realista y alcanzable en las actuales condiciones.11
Actualmente, existe menos confianza en los cuestionarios para evaluar la actividad física de niños y adolescentes, cualquiera que sea el modelo o instrumento. Varios metaanálisis de trabajos sobre cuestionarios, particularmente los autoinformes e informes aproximados, se han publicado recientemente y ponen seriamente en duda su fiabilidad.26-28 En nuestro país, se requieren nuevos estudios de la actividad física objetiva, en niños y adolescentes de todas edades, con registros acelerométricos de mayor cantidad de días (que creemos factibles), con un mayor número de participantes, incluidas variables como nivel socioeconómico, estación y clima, y tomando en cuenta posibles modelos de intervención en curso. Un estudio de este tipo, permitirá comparaciones apropiadas con datos internacionales y recomendaciones para la niñez chilena.
CONCLUSIÓN
La actividad física individual de escolares chilenos menores de 10 años es extremadamente variable. Las niñas son menos activas que los niños y los obesos menos activos que los no obesos. Ochenta y tres de los alumnos (pero solo 57% de las niñas) cumplen con la recomendación de tener actividad física moderada e intensa -la más saludable- por más de una hora al día.
Agradecimientos
A los niños, sus padres y autoridades escolares por su valiosa colaboración, a la Tecnóloga Médica Alyerina Anziani y la Secretaria Jacqueline Marchant por su ayuda técnica y a la International Atomic Energy Agency (IAEA) por su apoyo logístico.
1. Burrows R, Díaz E, Sciaraffia V, Gattas V, et al. Hábitos de ingesta y actividad física en escolares, según tipo de establecimiento al que asisten. Rev Med Chile 2008;136:53-63. [ Links ]
2. Burrows R, Burgueño M, Gattas V, Barrera G, et al. Características biológicas, familiares y metabólicas de la obesidad infantojuvenil. Rev Med Chile 2001;129:1155-62. [ Links ]
3. Sirard JR, Pate RR. Physical activity assessment in children and adolescents. Sports Med 2001;31:439-54. [ Links ]
4. Kain J, Vio F, Leyton B, Cerda R, et al. Estrategia de promoción de la salud en escolares de educación básica municipalizada de la comuna de Casablanca, Chile. Rev Chil Nutr 2005;32:126-32. [ Links ]
5. Olivares S, Kain J, Lera L, Pizarro F, et al.. Nutritional status, food consumption and physical activity among Chilean school children: a descriptive study. Eur J Clin Nutr 2004;58:1278-85. [ Links ]
6. Olivares S, Bustos N, Lera L, Zelada ME. Estado nutricional, consumo de alimentos y actividad física en escolares mujeres de diferente nivel socioeconómico de Santiago de Chile. Rev Med Chile 2007;135:71-8. [ Links ]
7. Godard C, Rodríguez MP, Díaz N, Lera L, et al. Valor de un test clínico para evaluar actividad física en niños. Rev Med Chile 2008;136:1155-62. [ Links ]
8. Vásquez F, Salazar G, Andrade M, Vásquez L, et al. Energy balance and physical activity in obese children attending day-care centers. Eur J Clin Nutr 2006;60:1115-21. [ Links ]
9. Biddle S, Sallis J, Cavill N. Health Education Authority. Londres: 1998.Págs.3-16. [ Links ]
10. Strong WB, Malina RM, Blimkie CJ, Daniels SR, et al. Evidence-based physical activity for school-age youth. J Pediatr 2005;146:732-7. [ Links ]
11. Janssen I. Physical activity guidelines for children and youth. Appl Physiol Nutr Metab 2007;32:S109-S121. [ Links ]
12. Kain J, Concha F, Salazar G, Leyton B, et al. Prevención de obesidad en preescolares y escolares de escuelas municipales de una comuna de Santiago de Chile: proyecto piloto 2006. Arch Latinoam Nutr 2009;59:139-146. [ Links ]
13. Trost SG, Mciver KL, Pate RR. Conducting accelerometerbased activity assessment in feld-based research. Med Sci Sports Exerc 2005;37:S531-S543. [ Links ]
14. Page A, Cooper AR, Stamatakis E, Foster LJ, et al. Physical activity patterns in nonobese and obese children assessed using minute-by-minute accelerometry. Int J Obes 2005;29:1070-6. [ Links ]
15. Pate RR, Pfeiffer KA, Trost SG, Ziegler P, et al. Physical activity among children attending preschools. Pediatrics 2004;114:1258-63. [ Links ]
16. Puyau MR, Adolph AL, Vohra FA, Butte NF. Validation and calibration of physical activity monitors in children. Obes Res 2002;10:150-7. [ Links ]
17. Nyberg G, Nordenfelt AM, Ekelund U, Marcus C. Physical activity patterns measured by accelerometry in 6- to 10-year-old children. Med Sci Sports Exerc 2009;41:1842-8. [ Links ]
18. Metcalf BS, Voss LD, Wilkin TJ. Accelerometers identify inactive and potentially obese children (EarlyBird 3). Arch Dis Child 2002;87:166-7. [ Links ]
19. Trayers T, Cooper AR, Riddoch CJ, Ness AR, et al. Do children from an inner city British school meet the recommended levels of physical activity? Results from a crosssectional survey using objective measurements of physical activity. Arch Dis Child 2006;91:175-6. [ Links ]
20. Van Coevering P, Harnack L, Schmitz K, Fulton JE, et al. Feasability of using accelerometers to measure physical activity in young adolescente. Med Sci Sports Exerc 2005;37:867-71. [ Links ]
21. Dencker M, Andersen NB. Health-related aspects of objectively measured daily physical activity in children. Clin Physiol Funct Imaging 2008;28:133-44. [ Links ]
22. Trost SG, Pate RR, Freedson PS, Sallis JF. Using objective physical activity measure with youth: How many days of monitoring are needed? Med Sci Sports Exerc 2000;32:426-31. [ Links ]
23. Treuth MS, Hou N, Young Dr, Maynard LM. Accelerometry-measured activity or sedentary time and overweight in rural boys and girls. Obes Res 2005;13:1606-14. [ Links ]
24. Butte NF, Puyau MR, Adolph AL, Vohra FA et al. Physical activity in nonoverweight and overweight Hispanic children and adolescents. Med Sci Sports Exerc 2007;39:1257-66 [ Links ]
25. Andersen LB, Harro M, Sardinha LB, Froberg K, et al. Physical activity and clustered cardiovascular risk in children: a cross-sectional study (The European Youth Heart Study). Lancet 2006;368:299-304. [ Links ]
26. Ekelund U, Tomkinson G, Amstrong N. What proportion of youth are physically active? Measurements issues, levels and recent time trends. Br J Sports Med 2011;45:859-65. [ Links ]
27. Chinapaw MJ, Mokkink LB, Van Poppel MN, van Mechelen W, et al. Physical activity questionnaires for youth: a systematic review of measurement properties. Sports Med 2010;40:539-63. [ Links ]
28. Farias Junior JC, Lopes Ada S, Florindo AA, Hallal PC. Validity and reliability of self-report instruments for measuring physical activity in adolescents: a systematic review. Cad Saude Publica 2010;26:1669-91. [ Links ]














