Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Odontológica Latinoamericana
versão On-line ISSN 1852-4834
Acta odontol. latinoam. vol.27 no.1 Buenos Aires maio 2014
ARTÍCULOS ORIGINALES
Assessment of the association between overweight/obesity and traumatic dental injury among Brazilian schoolchildren
Veruska M. Martins, Raulison V. Sousa, Eveline S. Rocha, Rafaella B. Leite, Monalisa C. Gomes, Ana F. Granville-Garcia
Dentistry Department, State University of Paraíba, Campina Grande, Paraiba State, Brazil.
CORRESPONDENCE Dr.Ana Flavia Granville-Garcia Rua Cap. Joao Alves Lira 1325/410, Bela Vista, Campina Grande, PB, Brazil CEP: 58101281/ E-mail: anaflaviagg@hotmail.com
ABSTRACT
The aim of this study was to evaluate the association between overweight/obesity and the occurrence of traumatic dental injury among schoolchildren aged 7 to 14 years. A cross-sectional study was carried out involving 590 students at public schools in the city of Campina Grande, Brazil. The classification proposed by O'Brien (1994) was used for the diagnosis of traumatic dental injury. Overweight/obesity was determined based on the body mass index. Clinical examinations were performed by two examiners who had undergone a calibration exercise (Kappa statistics of 0.87 and 0.90 for intra-examiner and inter-examiner, respectively). Data analysis involved the chi-square test and Fisher's exact test with a 5% level of significance. Traumatic dental injury was less prevalent among the schoolchildren with overweight/obesity than those without this condition (8.7% and 13.3%, respectively). When the sample was stratified by gender and age, traumatic dental injury was also more prevalent among schoolchildren without overweight/obesity. When the sample was stratified based on ethnicity, prevalence rates were similar between those with and without overweight/obesity. In the overall sample, no significant association was found between overweight/obesity and traumatic dental injury (p = 0.253). Overweight/obesity among schoolchildren aged 7 to 14 years was not associated with traumatic dental injury in this study. The analysis of physical activity may be important to gain a better understanding of this finding.
Keywords: Tooth Injuries; Dentition; Permanent; Obesity.
RESUMO
Associação entre sobrepeso/obesidade e trauma dentário em escolares Brasileiros
O objetivo do presente estudo foi avaliar a associacao entre o sobrepeso/obesidade e a ocorrencia do trauma dentario entre escolares de 7 a 14 anos de idade. Caracterizou-se como um estudo transversal realizado com 590 escolares de escolas publicas de Campina Grande, Brasil. Utilizou-se como criterio de diagnostico para traumatismo dentario a classificacao proposta por O'Brien (1994) e para sobrepeso/obesidade o indice IMC. Os exames clinicos foram feitos por dois examinadores previamente calibrados (Kappa intra e inter de 0,87 e 0,90, respectivamente). Os testes estatisticos utilizados foram Qui-quadrado e exato de Fisher (significancia de 5%). Os individuos sem sobrepeso/obesidade apresentaram mais lesoes de trauma dentario que aqueles com sobrepeso/obesidade (13,3% vs 8,7%). Quando estratificada a amostra em relacao ao sexo, idade e grupo etnico, o traumatismo dentario foi mais prevalente entre criancas/adolescentes sem sobrepeso/obesidade, com excecao do grupo etnico, que apresentaram prevalencias similares. No grupo total nao foi observada associacao entre sobrepeso/obesidade e trauma dentario (p=0,253). A presenca de sobrepeso/obesidade em escolares de 7 a 14 anos nao foi associada ao traumatismo dentario. A analise da atividade fisica pode ser um fator importante para melhor elucidar a tematica.
Palavras-chaves: Traumatismos Dentarios; Denticao Permanente; Obesidade.
INTRODUCTION
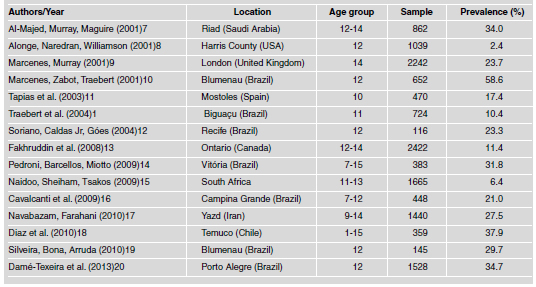
Traumatic dental injury is considered a public health problem1,2 and one of the main reasons for urgent dental care. It can also have a negative impact on quality of life3-6. The literature reports high prevalence rates of traumatic dental injury among schoolchildren (Table 1, with references.1,7-20). Studies indicate that accentuated overjet, inadequate lip seal and overweight/obesity are predisposing factors to this condition. However, divergent results are found regarding the association with overweight/obesity20- 24 and no in-depth analysis has yet been carried out on this subject.
