Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Odontológica Latinoamericana
versão On-line ISSN 1852-4834
Acta odontol. latinoam. vol.23 no.3 Buenos Aires dez. 2010
ARTÍCULOS ORIGINALES
Amoxicillin/metronidazole or scaling and root planing in the treatment of chronic periodontitis
Alejandra Bono1, Mabel Brunotto2
1Departament of Oral Pathology.
2Departament of Oral Biology. Faculty of Dentistry, National University of Cordoba, Argentina.
CORRESPONDENCE Dr. Mabel Brunotto Departamento de Biologia Bucal, Facultad de Odontologia Universidad Nacional de Cordoba Haya de la Torre s/n, ciudad universitaria CP 5000-Cordoba-Argentina brunottomabel@gmail.com
ABSTRACT
The aim of the present study was to evaluate the treatment with amoxicillin or metronidazole in comparison to scaling and root planing in the treatment of chronic periodontitis. Randomised clinical trials were searched in the databases MEDLINE, EMBASE, SciELO, Cochrane and Scopus from 1989 to 2010. The search started with 2895 articles.. From this initial number of articles, 10 publications were selected and included in the study according to fixed criteria. Studies included adult patients of both sexes aged between 21 and 80, diagnosed with chronic periodontitis and treated with amoxicillin and/or metronidazole or scaling and root planning. From each article, details were abstracted relating to sample size, design, sex, age, oral hygiene habits, the exposure to drug (doses, schedule), and results such as clinical effect, analysis methods, stratification variables. Conclusion: this meta-analysis showed absence of statistically significant difference between the effects studied.
Key words: Chronic periodontitis; Antimicrobial agents; Meta-Analysis.
RESUMEN
Amoxicilina/metronidazol o raspado y alisado radicular en el tratamiento de la periodontitis crónica
El objetivo del presente estudio fue evaluar el tratamiento con amoxicilina o metronidazol en comparacion con el raspado y alisado radicular en el tratamiento de la periodontitis cronica. Ensayos clinicos aleatorios se seleccionaron de las bases de datos MEDLINE, EMBASE, Scielo, Cochrane, y Scopus desde el ano 1989 a 2010. La busqueda comenzo con 2895 articulos. A partir de este numero inicial de articulos, 10 publicaciones fueron seleccionadas e incluidas en el estudio de acuerdo a los criterios fijados. Los estudios incluyeron pacientes adultos de ambos sexos, con edades entre 21 y 80 anos, diagnosticados con enfermedad periodontal cronica y tratados con amoxicilina y/o metronidazol o raspaje y alisado radicular. De cada articulo se extrajo el tamano muestral, diseno, genero y edad, habitos de higiene oral, medicacion (dosis y esquema), resultado clinico, metodo de analisis y variables de estratificacion. Conclusion: este meta-analisis mostro ausencia de significacion estadistica entre los efectos estudiados.
Palabras clave: Periodontitis cronica; Agentes antimicrobianos; Meta-Analisis.
INTRODUCTION
Periodontitis is known to be very common among the most deprived populations, especially among certain ethnic groups. In the latest WHO document, rules were agreed upon regarding equity and determinants of health, among which professional dental care is a major component for achieving and maintaining oral health1. Nevertheless, in Latin American countries, the availability of oral health services is poor in many communities that are vulnerable from a socio-economic standpoint2.
Chronic periodontitis is a multifactorial disease, caused by dental biofilm and other local and systemic factors. Adults generally suffer from chronic periodontitis associated to the presence of calculus, plaque, gingival inflammation, probing depth and clinical attachment level loss. In some cases the disease develops slowly. Factors such as tobacco, stress and systemic diseases have been described in relation to this pathology3. In clinical practice, it is well known that periodontal disease is mainly produced by bacteria, which is why the control of pathogenic microorganisms is essential for its therapy4. The goal of anti-infection therapy is to reduce the level of pathogenic microorganisms and maintain or strengthen the levels of beneficial species. The traditional therapies used in the clinical practice of periodontics, such as scaling and root planing together with gingival hygiene are not enough to heal periodontitis in a short time in a significant number of patients. One explanation for this is the complexity of the technique and the frequency of its application5.
Severe periodontitis is usually treated with antimicrobials such as tetracycline, minocycline or metronidazole6. However, chronic periodontitis is not usually treated with antimicrobials, although nowadays there are studies that report improvements by combining scaling and root planing with antimicrobial agents7. Published papers present conflicting results about antimicrobial therapy in chronic periodontitis, which is why it is necessary to determine the evidence on this issue. The aim of this work was to evaluate amoxicillin and/or metronidazole versus the application of scaling and root planing (SRP) to improve results in the therapy of chronic periodontitis.
