Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Odontológica Latinoamericana
versão On-line ISSN 1852-4834
Acta odontol. latinoam. vol.27 no.1 Buenos Aires maio 2014
ARTÍCULOS ORIGINALES
Evaluation of bond strength between leucite-based and lithium disilicate-based ceramics to dentin after cementation with conventional and self-adhesive resin agents
Fernando J. Rigolin1, Milton E. Miranda1, Flávia M. Flório2, Roberta T. Basting3
1 Department of Prosthetic Dentistry, São Leopoldo Mandic Dental Research Institute, School of Dentistry, Campinas, SP, Brazil.
2 Department of Preventive and Social Dentistry, São Leopoldo Mandic Dental Research Institute, School of Dentistry, Campinas, SP, Brazil.
3 Department of Restorative Dentistry, São Leopoldo Mandic Dental Research Institute, School of Dentistry, Campinas, SP, Brazil.
CONTACT INFORMATION Prof. Dr. Roberta Tarkany Basting Faculdade de Odontologia e Instituto e Centro de Pesquisas Sao Leopoldo Mandic Departamento de Odontologia Restauradora - Dentistica Rua Jose Rocha Junqueira, 13-Bairro Swift Campinas - SP, 13045-755, BRAZIL E-mail: rbasting@yahoo.com
ABSTRACT
The aim of this study was to compare the microtensile bond strength of two heat-pressed ceramics (leucite-based - IPS Empress Esthetic/ Ivoclar Vivadent, and lithium disilicate-based - IPS e.max Press/ Ivoclar Vivadent) to dentin with the use of conventional and self-adhesive resin cements. The occlusal surface of 60 intact human molars was removed and the dentin was exposed. Ceramic blocks were cemented randomly with regard to the cementation systems (n=10): conventional dual resin cement (Variolink II/ Ivoclar Vivadent), conventional self-polymerizing resin cement (Multilink/ Ivoclar Vivadent), and dual self-adhesive resin cement (RelyX U100/ 3M ESPE). The dual cementation systems were photoactivated with a LED light device (Radii Cal, SDI) for 40 seconds. The specimens were sectioned to obtain sticks of approximately 1 mm2 for microtensile tests on a universal testing machine (EMIC). The type of fracture was analyzed under a scanning electron microscope. The Analysis of Variance (ANOVA) and the Tukey test (a=0.05) showed that there was no difference between types of ceramic. Average microtensile bond strength was higher for the conventional dual resin cement (Variolink II) and the self-adhesive dual resin cement (RelyX U100), despite greater prevalence of premature loss of the sticks with the latter. Average bond strength was lower when the conventional self-polymerizing resin cement (Multilink) was used. Leucite-based and lithium disilicate-based cements present similar bond strength to the dentin with conventional dual resin cement (Variolink II) and a dual selfadhesive cement (RelyX U100).
Keywords: Ceramics; Resin cements.
RESUMO
Avaliação da resistência de união entre cerâmicas a base de leucita e dissilicato de lítio à dentina após cimentação com agentes resinosos convencionais e autoadesivos
O objetivo deste estudo foi avaliar a resistencia de uniao por microtracao a dentina humana entre ceramicas prensadas (a base de leucita - IPS Empress Esthetic/ Ivoclar Vivadent, e a base de dissilicato de litio - IPS e.max Press/ Ivoclar Vivadent) apos cimentacao com agentes resinosos e convencionais e autoadesivos. As superficies oclusais de 60 molares humanos higidos foram removidas e a dentina foi exposta. A cimentacao dos blocos ceramicos foi realizada de forma aleatoria de acordo com os sistemas de cimentacao (n=10): cimento resinoso dual convencional (Variolink II/ Ivoclar Vivadent), cimento resinoso autopolimerizavel convencional (Multilink/ Ivoclar Vivadent) e cimento resinoso dual autoadesivo (RelyX U100/ 3M ESPE). Os sistemas de cimentacao duais foram fotoativados com aparelho de luz LED (Radii Cal, SDI) por 40 segundos. Os especimes foram seccionados para a obtencao de palitos com aproximadamente 1 mm2 para a realizacao do teste de microtracao em maquina universal de ensaios (EMIC). O padrao de fratura foi analisado em microscopio eletronico de varredura. A Analise de Variancia (ANOVA) e o teste de Tukey (a=0,05) mostraram que nao houve diferencas entre os tipos de ceramicas. Houve maiores medias de resistencia de uniao por microtracao para o cimento resinoso dual convencional (Variolink II) e para cimento resinoso dual autoadesivo (RelyX U100), apesar de maior prevalencia de perdas prematuras dos palitos com este cimento. Houve menores medias de resistencia de uniao ao se utilizar o cimento resinoso autopolimerizavel convencional (Multilink). As ceramicas a base de leucita (IPS Empress Esthetic) e a base de dissilicato de litio (IPS e.max Press) apresentaram resistencia de uniao semelhante a dentina ao se utilizar o cimento resinoso dual convencional (Variolink II) e o dual autoadesivo (RelyX U100).
