Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Odontológica Latinoamericana
versão On-line ISSN 1852-4834
Acta odontol. latinoam. vol.29 no.2 Buenos Aires set. 2016
ARTÍCULOS ORIGINALES
Effects of new implant-retained overdentures on masticatory function, satisfaction and quality of life
Francielle A. Mendes1, Tânia de F. Borges2, Luiz C. Gonçalves3, Terezinha R.C. de Oliveira2, Célio J. do Prado4, Flávio D. das Neves4
1 Department of Dental Materials, Ribeirão Preto School of Dentistry, University of São Paulo, Brazil.
2 Department of Prosthodontics, Technical School of Health, Federal University of Uberlândia, Brazil.
3 Department of Removable Prosthodontics and Dental Materials, School of Dentistry, Federal University of Uberlândia, Brazil.
4 Department of Occlusion, Fixed Prosthodontics, and Dental Materials, School of Dentistry, Federal University of Uberlândia, Brazil.
CORRESPONDENCE Dr. Francielle Alves Mendes Av. Para, no 1720, Bloco 4L Anexo A, Sala 4LA42. 38405320, Uberlandia, M, Brazil. Email: franciellemendes@usp.br
ABSTRACT
The aim of this study is to evaluate the effects of replacing poorly fitting dentures on patient’s masticatory function, satisfaction and oral healthrelated quality of life. Fourteen patients with conventional maxillary complete dentures and mandibular overdentures retained by two implants bar clip system had their dentures replaced. The laboratory tests for the analysis of masticatory performance were conducted using an “Optocal” food simulator test. Questionnaires were used to evaluate patient satisfaction with dentures and impact of oral health on quality of life. Tests were conducted and questionnaires were administered before and 1, 3 and 6 months after the patient had adapted to the new dentures. Masticatory performance data and satisfaction with dentures (Visual Analogic Scale) were statistically analyzed by ANOVA and Tukey b test, satisfaction with dentures (SATs P) and impact of oral health on quality of life were evaluated using the Wilcoxon and Friedman tests (a=.05). There was no statistically significant improvement in masticatory function after denture replacement, although better outcomes were observed. Satisfaction with dentures and total score obtained using the OHIPedent showed significant improvement. It can be suggested that the potential for grinding food, patient satisfaction and aspects of quality of life improved immediately after denture replacement.
Key words: Edentulous; Quality of life; Overdenture; Patient satisfaction; Mastication.
RESUMO
Efeito de novas overdentures implanto retidas na função mastigatória, satisfação e qualidade de vida
Avaliar os efeitos da substituição de próteses mal adaptadas na função mastigatória, satisfação e qualidade de vida relacionada à saúde bucal do paciente. Quatorze pacientes com próteses totais convencionais maxilarese overdentures retidas por dois implantes mandibularessistem abarra clip etiveram suas prótes essubstituídas .Os testes laboratoriais para análise da performance mastigatória foram realizados utilizando um simulador de alimento “Optocal”. Foram utili za dos questionários para avaliar a satisfação com a prótese eo impacto da saúde bucal na qualidade de vida. Os testes foram realizados e os questionários foram aplicados antes, 1, 3 e 6 mes esapós o paciente ter adaptado às novas próteses. Os dados da performance mastigatória e satisfação com a prótese (EscalaAnalógica Visual) foram analisados estatistica mente por análise de variância e teste de Tukey b, a satisfação com próteses (SATs P) e o impacto da saúde bucal na qualidade de vida foram avaliados pormeio dos testes de Wilcoxon e Friedman (a = 0,05). Não houvem elhora estatisticamente significativa na função mastigatória após a troca daspróteses, em boram elhores resultados foram observados após a substituição. Satisfação com a prótese e a somatória total obtida utilizando o OHIPEdent mostraram melhora signi ficativa. Podese sugerir que o potencial de trituração dos alimentos, a satisfação do paciente com as nova spróteses e aspectos da qualidade de vida melhorar amimediatamente após a substituição da prótese.
Palavras chave: Desdentado; Overdentures; Mastigação; Satisfação com as próteses.