DATA SOURCES
This study was done according to the reporting items for systematic reviews and meta-analyses PRISMA guidelines8. We conducted a meta-analysis of studies of randomized clinical trials (RCT) from the MEDLINE, EMBASE, Scielo, Cochrane and Scopus databases, between January 1989 and January 2010, in order to provide evidence of the application of antimicrobials in chronic periodontitis treatment.
STUDY SELECTION
The search was started with 2895 articles from PubMed, EMBASE, Cochrane, Scopus and Scielo databases. Those authors that did not clearly establish inclusion criteria for the patients, or in which pharmaceutical forms were different from other studies, were discarded (Fig 1). When analyzing the main requirements for selecting the papers, we observed differences in answers related to design and form of result presentation. The most important result of the studies included is a great reduction in PD and improved BOP when antimicrobial -amoxicillin and metronidazole- therapy is used in comparison to control groups.

Fig. 1: Study flowchart to select articles according to fixed criteria.
Data extraction and quality assessment
From each article, details were abstracted relating to sample size, design, sex, age, oral hygiene habits, the drug treatment (doses, schedule), and results such as clinical effect, analysis methods, stratification variables. All studies included adult patients of both sexes aged between 21 and 80 years, diagnosed with chronic disease according to the international classification criteria of periodontal disease9 and treated with amoxicillin and/or metronidazole or scaling and root planing. They are designed as RCT studies with suitably matched controls, and sample sizes from 10 to 90 subjects. Furthermore, the studies measured common clinical parameters such as bleeding on probing (BOP), plaque, probing depth (PD), and periodontal attachment level (AL). The selected studies excluded patients with systemic diseases or with syndromes, pregnant women and with indication of other medicine. To evaluate the quality of the papers, data collection was performed by two reviewers independently (Dr. G. Bono, Pernambuco University, Brazil and Mauricio Kremer, Cordoba National University, Argentina), assessing studies for inclusion in duplicate. The papers were encoded and delivered independently to each reviewer. To accept/reject articles selected by the reviewers, the Kappa coefficient estimated by the Monte Carlo method was applied, setting a value > 0.8. A search was made of combined electronic databases, and manual searches were performed of journals and published doctoral theses. Furthermore, the bibliography of all selected papers was searched to identify grey literature. Results were expressed as average } standard deviation.
RESULTS
All studies correspond to Randomized Clinical Trial design (RCT) and their characteristics are shown in Table 1. A few limitations of this study are evident, such as the sample size and the protocol scheme. The studies do not have identical indications regarding doses or time of intake of metronidazole and amoxicillin for treating periodontitis. The time varies between 7 and 14 days with the drug taken three times daily. The main doses are: metronidazole 250 mg and amoxicillin 500 mg.
Table 1: Characteristics of studies included in this meta-analysis.


The meta-analysis was performed by standardised means differences and the total effect was estimated by random effect model using the software R version 2.9.0 (www.r-project.org), package meta, using the function metacont. PB showed a value I2 = 95%, the greatest effect is obtained with the study Mointaghavi10, SMD - 4.2160 [-4.9295, -3.5025] IC 95% (Fig 2). For AL there was high heterogeneity, I2 = 81.6%, with a total effect value of 0.45 (Fig 3), and BOP showed I2 = 97%, with a total SMD -1.053 (Fig 2).

Fig. 2: Effect of antimicrobial treatment vs SRP therapy, probing depth outcomes (top). Effect of antimicrobial treatment vs SRP therapy, bleeding on probing outcomes (bottom).
In relation to plaque index, the value for I2 was 0%, showing a null effect of treatment, the greatest effect was obtained in the test Feres, 2001 with an SMD of 0.5 (Fig 3).