Palavras-chave: Ceramicas; Cimento resinoso.
INTRODUCTION
With the growing demand for esthetic treatments, there has been development and improvement in the composition of ceramic and cementing systems, seeking greater mechanical strength in the materials, better bonding capacity to substrates, and enamel- like appearance.1,2 Looking to improve the mechanical properties, pressed ceramics reinforced with leucite or lithium disilicate were introduced. Their surfaces can be treated with acidic solutions to provide greater bonding capacity to adhesive cementing systems.3-5
They closely mimic natural teeth and are easier to manipulate in the laboratory since they are in the form of pellets that are injected under pressure.6 Among the types of pressed ceramics, in 2004 the Empress Esthetic system (Ivoclar Vivadent) was developed. It was composed of a vitreous ceramic reinforced with leucite which is small in size and had a more homogenous distribution due to new processing techniques that provided better mechanical properties.7 In 2006, the IPS e.max system emerged, evolving from the IPS Empress II system, composed of lithium disilicate, which has high resistance to fracture.8,9
It should be considered that proper adhesive cementing can increase resistance to fracture in the ceramic by up to 69%.10 This allows for the transmission of tension in tooth restorations, improving resistance, preventing the propagation of cracks, and increasing clinical longevity.11 Self-adhesive cements appear to facilitate the cementing technique because they minimize the clinical steps for application,12 enabling them to be used as an alternative to conventional cements,13 but they may result in lower bonding capacity of the restoration to the substrate, causing post-operative sensitivity and failure of the indirect restoration.14 Self-adhesive resin cements have a bonding mechanism provided by chelation of calcium ions by acid groups, producing a chemical bond with the hydroxyapatite of the dental structure. This is a superficial interaction and does not promote formation of a hybrid layer or resin tags in the dentinal tubules.15,16 However, conventional resin cements, due to the prior application of an adhesive system, promote the formation of a hybrid layer, enabling better bonding to the dentin substrate.17
Cementing systems can also have different activation methods for the setting reaction (self-polymers, photo-polymers, and dual polymers). Dual resin cements provide better control of the work time by the operator, and have the advantage of converting the monomers into polymers in areas where light cannot penetrate deeply to activate the setting reaction.12 Self-polymerizing cements have lower levels of resistance to flexion, modulus of elasticity, and microhardness as they take longer for polymeric to monomeric conversion18 while dual cements depend on the degree of conversion and are directly influenced by the potential for initial photoactivation. Nevertheless, self-adhesive cements that also present dual characteristics show the potential for higher chemical polymerization and greater microhardness when photoactivated.14 However, there is not yet sufficient information concerning the evaluation of bond strength of leucite-based and lithium disilicate-based reinforced ceramics to the dentin using different types of resin cements. They differ in crystalline microstructure composition, which should provide differences in bond strength, as well as the differences in adhesive strategy and setting reaction among resin cements. Therefore, the aim of this study was to compare the microtensile bond strength of two heat-pressed ceramics (leucite and lithium disilicate-based) to the dentin with the use of conventional and self-adhesive resin cements and to analyze the fracture mode. The null hypotheses to be tested were: 1) there was no difference regarding microtensile bond strength of two heat-pressed ceramics (leucite- and lithium-disilicate-based) to the dentin, regardless of the resin cement type used; 2) there was no difference regarding microtensile bond strength of ceramics to dentin when conventional and self-adhesive resin cements were used.
MATERIALS AND METHODS
Experimental design
The experimental units were 60 teeth on which flat dentin surfaces were obtained, to which ceramic blocks were cemented with resin cements. The factors studied were: a) ceramics, on 2 levels: leucitebased (Empress; Ivoclar Vivadent) and lithium disilicate-based (e.max Press; Ivoclar Vivadent); b) resin cements, on 3 levels: conventional dual resin cement (Variolink II; Ivoclar Vivadent), conventional self-polymerizing resin cement (Multilink; Ivoclar Vivadent), and dual self-adhesive resin cement (RelyX U100; 3M ESPE).