INTRODUCTION
Despite the declining prevalence and low incidence of edentulism in countries where reliable epidemio logical data exist, from a global perspective, large numbers of edentulous individuals, particularly among the elderly, are in need of rehabilitation. Complete dentures are and will remain the mainstay of treatment for the vast majority of edentulous patients. Most patients report satisfaction with denture usage, however, a smaller number are unable to adapt1. As it is especially difficult to adjust to a lower denture, because the support and retention areas are compromised, overdentures are recommended.
However, over time, implantretained overdentures present some complications such as loss of attachment, retention, denture fracture, tooth wear, denture base misfit due to bone resorption, color change and tooth shape25. The fact that the overdenture support system is similar to that of complete dentures, both being mucosasupported, suggests that overdentures should be replaced in shorter or similar periods to conventional complete dentures. As with complete dentures, the decision to replace overdentures should follow criteria based on a combination of the examiners’ subjective opinion regarding the denture aspect and the patients’ satisfaction6. However, many patients with clinically unacceptable dentures present greater than expected prosthetic tolerance and level of satisfaction, suggesting that such acceptance depends on how each individual adapts7. Dentists should tell patients when to replace dentures and explain the benefits to masticatory function and quality of life.
Many studies have evaluated masticatory function, satisfaction with the new denture and quality of life in individuals who received new complete dentures6,8-14. However, there is no published retrospective study comparing the masticatory function, satisfaction and quality of life in indivi duals who have worn two mandibular implantsupported overdentures before and after replacing new dentures. Considering the increasing use of mandibular implantretained overdentures, it is relevant to investigate the null hypothesis of this study, which was “denture replacement may improve masticatory function, patient satisfaction and quality of life”.
MATERIALS AND METHODS
This study was approved by the Institutional Review Board of the Federal University of Uberlandia for the use of human subjects in research and has therefore been performed in accordance with the ethical standards set forth in the 1964 Declaration of Helsinki and its later amendments. Written informed consent was obtained from each subject after a full explanation of the research project. In this study, participants are part of a longitudinal followup of patients who had their complete mandibular dentures converted to implantretained overdentures15,16 The evaluation of denture quality was performed by a single calibrated examiner. Laboratory tests were performed to assess masti catory performance and questionnaires were administered to assess patient satisfaction with the dentures and oral healthrelated quality before and 1, 3 and 6 months after the patient’s adaptation to the new dentures.
Evaluation of Denture Quality
Dentures were evaluated to determine the need for replacement according to the following criteria: vertical dimension, aesthetics, occlusion, extension of dentures, time of use, retention, stability, and incidence of fracture of dentures and clips. Furthermore, a subjective assessment focused on satisfaction was taken into consideration. All prosthetic procedures and evaluations were performed by the same prosthodontists according to a technique recommended by the Dental School of the Federal University of Uberlandia.
Objective Analysis of Masticatory Performance
Masticatory performance was determined by chewing 17 cubes (approximately 3 cm3) of Optocal17, for 40 continuous sequential strokes. Chewed particles were immediately sieved through a stack of eight sieves (Bertel Industria Metalur gica), with square apertures between 5.6 mm and 0.5 mm. Based on the weight of particles obtained from each sieve, the geometric mean diameter (GMD) of the particles was calculated using the weighted geometric mean. The GMD was calculated using Excel spreadsheets (Microsoft Corp, One Microsoft Way, Redmond, WA, 98052, USA). If all of the masticated content was retained in the 0.56mm sieve, (6660μm is the maximum GMD value) the patient would have 6660μm, which is considered the initial particle size. Masticatory Performance was calculated as the initial particle size minus GMD converted to a percentage by crossmultiplication. This method has been fully described elsewhere15,17,18.
Analysis of satisfaction with the prostheses
Two questionnaires were used to evaluate patient satisfaction: (1) Satisfaction with current prostheses and (2) Visual Analogue Scale (VAS)16.
1. Satisfaction with current prostheses The questionnaire consisted of six questions related to satisfaction with the appearance, retention and comfort of the prostheses 16,19: (1) Are you comfortable smiling in proximity to other people; (2) Are you satisfied with your appearance?; (3) Are you able to laugh outright with other people (a) The maxillary prosthesis moves (b) The mandibular prosthesis moves; (4) Do you talk freely to other people (a) The maxillary prosthesis moves (b) The mandibular prosthesis moves; (5) Do you eat in proximity to other people; (6) Do you have pain or any discomfort in your mouth. Patient perception in relation to each question was recorded by the researcher in terms of Yes or No.