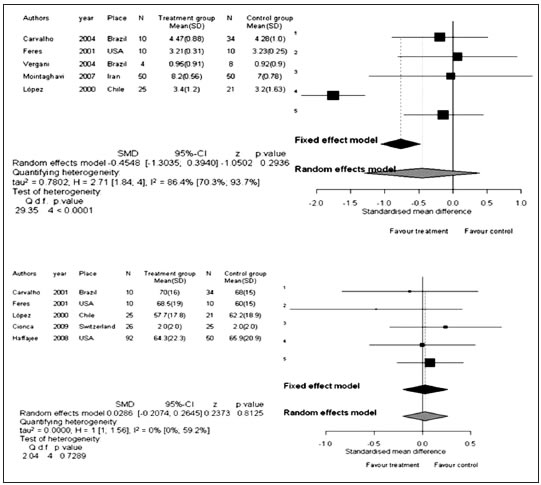
Fig. 3: Effect of antimicrobial treatment vs SRP therapy, periodontal attachment level outcomes (top). Effect of antimicrobial treatment vs SRP therapy, plaque outcomes (bottom)
DISCUSSION
Periodontal disease is one of main oral health issues, because it is the most prevalent oral pathology in several countries1. It is therefore important to evaluate alternative ways of attaining therapeutic options that will allow faster and more effective resolution than conventional therapies. The treatment of periodontal disease includes SRP therapy to reduce dental biofilm. However, studies on lipopolysaccharide (endotoxin) report that it can induce activation of macrophages to secrete lysosomal enzymes, oxygen radicals, chemokines, cytokines and prostaglandin E-2 (PGE-2), which contribute to inflammation and bone resorption11-12. The host response may be normal or pathological. In the latter case it may be due to a hyper-specific response involving T- and B- lymphocytes and production of neutralizing antibodies or not. Both the effect of bacteria and pathological host response determine destructive phenomena in periodontal tissues and the formation of pockets. This might promote a low redox potential and allow the growth of anaerobic microorganisms13. The results of this meta-analysis showed that the application of antimicrobials produces a remission of some of the clinical parameters in less time, without costly and aggressive interventions.
Cionca et al. 20097 suggested that scaling and root planing and full-mouth disinfection may reduce the need for supplementary therapies. They observed no difference in clinical parameters before treatment, but a significantly lower mean PD and BOP, which suggested the need for additional treatment. On the other hand, 6 months after treatment plus antibiotics, the average probing depth was significantly lowerin the problem group than in the control group. The conclusion of this research is that treatment with systemic metronidazole and amoxicillin significantly improved the 6-month clinical outcomes.
In addition, Matarazzo et al. 200814 showed the greatest improvements in probing depth and clinical attachment level in subjects receiving the two antibiotics together in comparison to the subjects treated with SRP alone. The investigation further showed significant reductions in the average counts and proportions of periodontal pathogens. Feres et al, 200215, concluded that metronidazole and amoxicillin are useful antibiotics because they rapidly diminish counts of putative periodontal pathogens, but must be accompanied by other procedures to bring about periodontal stability. On the other hand, authors such as Vergani Alonso et al. 200416 believe that it is not necessary to prescribe metronidazole in chronic periodontitis therapy. Haffajee et al. 200817 conclude that the therapy did not appear to create lasting changes in the percentage of resistant isolates or sites harboring resistant species. The SRP protocol is variable in the different times of the studies that enable chronic periodontitis to be resolved. There is clear evidence in these studies that antibiotics significantly reduced clinical attachment level and probing depth in patients; however, there are not many studies available for comparison, thus limiting general conclusions on the clinical benefit of the application of antibiotics. The treatment time was between 1 and 12 months. Systemic administration of metronidazole and amoxicillin, usually in conjunction with SRP allows beneficial changes in the composition of the subgingival microbiota by reducing pathogens and enables the growth of species compatible with the host. Furthermore, the combination of these drugs with a strict control of supragingival plaque during treatment of chronic periodontitis shows very promising results for treating it7.