The response variable was microtensile bond strength, which was quantitatively evaluated and obtained in MPa. The experimental design for the microtensile variable was completely randomized.
Dentin Specimen Preparation
The project was submitted to and approved by the Research Ethics Committee (protocol number 2010/0039). Sixty intact human molars, without cracks or fractures and maintained in 0.1% thymol at 4oC, were sectioned transversally to remove the occlusal portion of the tooth and expose the superficial dentin. A high concentration double-sided diamond disk (model 15 LC; Buehler, Lake Bluff, Ill) mounted on a metallographic cutter (Isomet 1000; Buehler, Lake Bluff, Ill) was used under cooling at a speed of 250 rpm. Another section was made to remove the roots and expose the pulp layer. The dentin surfaces were flattened with SiC sandpaper (3M ESPE, Sumare, SP, Brazil) with a granulation of 400 to 600 grits under cooling with water in a rotating electric polisher (Aropol 2V; Arotec Ind. e Comercio, Sao Paulo, SP, Brazil). Filling the pulp layer was done incrementally with a two-step self-conditioning adhesive system (Clearfil SE Bond; Kuraray Medical, Kurashiki, Okoyama, Japan) and a photo-polymerizing nanohybrid compound resin (Evolux; Dentsply, Petropolis, RJ, Brazil).
Ceramic block preparation
Thirty leucite-based pressed ceramic blocks (IPS Empress Esthetic; Ivoclar Vivadent, Schaan, Liechtenstein) (EE) and 30 lithium disilicatebased ceramic blocks (IPS e.max Press; Ivoclar Vivadent, Schaan, Liechtenstein) (EM) measuring 6x6x5 mm were made with the hot pressing technique using a special furnace (EP 600; Ivoclar Vivadent, Schaan, Liechtenstein) following the manufacturer's instructions. When cooled, the blocks were removed from the investment material (IPSR Press Vest Investment Material; Ivoclar Vivadent, Schaan, Liechtenstein) and smoothed and polished with SiC sandpaper (240 and 320 grits) (3M-ESPE, St. Paul, Mn, USA).
The EE and EM ceramic block surfaces were conditioned with 10% fluoridic acid (Porcelain Conditioner; Dentsply, Petropolis, RJ, Brazil) for 60 sec and 20 sec, respectively, then washed for 20s and air dried. For better removal of the product residues after acidic conditioning, the blocks were submitted to an ultrasonic bath in distilled water for 4 min and dried for 20 sec. Afterwards, the silane agent (Monobond; Ivoclar Vivadent, Schaan, Liechtenstein) was applied with a disposable brush (Cavibrush; FGM, Joinville, SC, Brazil) for 1 min.
Luting Procedures
Three cementation systems were used, with the respective adhesive systems indicated (Table 1), and applied in accordance with the types of ceramic, obtaining 6 experimental groups (n=10): Group EEV - EE cemented with conventional dual resin cement (Variolink II); Group EEM - EE cemented with conventional self-polymerizing resin cement (Multilink); Group EEU - EE cemented with dual self-adhesive resin cement (RelyX U100); Group EMV - EM cemented with conventional dual resin cement (Variolink II); Group EMM - EM cemented with conventional self-polymerizing resin cement (Multilink); and Group EMU - EM cemented with dual self-adhesive resin cement (RelyX U100). The cementing agents were manipulated and used according to the manufacturers' instructions (Table 1). After application of the cementing agents, the prepared ceramic blocks were set under a standardized pressure of 1 kgf to remove excess cement and photoactivation was carried out with an LED light (RadiiCal; SDI, Bayswater, Victoria, Australia) for 10 sec on each side, with a waiting time of 10 min for chemical curing. The specimens were stored at a temperature of 37oC for 72 hours until they were cut into sticks.
Table 1: Resin cements, lot numbers, manufacturers, delivery system, composition, and application technique.