2. Visual Analogue Scale (VAS) To complement the questionnaire with regards to satisfaction with current prostheses, four questions were asked to evaluate patient’s perception with regard to maxillary, mandibular prostheses, stability/ retention and appearance, which were verified using the Visual Analogue Scale – VAS16,20-22. The VAS has a scale of 010, with the extremes corresponding to “completely dissatisfied” and “totally satisfied”, respectively.
Analysis of oral healthrelated quality of life (OHIPedent)
The quality of life analysis was carried out by administering the OHIPedent16,23, a validated specific questionnaire for edentulous patients, which detects changes in oral healthrelated quality before and after the placement of new dentures. It is a 19item questionnaire with the following answering options: A = never, B = sometimes and C = almost always, which are divided into 4 domains: (a) masticatoryrelated complaints, (b) psychological discomfort and disability, (c) social disability and (d) oral pain and discomfort. Three possible responses with their scores in parentheses were provided as options: never (0), sometimes (1) or almost always (2). The scores for the questionnaire were calculated for the four domains at baseline, and after 1, 3 and 6 months.
STATISTICAL ANALYSIS
Statistical analysis was performed using the Statistical Package for Social Sciences (SPSS), version 17.0 (SPSS Inc.; Chicago, IL, USA). Masticatory performance potential was analyzed by OneWay Anova and satisfaction with prostheses (VAS) by OneWay Anova and Tukey b to compare the values obtained at baseline and at 1, 3 and 6 months. For the data obtained on the nominal scale, a satisfaction questionnaire and OHIPedent, Wilcoxon’s and Friedman’s tests were applied. Statistical significance was set at 5%.
RESULTS
Evaluation of Denture Quality
Among the 16 patients whose prostheses had been converted a year and a half before, 14 (10 female and 4 male) , between ages 32 and 74 years (mean age 59.2 years) had an appointment to reevaluate their prosthesis, which showed that their dentures needed to be replaced: 100% of patients presented unsatisfactory occlusion with poorly distributed contacts; 7 (50%) showed decreased vertical dimension; 11 (78%) showed extension of unsatisfactory dentures; 9 (64%) had over five years of denture use; 5 (35%) showed an incidence of denture base fracture in the clip region; and six (42%) were dissatisfied with the aesthetic appearance of the denture.
Masticatory Performance
There was no statistically significant difference in masticatory performance after denture replacement (ANOVA), although higher values were observed mainly after 3 and 6 months (Table 1).
Table 1. Mean, standard deviation, confidence interval and level of significance using ANOVA test (p< 0.05) for masticatory performance with 40 strokes before and 1, 3 and 6 months after denture replacement.

Analysis of satisfaction with the prostheses
1. Satisfaction with current prostheses No significant difference was found between satisfaction with the new mandibular overdentures and the old mandibular overdentures. For the complete maxillary denture, there was improvement in denture movement when laughing (question 3a) and talking freely with others (question 4a) in the first month after denture replacement. Greater satisfaction was also observed in terms of pain/discomfort in the mouth (question 6) (Table 2).
Table 2. Level of significance (p) and statistical category (SC)** of questions 1, 2, 3a, 3b, 4a, 4b, 5 and 6 comparing each question for the 4 stages.

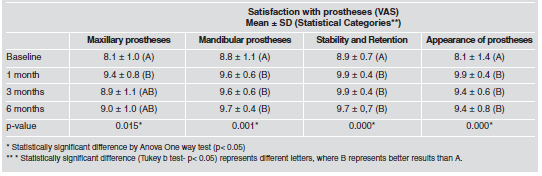
2. Visual Analogue Scale VAS There were statistically significant differences for all satisfaction aspects with the prostheses (VAS), showing improvement in both the complete maxillary dentures and the mandibular overdentures in the first evaluation after prosthesis replacement. Greater satisfaction with complete maxillary dentures was observed at the 1month evaluation after replacement. No statistically significant difference was found between baseline, 3 and 6 months only for this aspect (Table 3).
