Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Archivos argentinos de pediatría
versión impresa ISSN 0325-0075
Arch. argent. pediatr. vol.110 no.6 Buenos Aires dic. 2012
ORIGINAL ARTICLE
Professional burnout in pediatric intensive care units in Argentina
María Eugenia Galván, MDa, Juan C. Vassallo, MDa, Susana P. Rodríguez, MDa, Paula Otero, MDc, María Mercedes Montonati, MDa, Gustavo Cardigni, MDa, Daniel G. Buamscha, MDb, Daniel Rufach, MDb, Silvia Santos, MDb, Rodolfo P. Moreno, MDb, Mariam Sarli, MDb y Members of the Clinical and Epidemiological Research Group in Pediatric Intensive Care Units - Sociedad Argentina de Pediatría
a. Hospital Nacional de Pediatría "Prof. Dr. Juan P. Garrahan". Buenos Aires, Argentina.
b. Comité Nacional de Emergencias y Cuidados Críticos. Sociedad Argentina de Pediatría.
c. Pediatric Information Technology Work Group. Sociedad Argentina de Pediatría.
E-mail Address: María E. Galvan, MD: eugegalvan31@gmail.com
Funding: "Fundación Garrahan" Research Grant and Ramon Carrillo Arturo Oñativia Initiation Scholarship granted by the Health Research Committee (Comité Nacional Salud Investiga) of the Ministry of Health; both grants facilitated the inclusion of research scholars during the development process.
Conflict of Interest: None.
Received: 4-17-2012
Accepted: 6-4-2012
http://dx.doi.org/10.5546/aap.2012.466
SUMMARY
Introduction. There is currently a deficiency of physicians in pediatric intensive care units (PICU). The cause of this deficit is multifactorial, although the burnout phenomenon has been described as relevant.
Objective. To analyze the situation of human resource in the pediatric intensive care units in Argentina and measure the level of burnout.
Methods. An observational cross-sectional study through surveys administered electronically; the Maslach Burnout Inventory was used. Physicians that work at public o private pediatric intensive care units in Argentina during at least 24 hours per week were invited to participate.
Results. A total of 162 surveys were completed (response rate 60%). We observed a high risk of burnout in emotional exhaustion in 40 therapists (25%), in fulfillment in 9 (6%), and depersonalization in 31 (19%). In combination, 66 professionals (41%) had a high risk of burnout to some extent; there were independent protective factors of this risk as to be certified in the specialty (ORA 0.38, 95% CI 0.19 to 0.75) and work in public sector PICU (ORA 0.31, 95% CI 0.15 to 0.65), while working more than 36 hours/week on duty increased the risk (ORA 1.94, 95% CI 1.1 to 3.85). Additionally, 31% said that they did not plan to continue working in intensive care, and 86% did not think to continue with on call duties in the following years. Over 60% of respondents reported that changes in professional practice (salary, staff positions, early retirement, fewer loads on call) could prolong the expectation of continuing activities in PICU.
Conclusions. A significant percentage of doctors working in the PICU of Argentina have a high risk of burnout syndrome and a low expectation of continuing in the field.
Key words: Pediatric intensive care units; Burnout; Human resources.
INTRODUCTION
Critical care refers to the medical care of patients suffering from severe, unstable or acute conditions.1 In Argentina, pediatric intensive care has become a certified pediatric subspecialty since 1997.2 The presence of physicians trained in critical care improves the survival of patients and reduces health costs. Additionally, human resource deficiencies in these units increase morbidity and mortality.3
We are currently facing a deficiency of physicians trained to work in the PICU. The specialty of pediatric intensive care has been indicated as a priority in the training need by areas of human resources. Internationally, the Committee on Manpower for Pulmonary and Critical Care Societies (COMPACCS),4 details that future demand for critical care services in the United States will soon exceed the capacity of the current delivery system. In 2007, the Sociedad Argentina de Terapia Intensiva warned the community on the need to double the number of intensive care specialists, which meant incorporating 700 professionals to meet the demand. In recent years, however, no vacancies have been covered for the training of these specialists.
The causes for which physicians leave the PICU are multiple; the professional burnout5-8 has been described as one of the relevant factors for this.