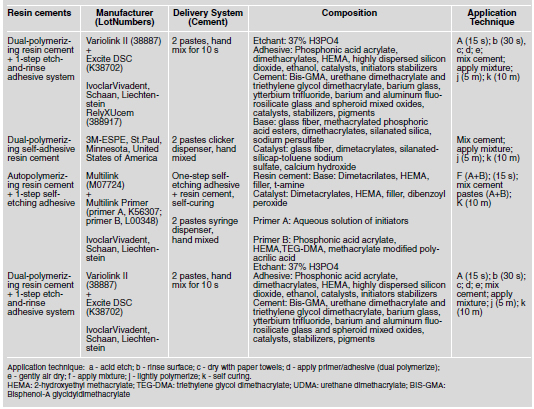
Microtensile Bond Test
The specimens were perpendicularly sectioned into slices of approximately 1 mm in width, which were then sectioned in the opposite direction, producing sticks with a cross-sectional area of approximately 1mm2. These sections were cut using a low concentration diamond disk (model 12230; Exact Corp. Enfield, Conn) at a low speed and under cooling with water. A cross-section of each stick was carefully measured with a digital caliper with resolution of 0.01 mm (Mitutoyo, Suzano, SP, Brazil) to calculate the adhesive area. The sticks obtained were set on a special device with a cyanoacrylate-based adhesive (Loctive Super Bonder; Henkel, Dusseldorf, Germany) for microtensile testing. They were positioned on a universal testing machine (DL2000; Emic, Sao Jose dos Pinhais, PR, Brazil) and submitted to tension at a speed of 0.5 mm/min. All the viable sticks were used to perform microtensile bond strength tests. The results obtained from the microtensile bond strength tests were submitted to statistical analysis. Due to the differences in the number of sticks obtained in each group, the experimental design was treated as an unbalanced factorial design. It considered the average microtensile bond strength of the sticks from each tooth as one test specimen, using the average of those sticks as an independent specimen. An exploratory analysis showed that the data could be evaluated by parametric tests due to normal distribution and the groups presented homogeneous variances, indicating the use of 2-way ANOVA and the Tukey Test, with the adopted level of significance being 5%. The analysis was carried out using the SAS statistics program (SAS Institute Inc.; Cary, NC, USA, Release 02/08/2001).
The failure modes were determined by examining the bond surfaces of the fractured specimens using a scanning electron microscope (SEM) (JSM 5900LV; JEOL Ltda., Akishima, Japan). The fractured surface was positioned in a stub and metalized with a gold/palladium layer in a sputtering machine (Bal-Tec SCD005, Liechtenstein) and viewed at magnifications of 75 × and 95 ×. The surfaces of the fractured bond were classified as: dentin adhesive (DA); ceramic adhesive (CA); mixed (M); cement cohesive (CC); dentin cohesive (DC) and ceramic cohesive (CeC). The results from the fracture type were evaluated in a descriptive manner as to frequency of distribution between the types presented.
RESULTS
Table 2 presents the frequency of specimens (teeth) and sticks lost through premature fracture before the tests and the number of viable sticks for carrying out the microtensile tests. Five specimens were lost in Group EMU and 1 was lost in Group EEV, with few sticks (10) obtained for Group EMU. The lost specimens were discarded from the data and no attempt was made to replace them. It is well documented that when statistical analysis are based on specimens that survived the specimen preparation procedures, there is an "over-evaluation" of the bond strength potential. However, when a 0-value is attributed to the specimen that prematurely fractured, the bond strength is underestimated.17
Table 2: Frequency of teeth and sticks lost and total of viable sticks according to groups.
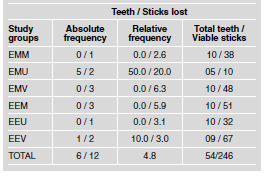
Table 3 shows that there was no statistical difference in the bond strength between ceramic types with different cementation systems (p>.05). However, there was a significant statistical difference in bond strength between the resin cements used, observing less bond strength with the conventional self-polymerizing resin cement (Multilink). There were higher bond strength averages for the conventional dual resin cement (Variolink II) and the self-adhesive cement (RelyX U100), with no statistical difference between the two.
Table 3: Standard average and deviation (MPa) of microtensile bond strength values according to ceramics and resin cements used and results of Tukey's test.
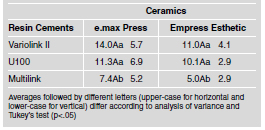
With regard to the type of fracture, it was observed that there was a predominance of the mixed-type fracture (Table 4), except for Group EEU and Group EMU, which had higher prevalence of adhesive fractures in the dentin (40% and 37.5%, respectively). Photomicrographs of the fracture types are shown in Figs. 1 through 8. Figs. 1 and 5 are representative of the mixed-type failure and portions of cement can be seen on the dentin surface, as opposed to Figs. 2 and 4, which are representative of the adhesive type failure, and the dentin surface is virtually free of cement residues on the surface. Figs. 3, 6, 7 and 8 are representative of cohesive type failures, although a great amount of cement (Fig. 3) or ceramic (Figs. 6 and 8) can be seen on the surface of dentin and ceramic fracture is clear in Fig. 7.