Table 3. Mean, standard deviation (SD) and statistical categories at baseline, 1, 3 and 6 months for the evaluation of satisfaction with prostheses using VAS.
Analysis of oral healthrelated quality of life (OHIPedent)
There was a statistically significant improvement in relation to four questions, namely, questions 2 on food retention, 3 on incorrect fitting, 6 on painful points in the mouth and 10 on avoiding eating due to painful points in the mouth. There were statistically significant differences for the four domains: masticatoryrelated complaints, psychological discomfort and disability and social disability. For oral pain and discomfort, no statistically significant difference was observed (Table 4).
Table 4. Statistical Category (SC)** and level of significance * (p) of questions, das s, subscales and questionnaire total score- OHIP-edent-19.

DISCUSSION
After denture replacement, there was no statisti cally significant improvement for the masticatory function, so the null hypothesis was rejected. For satisfaction with dentures and quality of life, the null hypothesis was partially rejected. The relevance of this study should be emphasized considering that no previous study has evaluated the effect of mandibular overdenture replacement on masticatory function, patient satisfaction and quality of life. The studies conducted on the subject referred to mandibular and maxillary conventional complete dentures. Andreiotelli et al. reported the following complica tions associated with implant overdentures: loss of retention or adjustment, clip or attachment fracture, overdenture fracture and acrylic resin base fracture. In this study, the main problems related to the prostheses were incidence of denture fracture (35%), loss of retention or loose clips (50%), unfavorable occlusion (100%), unsatisfactory prosthesis extension (78%), decreased vertical dimension (50%) and dissatisfaction with the aesthetic appearance (42%) 2.
The incidence of prosthesis fracture may have been due to the conversion of conventional overdenture to immediate prosthesis, which was not initially made for overdenture, causing fragility in the clip region and greater predisposition to fracture. In addition, the conversion time of prostheses of more than one year explains the problems with the clips: lack or loosening of retention. This was observed in the study by Bressan et al., in which few patients experienced loosening of retention (2.8%), but it was a crosssectional study and patients were recalled once a year for followup visits, and if necessary, activation of retentive clips3. The prostheses of all patients presented unsatis factory occlusion, mainly when there was contact with anterior teeth and poor distribution of posterior contacts upon closing. The maxillary prostheses of 9 patients presented unsatisfactory retention and stability, probably suggesting a relationship between unsatisfactory occlusion and prosthesis instability. After treatment, all patients presented bilateral balanced occlusion, which aims to stabilize dentures and minimize the resorption of alveolar bone and abrasion of denture teeth24.
After replacement, when asked about the buildup of food under the mandibular prosthesis (question 2 OHIPedent), patients reported that this no longer happened, and that they felt comfortable during mastication. Bressan et al. concluded that more than 50% of the subjects reported food impaction under the prosthesis and that this problem began about a year after treatment3. Complaints of food impaction may be related either to the time of denture use, as observed by Bressan, or to denture subextension, in which 78% of individuals had subextended mandibular prosthesis3. Other problems related to overdentures, such as decreased vertical dimension and dissatisfaction with the aesthetics, may be due to time of use (over 5 years), according to which they are in need of replacement.
The results of this study showed that although 64% of patients have improved masticatory performance (9 out of 14 patients), there was no statistically significant improvement after 1, 3 and 6 months, even though the prostheses were in satisfactory condition. In this study, patients were wearing complete dentures and after conversion to mandi bular overdenture, their masticatory function improved significantly15,16. However, the potential for grinding food did not improve immediately after replacing the unsatisfactory dentures, even though there was an improvement for all patients. This may a result of the time it takes to adapt to the new dentures, considering that implantretained overdentures require 6 months more than CD. Garret et al.8 analyzed mucosasupported prostheses and reported that after denture replacement, there is period of 3 weeks to 18 months, depending on the consistency of the food to be chewed, for prosthesis adjustment and patient adaptation, after which improvement is constant. The adaptation of lower mucosasupport area to the new prosthesis seems to play a key role in masticatory performance. Retention, which is an important aspect to the patient, appears to play a secondary role, similar to the support area. Although it presents better retention, the prosthesis has a support area similar to complete mucosasupported prosthesis. Patients’ first complaints referred to stability and retention of the upper prosthesis. In this study, patients who previously wore lower CD and converted to overdentures had 100% satisfied with prosthesis retention and stability16. This may explain why there were no complaints about the lower denture. Patient satisfaction is related mainly to stability, comfort, ability to chew and to speak, ease of prosthesis cleaning and aesthetics25,26. Not all patients were satisfied with aesthetics prior to replacement. Satisfaction was 100% after one month, remaining so after 3 and 6 months.