The term burnout, according to Freudenberger,9 is defined as "exhaustion of energy experienced by professionals when they feel overwhelmed by the problems of others." More recently, Maslach and Jackson10,11 defined it as "a response to chronic work stress whose components are an emotional and/or physical exhaustion syndrome, low working productivity, and excessive depersonalization."7
There are reports indicating that half of the pediatric intensivists would suffer burnout,12 while no published works exist in Argentina. The PICU survey conducted by the Argentine Association of Pediatrics in 2005 partially reflects this.2
The objective of this work was to analyze the situation of human resources at the PICUs of Argentina, through a systematic survey of the characteristics and opinions of physicians working in these units. Specifically, the objectives were to: a) describe the characteristics of physicians working at PICUs; b) identify their level of training, professional development, and work condition; c) measure the level of burnout ; d) explore opinions on continued employment, and e) discuss possible associations between the variables analyzed and the presence of burnout.
POPULATION AND METHODS
This is an observational cross-sectional study conducted using surveys administered systematically, voluntarily and confidentially.
All physicians working in health-care at public or private PICUs of Argentina that met the inclusion criteria of having a PICU care load equal to or higher than 24 hours per week and who provided their consent for the record and survey during the months assigned to data collection (May 2010 to June 2011) were invited to participate.
Different strategies were used to identify candidates for the survey: lists of scientific societies, lists of specialty conferences, networks, previous multicenter studies, and requests to heads of department of Argentine PICUs to refer staff data. A database was prepared based on these listings, and then duplicates or erroneous data were later eliminated.
The instrument for collecting prospective data was a self-administered survey comprised of 3 sections: 1) introduction to fundamentals, objectives, confidentiality agreement and request to complete it voluntarily; 2) list of questions to collect the study variables; and 3) burnout questionnaire (Maslach Burnout Inventory, MBI).13-16
A pilot test was performed; this consisted of delivering the survey to 20 intensivists, who were evaluated for their understanding of the survey and for reliability of the technical process for submission and reception. Variables explored included demographic features (sex, age, marital status, children, place of residence), aspects related to training in pediatric intensive care and to professional development; additionally, employment characteristics and level of professional satisfaction were collected.
For the assessment of burnout, the Maslach Burnout Inventory-Human Services Survey (MBI-SS) questionnaire was used, which is considered the classic MBI version (Maslach and Jackson, 1986).11 It consists of three scales to measure the frequency with which professionals perceive emotional exhaustion (the professional feels he cannot give more of himself or herself, both emotionally and affectionately), depersonalization (development of negative attitudes or feelings towards patients, dehumanized view of the patient), and low personal fulfillment (negative self-assessment, belief that nothing can change occupationally nor is it worth trying). This scale consists of 22 items divided into 3 sub-scales that explore personal fulfillment in 8 items, emotional exhaustion in 9 and depersonalization in 5; subjects assess each item on a Likert-type scale, indicating how often they have experienced the situation described in the question in the last year. In the emotional exhaustion scale, a score of ≥27 represents a high level of burnout; for depersonalization, a score of >9 means high level; the personal fulfillment scale has a meaning opposite to the above, so that, <33 points is considered high personal fulfillment and >39, low.
The research protocol was approved by the Ethics and Institutional Review Committees of the Hospital de Pediatría "Prof. Dr. Juan P. Garrahan."
Codes were used for data processing, thus securing their confidentiality. Characteristics of the professionals were compared according to level of burnout; for this analysis, professionals having at least a high risk level in some of the subscales explored were considered at high risk of burnout. T, Mann Whitney U or Fisher's exact tests were employed for the bivariate analysis, as appropriate. With the final result of high risk of burnout, a manual model of logistic regression was built to evaluate independent risk or protection factors for burnout; the construction of the model was conducted including those factors with an association equal to or less than p= 0.10; interactions and collinearity were explored. Calibration of the model was assessed with a Hosmer-Lemeshow test. The significance level was established in <0.05 and the statistical package for data processing was Stata 10.0 for Windows.
RESULTS
A total of 162 surveys were completed (60% response) The main characteristics of the group are shown in Table 1.