Table 4: Fracture type according to ceramic types and cements used.
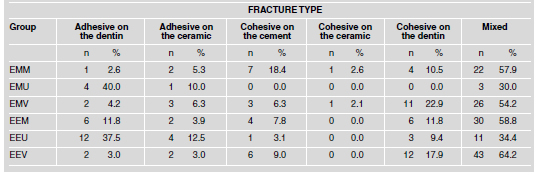

Fig. 1:Photomicrograph of surfaces of Group EEV with mixedtype fracture. A) Ceramic surface; B) Dentin surface.

Fig. 2:Photomicrograph of surfaces of Group EEU with adhesivetype fracture in dentin. A) Dentin surface; B) Ceramic surface.

Fig. 3: Photomicrograph of surfaces of Group EEM with cohesive- type fracture in cement. A) Dentin surface; B) Ceramic surface.

Fig. 4: Photomicrograph of surfaces of Group EEU with adhesive- type fracture in ceramic. A) Dentin surface; B) Ceramic surface.

Fig. 5: Photomicrograph of surfaces of Group EMM with mixed-type fracture. A) Dentin surface; B) Ceramic surface.

Fig. 6: Photomicrograph of ceramic surfaces of Group EEV with cohesivetype fracture in dentin.

Fig. 7: Photomicrograph of surfaces of Group EMV with cohesive- type fracture in ceramic. A) Dentin surface; B) Ceramic surface.

Fig. 8: Photomicrograph of surfaces of Group EEV with cohesive- type fracture in dentin. A) Dentin surface; B) Ceramic surface.
DISCUSSION
According to the results of this study, both null hypotheses were rejected. For the clinical success of ceramic restorations that adhere to the tooth, it is important to establish a perfect bond among the substrate, cement, and ceramic, allowing for clinical longevity in the restoration. Thus, when there is not an adequate bond, there can be clinical failures, leading to the fracture of ceramic restorations or failure of the bond.8 Adhesive cementation provides for a bond of indirect ceramic restorations to the dental substrate.19 In this study, ceramics were used that contained leucite crystals (Empress Esthetic) or that had a lithium disilicate base (e.max Press) which could be pretreated with fluoridic acid. This acidic solution promotes micromorphological alterations in the vitreous matrix and secondary crystalline phase of the ceramic, providing an increase in the surface area, creating microretentions,20 favoring better mechanical imbrication of the resin cement, and optimizing the bonding of the components.21,22 The association of the acidic conditioning of the ceramic with the silanization process should also be considered. It facilitates the contact with the ceramic due to bi-functional molecules, as well as providing a bond between the silica in the ceramic and the organic matrix of the resin cements by way of siloxane bonds,5,20,21 optimizing the bond strength between ceramic and cement.
According to Passos et al.,23 the application of hydrophobic adhesive on the ceramic after silanization generated less bond strength, while the nonapplication provided more stable values and greater bond strength. This increases the mechanical properties of the bond and justifies the idea of not carrying out this procedure in research.