Patients in our study already enjoyed good quality of life before treatment, according to the OHIPedent questionnaire, even though they were not satisfied with their prostheses. According to Forgie et al. and Scott et al. 27,28, quality of life involves economic and cultural factors, which were not addressed in this study. The greatest impact on patient quality of life involved retention of food particles under the prostheses (question 2), unsatisfactory adjustment of prostheses (question 3), presence of painful points in the mouth (question 6) and avoiding eating certain foods due to problems with the denture (question 10). After replacement, the answers were more favorable. Avoiding eating certain foods is typical of con ventional complete denture wearers, especially when the quality of dentures is unsatisfactory19,29. The retention of food particles under the prostheses can lead people to avoiding certain types of foods whenever possible, although they are able to chew some foods. The aim of implantretained overdentures is to improve quality of life for individuals considered functionally and psychologically mutilated, as in completely edentulous patients. Both technical quality in rehabilitation and detailed followup after rehabilitation can improve quality of life, satisfaction and masticatory function. It is thus extremely important for the dentist to know about these factors in order to be able to identify the best time to change the prosthesis.
Within the limits of this study, it is suggested that patient satisfaction and aspects of quality of life improved immediately after denture replacement, while the potential for grinding food improved after 3 months.
ACKNOWLEDGMENT
The authors are grateful to the following prosthodontists who helped with the prosthesis delivery: Dr. Vanderlei Luiz Gomes and Dr. Lia Dietrich.
1. Carlsson GE and Omar R. The future of complete dentures in oral rehabilitation. A critical review. J Oral Rehabil 2010; 37: 143-156. [ Links ]
2. Andreiotelli M, Att W and Strub JR. Prosthodontic Complications with Implant Overdentures: A Systematic Literature Review. Int J Prosthodont 2010; 23(3): 195-203. [ Links ]
3. Bressan E, Tomasi C, Stellini E, Sivolella S, Favero G, Berglundh T. Implantsupported mandibularoverdentures: a crosssectional study. Clinical Oral Implants Res 2012; 23; 814-819. [ Links ]
4. Bryant SR, MacDonald Jankowski D, Kim K. Does the type of implant prosthesis affect outcomes for the completely edentulous arch? Int J Oral Maxillofac Implants 2007; 22: 117-139. [ Links ]
5. Dudic A, Mericske Stern R. Retention mechanisms and prosthetic complications of implantsupported mandibular overdentures: longterm results. Clin Implant Relat Res Dent 2002; 4: 212-219. [ Links ]
6. Nevalainen MJ, Rantanen T, Narhi T, Ainamo A. Complete dentures in the prosthetic rehabilitation of elderly persons: five different criteria to evaluate the need for replacement. J Oral Rehabil 1997; 24:251-258. [ Links ]
7. Bergman B, Carlsson GE. Clinical longterm study of complete denture wearers. J Prosthet Dent 1985; 53:56-61. [ Links ]
8. Garrett NR, Perez P, Elbert C, Kapur KK. Effects of improvements of poorly fitting dentures and new dentures on masticatory performance. J Prosthet Dent 1996; 75:269-275. [ Links ]
9. Fenlon MR, Sherriff M. Investigation of new complete denture quality and patients’ satisfaction with and use of dentures after two years. J Dent 2004; 32: 327-333.
10. Allen PF. Association between diet, social resources and oral health related quality of life in edentulous patients. J Oral Rehabil 2005; 32: 623-628. [ Links ]
11. Veyrune JL, Tubert Jeannin S, Dutheil C, Riordan PJ. Impact of new prostheses on the oral health related quality of life of edentulous patients. Gerodontology 2005; 22: 39. [ Links ]
12. Fenlon MR, Sherriff M, Newton JT. The influence of personality on patients’ satisfaction with existing and new complete dentures. J Denti 2007; 35: 744-748.