Table 1: Prevalence studies on traumatic dental injury in the literature.
The prevalence of childhood obesity has been on the rise in both Brazil and around the world in recent decades, with rates ranging from 11.4% to 28.7%21,25-29. This increased prevalence has motivated a number of studies in the field of dentistry.
The aim of this study was to investigate a possible association between overweight/obesity and the occurrence of traumatic dental injury among schoolchildren aged 7 to 14 years.
METHODS
Sample characteristics
A cross-sectional study was carried out involving male and female school children aged 7 to 14 years at public schools in the city of Campina Grande, Brazil. The participants were selected from a population of 15,946 schoolchildren in the same age group. Two-stage sampling was performed to ensure representativeness: schools were first randomly selected from each administrative district of the city and schoolchildren were then randomly selected from each school. The sample size was calculated based on a 21.0% prevalence rate of traumatic dental injury, a 5% margin of error and a 95% confidence interval. A correction factor of 2.0 was applied to compensate for the design effect, leading to a minimum sample of 502 schoolchildren, to which 20% was added to compensate for possible losses. Thus, the sample size was determined to be 602 schoolchildren.
Eligibility criteria
Inclusion criteria were agreement to undergo the clinical examination and a statement of informed consent signed by a parent or guardian. Exclusion criteria were deviations from normality, missing teeth due to dental caries, extensive carious lesions on the upper central incisors and the use of an orthodontic appliance.
Pilot study
A pilot study was conducted to test the methodology. The children in the pilot study (n = 41) were not included in the main sample. The results revealed no misunderstandings regarding the questionnaire or need for changes to the method.
Training and calibration exercise
The theoretical phase involved a discussion of the diagnostic criteria for traumatic dental injury and an analysis of photographs. A specialist in this field served as the gold standard in the theoretical reference and instructed two researchers on how to perform the examination. The clinical phase was carried out at a randomly selected school that was not part of the main sample. Each researcher examined 50 schoolchildren for the determination of inter-examiner agreement. Thirty schoolchildren were examined a second time after a seven-day period for the determination of intraexaminer agreement. Kappa coefficients were 0.87 and 0.90 for intra-examiner and inter-examiner agreement, respectively, demonstrating that the examiners were capable of conducting the epidemiological study.
Data acquisition
Examinations were performed at school during normal classroom hours by the two examiners who had undergone the training and calibration exercise. The criteria proposed in the Children's Dental Health Survey of the United Kingdom30 were used for the diagnosis of traumatic dental injury. Both natural and artificial (classroom lighting) light was used during the examinations. The teeth were first cleaned and dried with gauze. A No 5 mouth mirror (PRISMAR, Sao Paulo, SP, Brazil) was used for the examination. The examiners used individual protection equipment against cross-infection and all materials had been sterilized. Body mass index (BMI) was calculated by weight in kilograms divided by the square of height in meters (Kg/m2). The determination of overweight/ obesity was based on the criteria established by the World Health Organization (2007) for child and adolescent growth and calculated using the AnthroPlus program31. Individuals with a BMI equal to or greater than the 85th percentile were classified with overweight/obesity. Individuals with a BMI greater than the 15th percentile and less than the 85th percentile were classified without overweight/obesity.
Statistical analysis
Data were analyzed using the Statistical Package for the Social Sciences (SPSS for Windows, version 18.0, SPSS Inc, Chicago, IL, USA). The chisquare test and Fisher's exact test were employed to test the association between overweight/obesity and traumatic dental injury. The level of significance was set at 5% (p < 0.05).
Ethical considerations
This study received approval from the State University of Paraiba (Brazil) under process number 05700133000-08 and was carried out in compliance with Resolution 196/96 of the Brazilian National Board of Health and the 1975 Declaration of Helsinki.