Table 1. Characteristics of intensivist pediatricians who responded to the survey
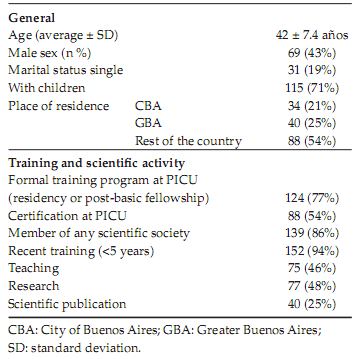
On average, physicians had been working in the PICU during the last 11 ± 7.5 years, with values ranging from 1 to 32 years; in 94 cases (58%), the professional had less than 10 years of seniority. There were 40% of professionals working in a single institution, 39% in two, and 21% in three or more facilities. Most physicians (96%) said they were working in units that met conditions for tertiary care. Half of them carried out their activity in the public and private sector, 61 (38%) in the public sector, and 19 (12%) exclusively in the private sector. Regarding the characteristics of the positions held at the PICU with the highest work load, 49 (30%) were heads at the PICU and 77 (47%) had staff functions; however, 38 physicians (23%) performed only on call duty activities.
A high percentage (89%) regularly performed on-call duties and, in 66 cases, the weekly on-call load was superior to 36 hours. Regarding the employment contract relationship, 119 (74%) had staff positions, while the rest (26%) worked under temporary contracts or for professional fees.
There was a 65% (110) of professionals who disagreed totally or partially with their remuneration, and 69% (112) considered they would choose this specialty again; 31% stated they had no plans to continue with PICU activity, and 86% had considered not to continue with on-call duties in the following years. Figure 1 shows the opinions on continuity in the specialty and performing oncall duties, according to seniority expressed as ordinal categories for years of work at PICU, and it was observed that even those physicians with few years of seniority did not plan to continue or perform on-call duties in the future.
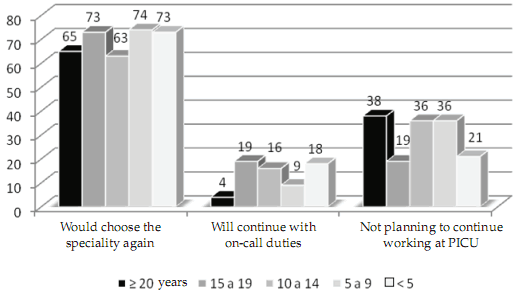
Figure 1. Opinions of intensivist pediatricians according to their seniority in specialty (% of positive responses)
Additionally, the questionnaire explored whether there were conditions that they considered would strengthen their continuity in this activity: A total of 93% (152) mentioned improving remunerations, 70% indicated early retirement, and 62% (101) responded that reducing on-call duty load and/or increasing staff activity were modifications that would impact positively on continuity.
Measurement of the burnout scale showed the following results: for the sub-scale of emotional exhaustion, the average value was 20 ± 9.97 points, and 25% (40) of the professionals presented a high risk of burnout; in relation to the personal fulfillment sub-scale, the value was 30 ± 7.15 points, with 6% (9) of the professionals with a high risk of burnout; finally, for the depersonalization sub-scale, the value was 5.7 ± 4.8 points, with 19% (31) of the intensivists at high risk. If we consider combined data, we find that 66 professionals (41%) had a high risk of burnout in some dimensions or sub-scales. Figure 2 shows the number of professionals for each burnout risk group (low, intermediate, and high) in each sub-scale.

Figure 2. Number of professionals according to risk level in each sub-scale of the Maslach Burnout Index.
The high risk of burnout in the "personal fulfillment" dimension was independent of the high risk in the other 2 scales (none of the 9 high-risk cases had emotional exhaustion or depersonalization at that risk level). In contrast to this, a significant association was observed between personal exhaustion and depersonalization: 35% of the cases of high risk in emotional exhaustion also had high depersonalization risk (p= 0.003).
Table 2 compares the professionals' characteristics according to a high risk of burnout, and it is observed that those with children and more seniority in the profession had less risk; on the contrary, being single was associated to a greater risk. Tables 3 and 4 show the academic and employment aspects of physicians according to the presence of burnout; being certified and working in the public sector reduced the risk, while performing only on-call duties and doing over 36 hours of weekly on-call duty was associated to a greater risk.
Table 2. Comparison of professionals' characteristics according to presence of high risk of burnout

Table 3. Comparison of academic aspects according to presence of high risk of burnout

Table 4. Comparison of employment aspects according to presence of high burnout risk

The multivariate analysis allowed estimating that being certified in the specialty (ORA 0.38, 95% CI 0.19-0.75) and working at the PICU in the public sector versus the private sector (ORA 0.31; 95% CI 0.15-0.65) were protective and independent factors for burnout, while doing on-call duties for more than 36 hours a week increased such risk (ORA 1.94, 95% CI 1.1-3.85).