13. Shigli K. Hebbal M. Assessment of changes in oral healthrelated quality of life among patients with complete denture before and 1 month postinsertion using Geriatric Oral Health Assessment Index. Gerodontology 2010; 27: 167-173. [ Links ]
14. Goiato MC, Garcia AR, Santos DM, Zuim PR. Analysis of masticatory cycle efficiency in complete denture wearers. J Prosthod 2010; 19: 10-13. [ Links ]
15. Borges TF, Mendes FA, Oliveira TRC, Prado CJ, Neves FD. Overdenture with immediate load: mastication and nutrition. Br J Nutr 2011; 105: 990-994. [ Links ]
16. Borges TF, Mendes FA, Oliveira TRC, Gomes VL, Prado CJ, Neves FD. Mandibular Overdentures with Immediate Loading: Satisfaction and Quality of Life. Int J Prosthodont 2011; 24:534-539. [ Links ]
17. Slagter AP, Olthoff LW, Steen WH, Bosman F. Comminution of food by complete denture wearers. J Dent Res 1992; 71:380-386 [ Links ]
18. Mendonca DB, Prado MM, Mendes FA, Borges TF, Mendonca G, Prado CJ, Neves FD. Comparison of masticatory function between subjects with three types of dentition. Int J Prosthodont 2009; 22:399-404. [ Links ]
19. Oliveira TR, Frigerio ML. Association between nutrition and the prosthetic condition in edentulous elderly. Gerodontology 2004; 21:205-208. [ Links ]
20. Feine JS, de Grandmont P, Boudrias P, Brien N, LaMarche C, Tache R, Lund JP. Within subject comparisons of implantsupported mandibular prostheses: Choice of prosthesis. J Dent Res 1994; 73:1105-1111. [ Links ]
21. Awad MA, Lund JP, Shapiro SH, Locker D, Klemetti E, Chehade A, Savard A, Feine JS. Oral health status and treatment satisfaction with mandibular implant overdentures and conventional dentures: A randomized clinical trial in a senior population. Int J Prosthodont 2003;16: 390-396. [ Links ]
22. Mendonca DB, Prado MM, Mendes FA, Borges TF, Mendonca G, Prado CJ, Neves FD. Comparison of masticatory function between subjects with three diferente types of dentition. Int J Prosthodont 2009; 22: 399-404. [ Links ]
23. Souza RF, Patrocinio L, Pero AC,Marra J, Compagnoni MA. Reliability and validation of a Brazilian version of the oral health impact profile for assessing edentulous subjects. J Oral Rehabil 2007; 34:821-826. [ Links ]
24. Badel T, Panduric J, Kraljevic S, Dulcic N. Checking the occlusal relationships of complete dentures via a remount procedure. Int J Periodontics Restorative Dent 2007; 27: 181-192. [ Links ]
25. Cibirka RM, Razzoog M, Lang BR. Critical evaluation of patient responses to dental implant therapy. J Prosthet Dent 1997; 78:574-581. [ Links ]
26. Awad MA, Feine JS. Measuring patient satisfaction with mandibular prostheses. Community Dent Oral Epidemiol 1998; 26: 400-405. [ Links ]
27. Forgie AH, Scott BJ, Davis DM. A study to compare the oral health impact profile and satisfaction before and after having replacement complete dentures in England and Scotland. Gerodontology 2005; 22: 137-142. [ Links ]
28. Scott BJ, Forgie, AH, Davis DM. A study to compare the oral health impact profile and satisfaction before and after having replacement complete dentures constructed by either the copy or the conventional technique. Gerodontology 2006; 23:79-86. [ Links ]
29. Oliveira TRC, Borges TF, Mendes FA, Neves FD. Malnutrition in the 21st Century.Risk of malnutrition in completely edentulous individuals (Chapter XIV). United States: Nova Science Publishers, 2007; 265-280. [ Links ]