RESULTS
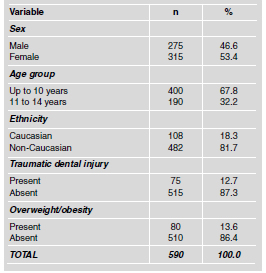
This study involved 602 schoolchildren, seven of whom refused to participate and five of whom were excluded due to extensive caries on the anterior teeth (1.9% of the total sample). Among the 590 schoolchildren examined, 275 (46.6%) were male and 315 (53.4%) were female. The majority of participants were up to ten years of age (67.8%) and non-Caucasian (81.7%). The prevalence of traumatic dental injury in the permanent anterior teeth was 12.7% (n = 74) and the prevalence of overweight/obesity was 13.6% (Table 2).
Table 2: Characterization of the sample.
Traumatic dental injury was less prevalent among the individuals with overweight/obesity than among those without this condition (8.7% vs. 13.3%). No significant association was found between overweight/obesity and traumatic dental injury (p = 0.253) (Table 3). When the sample was stratified based on gender among individuals with overweight/obesity, the prevalence of traumatic dental injury was greater among males than females (13.5% and 4.7%, respectively). However, the statistical tests revealed no association between traumatic dental injury and either gender or overweight/obesity in the sample studied (Table 3).
Table 3: Occurrence of traumatic dental injury according to weight classification and stratified by gender, age and ethnicity.
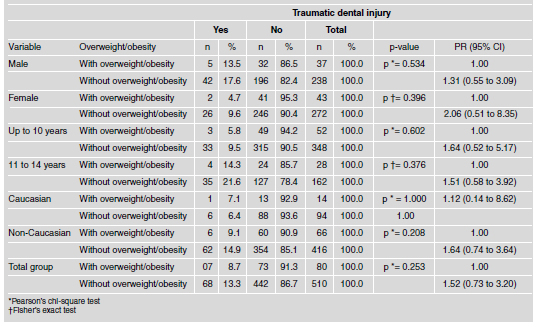
While traumatic dental injury among individuals with overweight/obesity was more prevalent in the 11-to-14-year-old age group than in those up to 10 years of age (14.3% and 5.8%, respectively), age was not significantly associated with traumatic dental injury in the sample. Moreover, no statistically significant difference was found between children with and without overweight/obesity when the sample was stratified based on ethnicity (Table 3).
DISCUSSION
Traumatic dental injury and childhood obesity have piqued the interest of the scientific community in recent years, as both conditions affect a significant portion of the population, have an impact on quality of life and involve high healthcare costs4,6,32,33. In this study, the prevalence of traumatic dental injury was 12.7% among schoolchildren aged 7 to 14 years. This is in agreement with findings described in both Brazilian1,6,34,35 and international5,11,36 studies, which report rates ranging from 10 to 18%. However, other studies report rates as high as 34.7%20 and even 66.6%18. The divergence may be explained by cultural differences as well as differences in the diagnostic criteria, type of sample and age group analyzed34,37.
The prevalence of overweight/obesity was 13.6%, which is similar to figures reported in studies carried out in Brazil (13.3 to 15.7%)25-27. Although this rate is lower than the national average (36.4%)38, it is sixfold higher than the target rate of 2.3% established by the World Health Organization39. Studies report a number of factors associated with the increase in the prevalence of overweight/obesity, such as changes in child behavior in recent decades, especially with regard to dietary habits and a reduction in physical activity27,32.
Excess weight can lead to alterations in the joints of the feet and their relationship to the ankle, which can affect postural control strategies and the alignment of other joints of the lower limbs and trunk. Over time, excessive shortening or lengthening may occur, which, along with the forward lean of the pelvis, lead to internal rotation of the hip and the emergence of valgus knees and fallen arches28,40. Due to these mechanisms of postural adaptation, reports of falls (29.41%) and imbalance (67.64%) are frequent among obese schoolchildren aged 6 to 12 years28.