The PD observed in other studies showed a decrease in the group of patients treated with antimicrobials, which would indicate a reduction of inflammation18-19. In regard to AL, this meta-analysis showed high heterogeneity among the studies. Evaluation of the formation of a new insertion requires a histological analysis, and thus an increase in probing attachment level after therapy does not necessarily mean that there has been a real increase in the insertion of connective tissue. It is probably due to improved health of the surrounding soft tissues that provide greater resistance to penetration of the probe20. The BOP decreased slightly in patients treated with antimicrobials which would indicate that sites with active disease decreased more than in controls (SRP). Recent studies on oral biofilm have shown that there are bacterial associations that have an impact on clinical parameters such as BOP21. The IP decreased in both treatments, leading to the disappearance of clinical signs of inflammation. Authors such as Van Dyke et al. 200822, remarked that the inflammatory response in periodontitis without a proper resolution is the cause of greater tissue destruction. In contrast Cobb, 200819 believes that the nature and magnitude of the host response that occurs in periodontal disease has an impact on the severity and rate of progression of disease and that the traditional treatment of SRP remains the “gold standard” technique for therapy of this disease, but this treatment has a high probability of relapse in the periodontal pocket. The new PD infection is due to a dental biofilm composition by tolerant microorganism residues, for which the maximum effect is achieved with the combination of SRP and locally applied antimicrobial. In relation to geographical particularities of chronic periodontitis, this meta-analysis was conducted using data from different parts of the world such as Chile, Brazil, United States, Switzerland and Iran. In general there were no differences between the geographic data. However, it is not feasible to compare the prevalence of periodontal disease around the world, and it varies with the genetics of each person. The quality of available data from developing and developed countries is not comparable, it is expected that future epidemiological investigations will elucidate this issue by appropriate and accurate methodology. Conditions of poor oral health may be due to a number of factors such as socioeconomic status and educational level, which differ between countries and within countries. These different social positions, medical conditions, jobs and economic situations and other personal situations have an impact on general and oral health, being stronger in disadvantaged communities in under-industrialized countries, who have limited resources to protect themselves23. Hence it is important to evaluate alternative ways of achieving therapeutic options that allow faster and more effective resolution than conventional ones.
When the main requirements for the selection of items were analyzed, differences were found in items related to study design and presentation of results. Most of the studies included in this metaanalysis reported results of PB and BOP reduction when antimicrobials were used for the treatment of chronic periodontitis. One limitation of this study is the sample size of the studies included, and patterns of antimicrobial management protocol. The heterogeneity of the metaanalysis is attributed to variability in participants, interventions and presentation of the outcomes (clinical heterogeneity), as well to the variability in study design and bias risk, which can be described as methodological heterogeneity24. Some of these components were observed in our study. The limitations of this study corresponded to the size of the sample and outline protocol. The studies do not contain identical information on the dose or time of intake of metronidazole and amoxicillin for the treatment of periodontitis.
Nevertheless, oral health depends on many determinants, including socioeconomic status, educational level, health systems, among others, to improve clinical outcomes reach of traditional treatment, especially considering the use of medication and/or with SRP therapy as a therapeutic strategy for the resolution of chronic periodontitis.
CONCLUSION
In conclusion, the result of this meta-analysis showed absence of statistically significant difference between the effects studied.
ACKNOWLEDGEMENTS
Doctoral Fellowship of the Science and Technology Department of National University of Cordoba (Res HCS 2276/09).
1. Blas E and Kurup AS. Equity, social determinants and public health programmes. 2010 WHO. WHO Library Cataloguing in Publication Data http://whqlibdoc.who.int/publications/2010/9789241563970_eng.pdf [ Links ]
2. Cornejo LS, Brunotto M, Hilas E. Salivary factors associated to the prevalence and increase of dental caries in rural schoolchildren. Rev Saude Publica. 2008;42:19-25. [ Links ]
3. Tanner ACR, Kent R Jr., Kanasi E, Lu SC, Paster BJ, Sonis ST, et al. Clinical characteristics and microbiota of progressing slight chronic periodontitis in adults. J Periodontol 2007;34:917-930. [ Links ]
4. Darveau RP. The oral microbial consortium’s interaction with the periodontal innate defense system. DNA Cell Biol 2009;28:359-360.
