Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO  uBio
uBio
Compartir
Revista argentina de microbiología
versión impresa ISSN 0325-7541versión On-line ISSN 1851-7617
Rev. argent. microbiol. v.38 n.3 Ciudad Autónoma de Buenos Aires jul./sep. 2006
G. Griemberg1*, C. T. Bautista2, M. C. Pizzimenti1, G. Orfus1, B. Alonso3, T. Fernández4, O. Cando5, L. Martínez Peralta6
1Departamento de Bioquímica Clínica, Facultad de Farmacia y Bioquímica, UBA and Hospital de Clínicas José de San Martín, UBA; 2Asociación Benéfica PRISMA, Lima, Perú; 3Hospital Francisco P. Muñiz; 4Hospital Ramos Mejía; 5Hospital Juan Fernández; 6Centro Nacional de Referencia de SIDA, Facultad de Medicina, UBA. Junín 956 (1113) Ciudad Autónoma de Buenos Aires, Argentina.
*Correspondence. E-mail: griemberg@gmail.com
ABSTRACT
A cross-sectional anonymous study of 261 STD (sexually transmitted diseases) outpatients and 288 outpatients from other hospital departments was conducted at four major city hospitals in Buenos Aires. High prevalence of human immunodeficiency virus (HIV) (14.5%) and syphilis (30.2%) was noted. Fifty-two persons were diagnosed with both HIV and syphilis. Of the 87 HIV cases observed, 52 (59.7%) were co-infected with syphilis. Stratified analysis by gender showed that the prevalence of HIV, syphilis and HIV/syphilis co-infection was significantly (p<0.001) higher in men than women (HIV: 20.1% vs. 4.6%; syphilis: 39.3% vs. 17.4%; co-infection: 13.6% vs. 1.7%). Integrated HIV / STD intervention programs and more effective surveillance are required in Argentina.
Keywords: HIV, syphilis, co-infection, prevalence, STD, Argentina
RESUMEN
Alta prevalencia de co-infección sífilis-VIH en cuatro hospitales de la Ciudad de Buenos Aires, Argentina. Se realizó un estudio transversal no vinculante entre pacientes ambulatorios de cuatro grandes hospitales de Buenos Aires, 261 provenían de consultorios de enfermedades de transmisión sexual (ETS) y 288 de otros servicios. Se observó una alta prevalencia del virus de la inmunodeficiencia humana (VIH) (14,5%) y sífilis (30,2%). En cincuenta y dos pacientes se diagnosticaron ambas infecciones. De los 87 casos VIH, 52 (59,7%) estaban coinfectados con sífilis. El análisis estratificado por sexo demostró que la prevalencia de VIH, sífilis y coinfección VIH/sífilis fue significativamente (p<0,001) más alta en hombres que en mujeres (VIH: 20,1% vs. 4,6%; sífilis: 39,3% vs. 17,4%; coinfección: 13,6% vs. 1,7%). En la Argentina se requieren programas integrados de intervención VIH/ETS y una más efectiva vigilancia epidemiológica.
Palabras clave: VIH, sífilis, coinfección, prevalencia, ETS, Argentina
Numerous reports indicate that a history of sexually transmitted diseases (STD), including syphilis, significantly increases susceptibility to HIV (human immunodeficiency virus) infection (8). In Argentina, the number of persons living with HIV was approximately 130,000 at the end of 2003, an increase of 8% from 2001 (12). The HIV epidemic in this country is predominantly sexually transmitted (46.4% heterosexual and 19.4% men who have sex with men [MSM]), followed by transmission among injecting drug users (16.4%). The overall prevalence of syphilis is unknown in Argentina, contributing to the lack of information regarding the prevalence of HIV/syphilis co-infection. Previous studies have reported a high syphilis prevalence rate of between 5.3% and 7.7% among blood donors (9) and 3.7% among pregnant women (5).
A cross-sectional, anonymous epidemiological study was conducted among clinic attendees at four major city hospitals in Buenos Aires from July to October 2002. This study was performed in preparation for a larger study (11) to be published later. The study protocol was approved by Buenos Aires University, Code name: UBACyT B092.
After obtaining informed consent, 599 clinic attendees aged 18 or older were enrolled. Two STD clinics (Hospital de Clinicas and Hospital Muñiz) enrolled 261 (44%) volunteers. The remaining 288 (56%) individuals, who were clinically suspected of having a STD, were enrolled from two outpatient clinics (Hospital Ramos Mejía and Hospital Fernández). HIV infection was diagnosed by enzyme-linked immunosorbent assay screening (BIOKIT SA-HIV 1/2, Barcelona, Spain). All repeatedly-positive samples were confirmed by Western blot testing (HIV Blot 2, Genelabs, Singapore). The VDRL (Venereal Diseases Research Laboratory) test (Wiener Laboratorios, SAIC, Rosario, Argentina) was applied to screen for prior syphilis infection. Syphilis infection was then confirmed by passive hemaglutination assay (TPHA, Serodia-TP.PA, Fujirebio INC, Japan) and by indirect immunofluorescence test (FTA-abs, Inmunofluor Biocientifica SA, Argentina).