Analyses addressing the influence of obesity on the occurrence of traumatic dental injury remain scarce and the findings are conflicting. A study carried out in 2006 assessed this association in preschoolers and found that children with overweight/obesity had a 2.5-fold greater chance of having traumatic dental injury than children within the ideal weight range41. Similar findings are reported in an investigation carried out in Italy with schoolchildren aged 6 to 11 years21 and a study conducted in Brazil involving 13-year-olds22. According to the authors cited, obesity in children is a risk factor for traumatic dental injury because obese children are less agile than those who are within the ideal weight range, which may make them more prone to accidents21,22. However, overweight/ obesity did not prove to be a risk factor for the occurrence of traumatic dental injury among the schoolchildren analyzed in our study (p = 0.253), which is in agreement with findings described in other Brazilian studies as well as other papers published in the international literature11,20,23,34,37,42.
When the sample is stratfied by gender, age and ethnic background, traumatic dental injury was more prevalent among the schoolchildren without overweight/ obesity, except those of Caucasian ethnicity, among whom prevalence rates were similar (7.1% vs. 6.4%). Previous studies have also found no association between gender and the occurrence of traumatic dental injury among individuals with overweight/obesity34,37. With regard to age and ethnic background, a search of the literature revealed no study that stratified the sample based on these variables in the analysis of an association between traumatic dental injury and overweight/obesity. In our study, however, the occurrence of traumatic dental injury proved to be independent of overweight/ obesity in the stratified analysis.
The divergent results in the literature on this subject suggest that other factors, such as physical activity, merit further investigation. Falls stemming from physical activities are considered a predisposing factor for the occurrence of traumatic dental injury. As children/adolescents with overweight/ obesity lead a sedentary lifestyle43,44, they are consequently less prone to accidents of this nature in comparison to children/adolescents within the ideal weight range11,18,36,45,46. Case-control studies and longitudinal investigations are needed to assess the influence of different degrees of physical activity on the occurrence of traumatic dental injury.
It is important to highlight the methodological differences among studies regarding the diagnosis of overweight/ obesity. In this study, schoolchildren with a BMI equal to or greater than the 85th percentile were classified as overweight/obese, which is similar to the criterion used in a previous study11. However, other studies either used different cutoff points21,23 or failed to report the cutoff point employed20,22,42. Some studies applied a different classification system, such as that proposed by the National Center for Health Statistics34,37. The different cutoff points may contribute to the contradictory findings reported in studies of this nature and underscore the need to analyze the data with caution. Moreover, all studies addressing this issue have had a cross-sectional design, which does not allow the determination of cause and effect. As a change in nutritional status from ideal weight to excess weight or vice versa is faster among schoolchildren than in other phases of life, prevalence bias is a factor to consider in these studies.
1. Traebert, J, Almeida ICS, Garghetti C, Marcenes W. Prevalence, treatment needs, and predisposing factors for traumatic injuries to permanent dentition in 11-13-year-old schoolchildren. Cad Saude Publica 2004;20:403-410. [ Links ]
2. Glendor U. Aetiology and risk factors related to traumatic dental injuries - a review of the literature. Dent Traumatol 2009;25:19-31. [ Links ]
3. Cortes MI, Marcenes W, Sheiham A. Impact of traumatic injuries to the permanent teeth on the oral health-related quality of life in 12-14-yearold children. Community Dent Oral Epidemiol 2002;30:193-198. [ Links ]