DISCUSSION
The results from this study show a high level of burnout and work dissatisfaction among the intensivist pediatricians surveyed. Pediatricians from all country districts are reflected in this study. In this field, other reports have estimated a similar prevalence.6 In contrast to the work conducted by Pistelli et al., for general pediatricians, which include staff interns,7 the average values of burnout observed in our work were lower regarding emotional exhaustion (20 versus 30.6) and personal fulfillment (30 versus 35.7), but higher for depersonalization (5.7 versus 0.5); in that study, no differences were observed for pediatricians performing tasks at the PICU, though this sub-group could have been under-represented. Also, seniority in the profession was associated with greater personal fulfillment and less depersonalization.
Our study is focused exclusively in pediatricians who are intensivists, and while the greater number of years working in the specialty seemed to be protective against the risk of global burnout, this association was not maintained in the multivariate analysis.
The results of the Maslach scale may be compared through the arithmetic means of scores obtained by subjects for each of the three subscales (emotional exhaustion, depersonalization and personal fulfillment) or positioning them in the corresponding ranges of high, medium or low burnout predefined for each sub-scale.11 The scales should not be added up, since each of the three parameters uses a different score system, even of a different sign: ones are positive (more points, more burnout) and one is negative (more points, less burnout). Another way to compare the results is to count the percentage of individuals studied who have a high score for a certain subscale. Despite there is no global level of burnout, some authors refer to a high level of burnout for those subjects with at least one high scale.17,18 The importance of the definition lays in the comparability of the results with those of other works. We decided to adopt this form of analysis to characterize risk globally, since high risk in any of the scales means an alert for the professional. Thus, high risk of burnout occurred in 41% of the respondents, which implies an alarming diagnosis. Figures of burnout close to 38% in pediatric oncologists have been recently published, in which younger professionals presented greater frequency of burnout.19
Different variables haven been proposed as predisposing factors for burnout: gender, prolonged working hours and little sleep, among others. The situation of young professionals seems to be a risk factor some studies agree on, which is worrying for the future of the specialty. In a study conducted in Buenos Aires, the prevalence of burnout among resident physicians was of 20%, with a high component of emotional exhaustion and depersonalization.20 In our study, physicians with less seniority had greater tendency to present a higher risk of burnout; additionally, they showed a high percentage of dissatisfaction and very low expectation of continuing to work in a PICU, which will probably aggravate the human resource crisis in this sector. In our population, having more years of specialty practice could have a protective effect on the occurrence of burnout.
Dissatisfaction in medical practice has been related to various factors: managed care, legal aspects, greater patient expectations, or differences in the doctor-patient relationship. As Ceriani indicates in a recent editorial,21 there is a worrying situation of frustration and lack of motivation behind all these factors.
In our study, 80% of the professionals had no expectation of continuing to work in the specialty in the future. This situation appears to have gotten worse in the last years; a work published in 1998 reported that 55% of intensivist pediatricians surveyed in Argentina were dissatisfied with their job.8
Employment conditions and the number of on-call duties are associated to the risk of burnout. In our study, working in the private sector or performing on-call duties for more than 36 hours per week is associated to professional exhaustion. Similar situations were reported in adult intensivists in a recent survey by the Colegio Argentino de Terapia Intensiva.22 This survey described that more than half of respondents practiced only as on-call physicians performing an average of more than 48 hours of on-call duties a week.
Most professional respondents believe that implementing a few measures related to the professional practice, such as early retirement, 12 hours of on-call duties, bonus for intensive care, among others, would improve expectations to continue working at the PICU.
Weaknesses of our work are related to that 40% of the surveys were not answered and to the fact that we cannot disregard the fear of personal identification, which could have influenced the answers.
CONCLUSIONS
About 40% of physicians that work at a PICU in Argentina have a high level of burnout; few have expectations to continue working in the area, and less than 15% consider continuing with on-call duties in the following years.
Being certified in the specialty and working in a public sector PICU were protective and independent factors to burnout, while having more than 36 hours of weekly on-call duties increased such risk.
Changes in the professional practice could prolong the expectation of respondents to develop health-care activities at the PICU.
ANNEX

Acknowledgments
To Virginia Sphers, MD, for her contribution in the review of the research protocol.