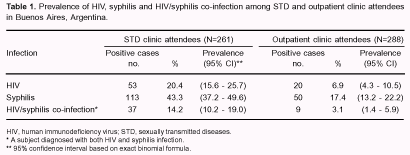
Of the 599 subjects enrolled, 51% were men, the mean age was 31 years (range 18 to 66 years). A higher number of men were enrolled at the STD clinics than at the outpatient clinics (85% vs. 29%). A total of 87 HIV cases and 181 syphilis cases were found, the overall prevalence then was of 14.5% (95% CI = 11.8 to 17.6) and 30.2% (95% CI = 26.6 to 34.1), respectively. Fifty-two (8.7%) persons were diagnosed with both HIV and syphilis. Of the observed 87 HIV cases, 52 (59.7%) of them were co-infected with syphilis. Syphilis was significantly associated with HIV infection (OR = 4.4, 95% CI = 2.8 to 7.1, p< 0.001). Stratified analysis by gender showed that the prevalence of HIV, syphilis and HIV/syphilis co-infection was significantly (p<0.001) higher in men than women (HIV: 20.1% vs. 4.6%; syphilis: 39.3% vs. 17.4%; co-infection: 13.6% vs. 1.7%). The prevalence of syphilis among HIV infected persons was almost twofold higher in men than women (67.7% vs. 36.0%, p = 0.020). In addition, there were statistically significant differences in HIV, syphilis and HIV/syphilis co-infection prevalence between STD and outpatient clinic attendees (Table 1). Of the 53 HIV cases detected among STD clinic attendees, 37 (70%) had syphilis infection, whereas of the 20 HIV cases among outpatient clinic attendees, 9 (45%) reported syphilis infection.
The main limitation of this study was the lack of information about risk behavior such as unprotected sex or drug use. Therefore, we were unable to determine the relative impact of behavioral risk factors among clinic attendees. However, we believe that these results will have important public health implications.
This epidemiological study documents the high prevalence of HIV, syphilis, and HIV/syphilis co-infection among all clinic attendees, in particular from STD clinics. Most of the STD clinic patients were anecdotally reported to be MSM, which may explain the high prevalence observed in this study (4). High rates of HIV/syphilis co-infection have been observed in recent syphilis outbreaks among MSM in urban areas, such as Seattle, Chicago, San Francisco, Los Angeles and Miami in the Unites States (1), and in European countries, such as Italy (2), Norway (6) and Ireland (7). In addition, a previous study conducted in 1995 in Buenos Aires also reported a high rate of HIV/syphilis co-infection (15.6%) in a smaller group of HIV patients (n=41) (3).
Further studies are needed in order to better define the epidemic of syphilis infection, a sensitive marker of sexual risk behaviour and a co-factor in HIV transmission. Integrated HIV/STD intervention programs and effective surveillance, e.g. panel surveys and sentinel surveillance of laboratory diagnosed infections (10), should target not only high risk groups such as MSM, but also the population at large in Argentina.
Acknowledgements: We wish to thank Drs. Jorge Benetucci, Pedro Cahn, Marcelo Losso and Ricardo Casco for the provision of the samples used in this study. We are grateful to Drs. Susan Buchbinder and Mercedes Weissenbacher for their suggestions and support. We are very thankful to the WHO/UNAIDS (grant HTP/HVI/JS) and Buenos Aires University (grant UBACyT B092) for their financial support, and to A. Sebastian for his technical assistance.
REFERENCES
1. Buchacz K, Greenberg A, Onorato I, Janssen R. Syphilis epidemics and human immunodeficiency virus (HIV). Incidence among men who have sex with men in the United States: implications for HIV prevention. Sex Transm Dis 2005; 32: S73-9. [ Links ]
2. Cusini M, Ghislanzoni M, Bernardi C, Carminati G, Zerboni R, Alessi E, et al. Syphilis outbreak in Milan, Italy. Sex Transm Infect 2004; 80: 154. [ Links ]
3. Diez MS, Nocito I, de Frade AR, Cappello SG, Guillen SM, Montero A. Serological evidence of cytomegalovirus, hepatitis B and C, Epstein-Barr virus, Toxoplasma gondii, Trypanosoma cruzi and Treponema pallidum in HIV infected patients. Medicina (Buenos Aires) 2001; 61: 378-80. [ Links ]
4. G Griemberg, (personal communication). [ Links ]
5. Griemberg G, Ravelli MR, Etcheves PC, Orfus G, Pizzimenti MC. Syphilis and pregnancy. Prenatal control, seropre-valence and false biological positives. Medicina (Buenos Aires) 2000; 60: 343-7. [ Links ]
6. Halsos AM, Edgardh K. An outbreak of syphilis in Oslo. Int J STD AIDS 2002; 13: 370-2. [ Links ]
7. Hopkins S, Lyons F, Coleman C, Courtney G, Bergin C, Mulcany F. Resurgence in infectious syphilis in Ireland: an epidemiological study. Sex Transm Dis 2004; 31: 317-21. [ Links ]
8. Royce RA, Sena A, Cates W Jr, Cohen MS. Sexual transmission of HIV. N Engl J Med 1997; 336: 1072-8. [ Links ]
9. Schmunis GA, Zicker F, Segura EL, del Pozo AE. Transfusion-transmitted infectious diseases in Argentina, 1995 through 1997. Transfusion 2000; 40: 1048-53. [ Links ]
10. Slater W, Low N. Surveillance of sexually transmitted infections in primary care. Sex Transm Infect 2004; 80: 152. [ Links ]
11. Weissenbacher M, Casco R, Reboredo G, Benetucci J, Bermejo A, Losso M, et al. Prevalence of HIV and STI in five hospitals from Buenos Aires, Argentina. 8th World STI/AIDS Congress, 2003, Abstract 42, p. 112, Punta del Este, Uruguay. [ Links ]
12. World Health Organization, UNAIDS, June 2004. Report on the global AIDS epidemic, 4th global report, table of country-specific HIV/AIDS estimates and data, end 2003, June 2004; p. 189-207 (available at http://www.unaids.org/bangkok2004/GAR_html/GAR2004_00_en.htm,last accessed on 16 July 2004). [ Links ]
Recibido: 26/6/06
Aceptado: 28/8/06