4. Glendor U. Epidemiology of traumatic dental injuries-a 12 year review of the literature. Dent Traumatol 2008;24:603-611. [ Links ]
5. Fakhruddin KS, Lawrence HP, Kenny DJ, Locker D. Impact of treated and untreated dental injuries on the quality of life of Ontario school children. Dent Traumatol 2008;24:309-313. [ Links ]
6. Francisco SS, Souza Filho FJ, Pinheiro ET, Murrer RD, Soares, AJ. Prevalence of traumatic dental injuries and associated factors among brazilian schoolchildren. Oral Health Prev Dent 2013; 11:31-38. [ Links ]
7. Al-Majed J, Murray JJ, Manguire A. Prevalence of dental trauma in 5-6- and 12-14-year-old boys in Riyadh, Saudi Arabia. Dent Traumatol 2001;17:153-158. [ Links ]
8. Alonge K, Narendran S, Williamson DD. Prevalence of fractured incisal teeth among children in Harris County, Texas. Dent Traumatol 2001; 15:218-221. [ Links ]
9. Marcenes W, Murray S. Social deprivation and traumatic dental injuries among 14-year-old schoolchildren in Newham, London. Dent Traumatol 2001;17:17-21. [ Links ]
10. Marcenes W, Zabot NE, Traebert J. Socio-economic correlates of traumatic injuries to the permanent incisors in schoolchildren aged 12 years in Blumenau, Brazil. Dent Traumatol 2001;17: 22-26. [ Links ]
11. Tapias MA, Jimenez-Garcia R, Lamas F, Gil AA. Prevalence of traumatic crown fractures to permanent incisors in a childhood population: Mostoles, Spain. Dent Traumatol 2003;19:119-122. [ Links ]
12. Soriano EP, Caldas jr AF, Goes PSA. Risk factors related to traumatic dental injuries in Brazilian schoolchildren. Dent Traumatol 2004; 20:246-250. [ Links ]
13. Fakhruddin KS, Lawrence HP, Kenny DJ, Locker D. Etiology and environment of dental injuries in 12- to 14-year-old Ontario schoolchildren. Dent Traumatol 2008;24:305-308. [ Links ]
14. Pedroni IBG, Barcellos IA, Miotto MHMB. Treatment of traumatized permanent teeth. Pesq Bras Odontoped Clin Integr 2009;9:107-112. [ Links ]
15. Naidoo S, Sheiham A., Tsakos G. Traumatic dental injuries of permanent incisors in 11- to 13-year-old South African schoolchildren. Dent Traumatol 2009;25:224-228. [ Links ]
16. Cavalcanti AL, Bezerra PKM, Alencar CRB, Moura C. Traumatic anterior dental injuries in 7- to 12-year-old Brazilian children. Dent Traumatol 2009;25:198-202. [ Links ]
17. Navabazam A, Farahani SS. Prevalence of traumatic injuries to maxillary permanent teeth in 9- to 14 -year-old school children in Yazd, Iran. Dent Traumatol 2010;26:154-157. [ Links ]
18. Diaz JA, Bustos l, Brandt AC, Fernandez BE. Dental injuries among children and adolescents aged 1-15 years attending to public hospital intemuco, Chile. Dent Traumatol 2010; 26:254-261. [ Links ]
19. Silveira JLGC, Bona AJ, Arruda JAB. Dental trauma in 12-year-old schoolchildren from the city of Blumenau, SC, Brazil. Pesq Bras Odontoped Clin Integr 2010; 10:23-26. [ Links ]
20. Dame-Teixeira N, Alves LS, Susin C, Maltz M. Traumatic dental injury among 12-year-old south brazilian schoolchildren: prevalence, severity, and risk indicators. Dent Traumatol 2013; 29: 52-58. [ Links ]
21. Petti S, Cairella G, Tarsitani G. Childhood obesity: a risk factor for traumatic injuries to anterior teeth. Endod Dent Traumatol 1997; 13:285-288. [ Links ]
22. Nicolau B, Marcenes W, Sheiham A. Prevalence, causes and correlates of traumatic dental injuries among 13-yearsold in Brazil. Dent Traumatol 2001; 17:213-217. [ Links ]
23. Artun J, Al-Azemi R. Social and behavioral risk factors for maxillary incisor trauma in an adolescent Arab population. Dent Traumatol 2009; 25:589-593. [ Links ]
24. Schatz JP, Hakeber M, Ostini E, Kiliaridis S. Prevalence of traumatic injuries to permanent dentition and its association with overjet in a Swiss child population. Dent Traumatol 2013; 29:110-114. [ Links ]
25. Leao LSCS, Araujo LMAB, Moraes LTLP, Assis AM. Prevalence of obesity in school children from Salvador, Bahia. Arq Bras Endocrinol Metab 2003;47:151-157. [ Links ]
26. Ricardo GD, Caldeira GV, Corso ACT. Prevalence of overweight and obesity and adiposity central indexes among school-aged children in Santa Catarina, Brazil. Rev Bras Epidemiol 2009;12:1-12. [ Links ]