1. Ewart QW, Marcus L, Gaba MM, Brandnen RH, et al. The critical care medicine crisis: a call for federal action a white paper from the critical care professional societies. Chest 2004;125(Issue 4,April). [ Links ]
2. Rufach D, Santos S, Vassallo J. Relevamiento de UCIP´s en la República Argentina. IV Congreso Argentino de Emergencias y Cuidados Críticos Pediátricos. Buenos Aires, 26-28 de mayo; 2005. [ Links ]
3. Joint commission on accreditation of Health Care Organization. Sentinel event alert preventing ventilator-related death and injuries. Washington, DC: Joint Commission; 2002. Pág.25. [ Links ]
4. Angus DC, Kelley MA, Schmitz RJ, White A, et al. Caring for the critically ill patient. Current and projected workforce requirements for care of the critically ill and patients with pulmonary disease: can we meet the requirements of an aging population? JAMA 2000;284:2762-70. [ Links ]
5. Cardigni G, Sphers V, Althabe M, et al. Burnout en terapia intensiva pediátrica en Argentina. 3° Congreso Mundial Terapia Intensiva Pediátrica. Montreal Canadá; junio 2000. [ Links ]
6. Pistelli Y, Perochena J. Síndrome de desgaste profesional en médicos pediatras. Análisis bivariado y multivariado. Arch Argent Pediatr 2011;109(2):129-34. [ Links ]
7. Cardigni G, Althabe M, Vega L. El intensivista pediátrico ejerciendo la especialidad. Arch Argent Pediatr 1998; 96:363-8. [ Links ]
8. Maslach C, Jackson S. The measurement of experienced Burnout. J Occup Behavior 1981;2:99-113. [ Links ]
9. Freudenberger HJ. Staff burn-out. J Soc Issues 1974;30(1): 159-65. [ Links ]
10. Maslach C, Jackson SE. The Maslach Burn-out Inventory. Manual Research Edition. University of California. Palo Alto: Consulting Psychologist Press; 1986. [ Links ]
11. Maslach C, Schaufeli WB, Leiter MP. Job burnout. Ann Rev Psychol 2001;52:397-422. [ Links ]
12. Fields AL, Cuendon TT, Brasseux CO, Gets PR, et al. Physician burnout in pediatric critical intensive care medicine. Crit Care Med 1995;23:1425-9. [ Links ]
13. Gil-Monte PR. Factorial Validity of the Maslach Burn-out Inventory (MBIHSS) among Spanish professionals. Rev Saúde Pública 2005;39(1):1-8. [ Links ]
14. Gil-Monte PR, Peiró JM. A longitudinal study on Burnout syndrome in nursing professionals. En: Avattone F, Arnoldd eds. Burnout (Feelings work in Europe). Quaderni di Psicologia del Lavoro. Roma: Guerini Studio. 1997;5:407-14. [ Links ]
15. Gil-Monte PR, Peiró JM. Validez factorial del Maslach Burn-out Inventory en una muestra multiocupacional. Psicothema 1999;11(3):679-89. [ Links ]
16. Redondo Granado MJ. Errores frecuentes en la comparación de resultados de estudios sobre Burnout o desgaste profesional. An Pediatr (Barc) 2005;63(4):380-1. [ Links ]
17. Prieto Albino L, Robles Agüero E, Salazar Martínez LM, Daniel Vega E. Burnout en médicos de atención primaria de la provincia de Cáceres. Aten Primaria 2002;29:249-302. [ Links ]
18. Roth M, Morrone K, Moody K, Kim M, et al. Career burnout among pediatric oncologists. Pediatr Blood Cancer 2011;57(7):1168-73. [ Links ]
19. Catsicaris C, Eymman A, Cachiarelli N, Usandivaras I. La persona del médico residente y el síndrome de desgaste profesional (Burnout). Un modelo de prevención en la formación médica. Arch Argent Pediatr 2007;105(3):236-40. [ Links ]
20. Ceriani J. La insatisfacción en la práctica médica. Arch Argent Pediatr 2011;109 (6):474-5. [ Links ]
21. Colegio Argentino de Terapia Intensiva. Realidad Laboral del intensivista de la Argentina. 20º Congreso Argentino de Terapia Intensiva. Mar del Plata 30 de septiembre al 3 de octubre de 2010. Disponible en: http://www.cati.org.ar/ fles/medicos-intensivistas-un-recurso-critico-pdf.