5. Haffajee AD, Socransky SS, Gunsolley JC, Systemic antiinfective periodontal therapy. A systematic review. Ann Periodontol 2003;8:115-181. [ Links ]
6. Feres M. Antibiotics in the treatment of periodontal diseases: microbiological basis and clinical applications. Ann R Australas Coll Dent Surg 2008;19:37-44. [ Links ]
7. Cionca N, Giannopoulou C, Ugolotti G, Mombelli A. Amoxicillin and metronidazole as an adjunct to full-mouth scaling and root planing of chronic periodontitis. J Periodontol 2009;80:364-371. [ Links ]
8. Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 2009;339:b2535. [ Links ]
9. Armitage G.. Periodontal diagnosis and classification of periodontal diseases. Periodontol 2000. 2004;34:9-21. [ Links ]
10. Moeintaghavi A, Talebi-ardakani MR, Haerian-ardakani A, Zandi H, Taghipour S, Fallahzadeh H, Pakzad A, Fahami N. Adjunctive effects of systemic amoxicillin and metronidazole with scaling and root planing: a randomized, placebo controlled clinical trial. J Contemp Dent Pract 2007;8:51-59. [ Links ]
11. Inagaki S, Ishihara K, Yasaki Y, Yamada S, Okuda K.Antibody responses of periodontitis patients to gingipains of Porphyromonas gingivalis. J Periodontol 2003;74:1432-1439. [ Links ]
12. Yun LW, Decarlo AA, Collyer C, Hunter N. Enhancement of Th2 pathways and direct activation of B cells by the gingipains of Porphyromonas gingivalis. Clin Exp Immunol 2003; 134:295-302. [ Links ]
13. Colombo AP, Boches SK, Cotton SL, Goodson JM, Kent R, Haffajee AD, Socransky SS, Hasturk H, Van Dyke TE, Dewhirst F, Paster BJ. Comparisons of subgingival microbial profiles of refractory periodontitis, severe periodontitis, and periodontal health using the human oral microbe identification microarray. J Periodontol 2009;80:1421-1432. [ Links ]
14. Matarazzo F, Figueiredo LC, Cruz SE, Faveri M, Feres M. Clinical and microbiological benefits of systemic metronidazole and amoxicillin in the treatment of smokers with chronic periodontitis: a randomized placebo-controlled study. J Periodontol 2008;35:885-896. [ Links ]
15. Feres M, Haffajee AD, Allard K, Som S, Goodson S, Socransky SS: Antibiotic resistance of subgingival species during and after antibiotic therapy. J Clin Periodontol 2002;29:724-735. [ Links ]
16. Vergani Alonso S, Silva EB, Vinholis AH, Marcantonio RAC. Systemic use of metronidazole in the treatment of chronic periodontitis: a pilot study using clinical, microbiological, and enzymatic evaluation. Braz Oral Res 2004;18:121-127. [ Links ]
17. Affajee AD, Patel M, Socransky SS. Microbiological changes associated with four different periodontal therapies for the treatment of chronic periodontitis. Oral Microbiol Immunol 2008;23:148-157. [ Links ]
18. Knofler G, Purschwitz, Jentsch. Evaluation of Partial- and Full-Mouth Scaling. J Periodontol 2007;78:2135-2142. [ Links ]
19. Cobb CM. Microbes, inflammation, scaling and root planing, and the periodontal condition.J Dent Hyg 2008;82:4-9. [ Links ]
20. Clinical Periodontology and Implant Dentistry. Lindhe J, Karring T, Lang NP. Cap. 2. pp.50-73., 2003. 4th ed. Blackwell Publishing Ltd. [ Links ]
21. Demmer RT, Papapanou PN, Jacobs DR Jr, Desvarieux M. Bleeding on probing differentially relates to bacterial profiles: the Oral Infections and Vascular Disease Epidemiology Study. J Periodontol 2008;35:479-486. [ Links ]
22. Van Dyke TE. The Management of Inflammation in Periodontal Disease. J Periodontol 2008;79:1601-1608. [ Links ]
23. Rylev M, Kilian M. Prevalence and distribution of principal periodontal pathogens worldwide. J Periodontol. 2008; 35:346-361. [ Links ]
24. Deek JJ and Higgins JPT. Statistical algorithms in Review Manager 5. Behalf of the Statistical Methods Group of the Cochrane Collaboration. 2007. http://www2.cochrane.org_resources_handbook_Statistical_Methods_in_RevMan5.pdf_q=resources_handbook_S tatistical_Methods_in_RevMan5 [ Links ]
25. Carvalho LH, D’Avila GB, Lea˜o A, Haffajee AD, Socransky SS, Feres M: Scaling and root planing, systemic metronidazole and professional plaque removal in the treatment of chronic periodontitis in a Brazilian population: I. Clinical results. J Periodontol 2004;31:1070-1076.
26. Feres M, Haffajee AD, Allard K, Som S, Socransky SS. Change in subgingival microbial profiles in adult periodontitis subjects receiving either systemically-administered amoxicillin or metronidazole. J Periodontol 2001;28:597-609. [ Links ]
27. Lopez NJ, Gamonal JA, Martinez B. Repeated Metronidazole and Amoxicillin. Treatment of Periodontitis. A follow up study. J Periodontolol 2000;71:79-89. [ Links ]
28. Carvalho LH, D’Avila GB, Lecao A,Goncalves C, Haffajee AD, Socransky SS, Feres M. Scaling and root planing, systemic metronidazole and professional plaque removal in the treatment of chronic periodontitis in a Brazilian population II – microbiological results. J Periodontol. 2005;32:406-411.