27. Leal VS, Lira PIC, Oliveira JS, Menezes RCE, Sequeira LAS, Arruda Neto, MA, Andrade SLLS, Batista Filho M. Overweight in children and adolescents in Pernambuco state, Brazil: prevalence and determinants. Cad Saude Publica 2012;28:1175-1182. [ Links ]
28. Aleixo AA, Guimaraes EL, Walsh IAP, Pereira K. Influence of overweight and obesity on posture, overall praxis and balance in schoolchildren. Journal of Human Growth and Development 2012;22:239-245. [ Links ]
29. Pedroni JL, Rech RR, Halpern R, Marin S, Roth LR, Sirtoli M, Cavalli A. Prevalence of abdominal obesity and excess fat in students of a city in the mountains of southern Brazil. Cien Saude Colet 2013; 18:1417-1425. [ Links ]
30. O'Brien M. Children's dental health in the United Kingdom 1993. Office of population censuses and surveys. London: HMSO; 1994. [ Links ]
31. WHO AnthroPlus for personal computers manual: Software for assessing growth of the world's children and adolescents. Geneva: WHO, 2009. [cited 2013 May 20]. Available from: http://www.who.int/growthref/tools/en/. [ Links ]
32. Enes CC, Slater B. Obesity in adolescence and its main determinants. Rev Bras Epidemiol 2010;13:163-171. [ Links ]
33. Ferreira JS, Aydos RD. Prevalence of hypertension among obese children and adolescents. Cien Saude Colet 2010;15:97-104. [ Links ]
34. Soriano EP, Caldas Jr AF, Carvalho MVD, Caldas KU. Relationship between traumatic dental injuries and obesity in brazilian schoolchildren. Dental Traumatol 2009;25:506-509. [ Links ]
35. Piovesan C, Abella C, Ardenghi TM. Child oral health-related quality of Life and socioeconomic factors associated with traumatic dental injuries in schoolchildren. Oral Health Prev Dent 2011; 9:405-411. [ Links ]
36. Ankola AV, Hebbal M, Sharma R, Nayak SS. Traumatic dental injuries in primary school children of South India - a report from districtwide oral health survey. Dent Traumatol 2013; 29:134-138. [ Links ]
37. Soriano EP, Caldas Jr AF, Carvalho, MVD, Amorim HAT. Prevalence and risk factors related to traumatic dental injuries in brazilian schoolchildren. Dent Traumatol 2007;23:232-240. [ Links ]
38. Instituto Brasileiro de Geografia e Estatistica. Pesquisa de orcamentos familiares: antropometria e estado nutricional de criancas, adolescentes e adultos do Brasil. Rio de Janeiro: Instituto Brasileiro de Geografia e Estatistica; 2010. [ Links ]
39. Centro Brasileiro de Analise e Planejamento, Ministerio da Saude. Pesquisa nacional de demografia e saude da crianca e da mulher - PNDS 2006: dimensoes do processo reprodutivo e da saude da crianca. Brasilia: Ministerio da Saude; 2009. [ Links ]
40. Martinelli AR, Purga MO, Mantovani AM, Camargo MR, Rosell AA, Fregonesi CEPT, Freitas Junior IF. Analysis of lower limb alignment in overweight children. Rev Bras Cineantropom Desempenho Hum 2011; 13:124-130. [ Links ]
41. Granville-Garcia AF, Menezes VA, Lira PIC. Dental trauma and associated factors in Brazilian preschoolers. Dent Traumatol 2006; 22:318- 322. [ Links ]
42. Nicolau B, Marcenes W, Sheiham A. The relationship between traumatic dental injuries and adolescents' development along the life course. Dent Traumatol 2003; 31:306-313. [ Links ]
43. Mitchell JA, Mattocks C, Ness AR, Leary SD, Pate RR, Dowda M, Blair SN, Riddoch C. Sedentary behavior and obesity in a large cohort of children. Obesity (Silver Spring) 2009; 17: 1596-1602. [ Links ]
44. Herman KM, Sabiston CM, Tremblay A, Paradis G. Self-rated health in children at risk for obesity: associations of physical activity, sedentary behaviour and BMI. J Phys Act Health 2013; 8. [Epub ahead of print] [ Links ]
45. Stewart GB, Shields BJ, Fields S, Comstock RD, Smith GA. Consumer products and activities associated with dental injuries to children treated in United States emergency departments, 1990-2003. Dent Traumatol 2009; 25: 399-405. [ Links ]
46. Govindarajan M, Reddy VN, Ramalingam K, Durai KS, Rao PA, Prabhu A. Prevalence of traumatic dental injuries to the anterior teeth among three to thirteen-year-old school children of Tamilnadu. Contemp Clin Dent 2012; 3:164-167. [ Links ]