Data from this study show that both ceramics had similar average values of bond strength for the same type of cement utilized, despite having presented different compositions (Table 1), just as Della Bona et al.4 reported greater bond strength in lithium disilicatebased ceramic than leucite-based. However, their clinical indications differed due to the differences in mechanical properties, verifying that the lithium disilicate- based ceramic (e.max Press) is stronger.8
IPS Empress Esthetic ceramic has the addition of leucite crystals that optimize the mechanical properties and prevent the propagation of cracks. It is made with pressure and heat via the hot pressing technique, increasing mechanical resistance, though not sufficiently to recommend it for creating partial permanent prostheses.6,24 However, the IPS e.max Press system, in addition to being made using the same technology as the previous system, has the addition of lithium disilicate crystals which, after the pressing and sintering process of their microstructure, contain a large quantity of long crystals (60% in volume). This is different from the leucite crystals, which are smaller in volume and grant greater flexural strength and resistance to fracture because of the spatial configuration of their crystalline grid. This system is recommended for permanent prostheses of up to three elements and single crowns.1,24,25
The choice of the resin cementation system for adhesive cementation is critical. There are different types of cement and the criteria for selection should be based on ease of manipulation; esthetics; resistance to compression and flexion; obtaining adequate marginal closure; and high bond strength that prevents the dislocation of the restoration and marginal microleakage.14,18,26-28 There are cements that may or may not be used with adhesive systems, facilitating the practicality of clinical use by reducing treatment steps to the dentin surface for the cementation. Thus, self-adhesive resin cement (RelyX U100) was evaluated in this study because it eliminates the steps of acidic conditioning and primer/adhesive application on the substrate.13 Its bonds to the dentin substrate through a mechanism of micromechanic retention and chemical interaction between the acidic monomer groups (phosphoric acid methacrylate ester) contained in the cement and the hydroxyapatite of the substrate. Immediately after its manipulation, it has relatively low pH (about 2), which superficially removes the smear layer without opening the dentin tubules and without forming a hybrid layer. Its setting is based on the polymerization reaction of free radicals initiated by photoactivation or self-polymerization. 29,30 However, studies have shown that this cement, or its previous version (RelyX Unicem), have lower bonding capacity due to the weak interaction with the substrate and low capacity for de-mineralization, leading to adhesive failure.13,17,31 Conditioning the enamel substrate with phosphoric acid has also been suggested in order to increase bond strength. Although this study has shown that self-adhesive cement (RelyX Unicem) did not differ in terms of bond strength from the conventional dual resin cement (Variolink II) evaluated, there was high prevalence of specimens prematurely lost when using the self-adhesive cement, as well as a lower number of viable sticks for the microtensile tests (Table 2). Premature failures were excluded from the statistical calculations, as their inclusion would have affected the normality of data distribution, thus precluding the use of parametric tests for assessing the influence of each study variable and of their interactions on the measured bond strengths.32 Goracci et al.32 did not consider the sticks prematurely fractured from a self-etching adhesive resin cement in their study and showed that this cement had the least reliable bonding potential. It could be suggested that as there was no difference with the conventional dual resin cement (Variolink II), taking into account that the lost specimens and sticks were not considered in the statistical analysis, the viable sticks for the study with self-adhesive cement (RelyX U100) presented adequate bond strength.
Hooshmand et al.33 found that dual-polymerized resin cements had better bonding efficacy to the lithium disilicate glass ceramic than the self-adhesive resin cement. In a clinical study, self-adhesive resin cement (RelyX Unicem) showed clinical outcomes similar to a conventional multi-step cementation procedure after 2 years of clinical service of inlay and onlay restorations with margins in enamel for most of the USPHS criteria evaluated.34 Therefore, future clinical research should also provide more answers about the performance of these resin cements, thus better explaining the in vitro studies.
The conventional self-polymerizing resin cement (Multilink) showed less bond strength than the other cements, corroborating the results of other studies.18,26 This may occur because of the activation of the monomers in a dual mode for the other cements evaluated, taking into account that photoactivation was carried out for the self-adhesive cement and for the conventional dual resin cement, providing greater polymer conversion than if the cement were only chemically activated.27,35 According to a study by Kumbuloglu et al.,14 the degree of conversion of resin cement is directly enhanced by photoactivation, which together with the redox system (tertiary amine reaction/Benzoyl peroxide) in its chemical setting reaction, complements the final polymerization. In self-polymerizing cements, this can take up to 24 hours, increasing the curing time, potentially decreasing the bond strength, and presenting lower surface hardness.35 On the other hand, due to greater monomer conversion, conventional dual resin cement (Variolink II) attains greater strength, hardness modulus, and flexion when also photoactivated during cementation.18,28
The conventional dual resin cement system (Variolink II) had the best bond strength of all the cements in this study, in agreement with the results of other studies. 18,19,25,29 Its utilization technique calls for the application of acidic conditioning on the dentin substrate, followed by the application of a hydrophilic adhesive system for the formation of a hybrid layer to make the adhesive bond effective.36 In this cementation system, the manufacturer recommends the use of a conventional two-step dual adhesive system (Excite DSC), indicating this type of activation of the setting reaction in locations where the polymerization may be compromised because of the width of the restorative material, with photoactivation being unnecessary since the setting action of the adhesive will occur together with that of the resin cement.25,36 The kind of fracture in this type of resin cement was predominantly mixed, and could be related to the adequate bond strength between the dentin substrate and the ceramics used in the study. However, there was a considerable number of cohesive fractures in the dentin with the use of leucite-based ceramics (17.9%) and lithium disilicate-based ceramics (22.9%), which may be explained by the type of adhesive system employed. In addition, the fact should be considered that the cement was a dual type, where the photoactivation of the cement allowed for greater polymer conversion, influencing the bond strength, as observed in other studies.27,28,35 In Groups EMM and EMV, there was a cohesive fracture in the ceramic, which could be related to tension when the ceramic was being cut or to a problem in the structure of the ceramic.
ACKNOWLEDGMENTS
The authors would like to thank LME/LNNano/CNPEM for the technical support during the electron microscopy work, Sofhia Carla Coelho for the technical support with the manufacturing of the ceramic blocks, and Ivoclar Vivadent for the materials used in this study.
1. Heintze SD, Cavalleri A, Zellweger G, Buchler A, Zappini G. Fracture frequency of all-ceramic during dynamic loading in a chewing simulator using different loading and luting protocols. Dent Mater 2008;24:1352-1361. [ Links ]
2. Radovic I, Monticelli F, Goracci C, Vulicevic ZR, Ferrari M. Self-adhesive resin cements: a literature review. J Adhes Dent 2008;10:251-258. [ Links ]
3. Ayad MF, Fahmy NZ, Rosenstiel SF. Effect of surface treatment on roughness and bond strength of a heat-pressed ceramic. J Prosthet Dent 2008;99:123-130. [ Links ]
4. Della Bona A, Anusavice KJ, Shen C. Microtensile strength of composite bonded to hot-pressed ceramics. J Adhesive Dent 2000;2:305-313. [ Links ]
5. Della Bona A, Anusavice KJ, Mecholsky Junior JJ. Apparent interfacial fracture toughness of resin/ ceramic systems. J Dent Res 2006;85:1037-1041. [ Links ]
6. Bitter K, Paris S, Hartwing C, Neumann K, Kielbassa AM. Shear bond strengths of different substrates bonded to lithium disilicate ceramics. Dent Mater J 2006;25:493-502. [ Links ]
7. Buhler-Zemp P. IPS Empress Esthetic scientific documentation [catalog]. Santa Maria, CA: Ivoclar Vivadent AG; 2004.p.3-5. [ Links ]
8. Heintze SD, Albrecht T, Cavalleri A, Steiner M. A new method to test the fracture probability of all-ceramic crowns with a dual-axis chewing simulator. Dent Mater 2011;27:e10-e19. [ Links ]
9. Wolfart S, Eschbach S, Scherrer S, Kern M. Clinical outcome of three-unit lithium-disilicate glass-ceramic fixed dental prostheses: up to 8 years results. Dent Mater 2009; 25:e63-e71. [ Links ]
10. Dietschi D, Spreafico R. Current clinical concepts for adhesive cementation of tooth-colored posterior restorations. Pract Periodontics Aesthet Dent 1998;10:47-55. [ Links ]
11. Burke FJT, Wilson NHF, Watts DC. Fracture resistance of teeth restored with indirect composite resins: the effect of alternative luting procedures. Quintessence Int 1994;25: 269-275. [ Links ]
12. Pegoraro TA, Silva NR, Carvalho RM. Cements for use in esthetic dentistry. Dent Clin North Am 2007;51:453-471. [ Links ]
13. Abo-Hamar SE, Hiller KA, Jung H, Federlin M, Friedl KH, Schmalz G. Bond strength of a new universal self-adhesive resin luting cement to dentin and enamel. Clin Oral Investig 2005;9:161-167. [ Links ]
14. Kumbuloglu O, Lassila LVJ, User A, Vallittu PK. A study of the physical and chemical properties of four resin composite luting cements. Int J Prosthod 2004;17:357-363. [ Links ]
15. Al-Assaf K, Chakmakchi M, Palaghias G, Karanika-Kouma A, Eliades G. Interfacial characteristics of adhesive luting resins and composites with dentin. Dent Mater 2007;23: 829-839. [ Links ]
16. De Munck J, Vargas M, van Landuyt K, Hikita K, Lambrechts P, van Meerbeek B. Bonding of an auto-adhesive luting material to enamel and dentin. Dent Mater 2004;20:963-971. [ Links ]
17. Viotti RG, Kasaz A, Pena CE, Alexandre RS, Arrais CE, Reis AF. Microtensile bond strength of new self-adhesive luting agents and conventional multistep systems. J Prosthet Dent 2009;102:306-312. [ Links ]
18. Hofmann N, Papsthart G, Hugo B, Klaiber B. Comparison of photo-activation versus chemical or dual-curing of resinbased luting cements regarding flexural strength, modulus and surface hardness. J Oral Rehabil 2001;28:1022-1028. [ Links ]
19. Ibarra G, Johnson GH, Geurtsen W, Vargas MA. Microleakage of porcelain veneer restorations bonded to enamel and dentin with a new self-adhesive resin-based dental cement. Dent Mater 2007;23:218-225. [ Links ]
20. Pisani-Proenca J, Erhardt MCG, Valandro LF, Gutierrez- Aceves G, Bolanos-Carmona MV, Castillo-Salmeron RD, Bottino MA. Influence of ceramic surface conditioning and resin cements on microtensile bond strength to a glass ceramic. J Prosthet Dent 2006;96:412-417. [ Links ]
21. Fabianelli A, Pollington S, Papacchini F, Goracci C, Cantoro A, Ferrari M, van Noort R. The effect of different surface treatments on bond strength between leucite reinforced feldspathic ceramic and composite resin. J Dent 2010;38:39-43. [ Links ]
22. Pollington S, Fabianelli A, van Noort R. Microtensile Bond strength of a resin cement to a novel fluorcanasite glassceramic following different surface treatments. Dent Mater 2010;26:864-872. [ Links ]
23. Passos SP, Valandro LF, Amaral R, Ozcan M, Bottino MA, Kimpara ET. Does adhesive resin application contribute to resin Bond durability on etched and silanized feldspathic ceramic? J Adhes Dent 2008;10:455-460. [ Links ]
24. Clelland NL, Ramirez A, Katsube N, Seghi RR. Influence of bond quality on failure load of leucite-and lithia disilicate- based ceramics. J Prosthet Dent 2007;97:18-24. [ Links ]
25. Toman M, Toksavul S, Akin A. Bond strength of all-ceramics to tooth structure using new luting systems. J Adhes Dent 2008;10:373-378. [ Links ]
26. Arrais CAG, Giannini M, Rueggeberg FA, Pashley DH. Microtensile bond strength of dual-polymerizing cementing systems to dentin using different polymerizing modes. J Prosthet Dent 2007;97:99-106. [ Links ]
27. Lee IB, An W, Chang J, Um CM. Influence of ceramic thickness and curing mode on the polymerization shrinkage kinetics of dual-cured resin cements. Dent Mater 2008;24:1141-1147. [ Links ]
28. Pereira SG, Fulgencio R, Nunes TG, Toledano OR, Carvalho RM. Effect of curing protocol on the polymerization of dual-cured resin cements. Dent Mater 2010;26:710-718. [ Links ]
29. Duarte S Jr, Botta AC, Meire M, Sadan A. Microtensile bond strengths and scanning electron microscopic evaluation of self-adhesive and self-etch resin cements to intact and etched enamel. J Prosthet Dent 2008;100:203-210. [ Links ]
30. Escribano N, Macorra JC. Microtensile Bond strength of self-adhesive luting cements to ceramic. J Adhes Dent 2006;8:337-341. [ Links ]
31. Yang B, Ludwig K, Adelung R, Kern M. Micro-tensile bond strength of three luting resins to human regional dentin. Dent Mater 2006;22:45-56. [ Links ]
32. Goracci C, Cury AH, Cantoro A, Papacchini F, Tay FR, Ferrari M. Microtensile bond strength and interfacial properties of self-etching and self-adhesive resin cements used to lute composite onlays under different seating forces. J Adhes Dent 2006;8:327-335. [ Links ]
33. Hooshmand T, Rostami G, Behroozibakhsh M, Fatemi M, Keshvad A, van Noort R. Interfacial fracture toughness of different resin cements bonded to a lithium disilicate glass ceramic. J Dent 2012;40:139-145. [ Links ]
34. Taschner M, Kramer N, Lohbauer U, Pelka M, Breschi L, Petschelt A, Frankenberger R. Leucite-reinforced glass ceramic inlays luted with self-adhesive resin cement: A 2- year in vivo study. J Adhes Dent 2012;28:535-540. [ Links ]
35. Vrochari AD, Eliades G, Hellwig E, Wrbas KT. Curing efficiency of four self-etching, self-adhesive resin cements.Dent Mater 2009;25:1104-1108. [ Links ]
36. Raffaelli O, Cagidiaco MC, Goracci C, Ferrari M. XP Bond in self-curing mode used for luting porcelain restorations. Part A: microtensile test. J Adhes Dent 2007;9: 275-278. [ Links ]














