Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Odontológica Latinoamericana
versão On-line ISSN 1852-4834
Acta odontol. latinoam. vol.31 no.2 Buenos Aires ago. 2018
ORIGINAL ARTICLE
Self-medication in patients seeking care in a dental emergency service
Automedicación en pacientes que concurren a un servicio de guardia odontológica
Federico Stolbizer1,2, Daniel F. Roscher1, Maria M. Andrada1, Lautaro Faes2, Carla Arias2, Cecilia Siragusa1,2, Silvio Prada2, Jonathan Saiegh2, Daniel Rodríguez2, Ariel Gualtieri3, Carlos F. Mendez4,5
1 Universidad de Buenos Aires. Facultad de Odontología. Cátedra de Cirugía y Traumatología Bucomaxilofacial II. Buenos Aires. Argentina.
2 Universidad de Buenos Aires. Facultad de Odontología. Servicio de Emergencias. Buenos Aires. Argentina.
3 Universidad de Buenos Aires. Facultad de Odontología. Cátedra de Biofísica y Bioestadística. Buenos Aires. Argentina.
4 Universidad de Buenos Aires. Facultad de Odontología. Cátedra de Farmacología. Buenos Aires. Argentina.
5 CONICET-Universidad de Buenos Aires. Instituto de investigaciones Biomédicas (INBIOMED). Buenos Aires. Argentina.
ABSTRACT
The aims of this work were: To determine what percentage of first-time patients to the Dental Emergency Department at the School of Dentistry of Buenos Aires University had taken medications to relieve or treat their condition. To determine what percentage of these had used self-medication, and which were the most frequently taken medicines. To determine whether there is an association between self-medication and educational level, and between self-medication and whether the patient has health coverage. This was an observational, cross-sectional study which reviewed 567 clinical histories of patients who visited the Dental Emergency Department from March 2015 to September 2016. The following parameters were assessed: sex, age, reason for consultation, medication, dose, interval, duration and indication. Patients'educational level and whether they had health coverage were ascertained. Confidence intervals of 95% were calculated for percentages using the Wilson score method. Inferential analyses were performed using the Chi-square test (f). Significance level was set at 5%.
Eighty five percent (85%,.n=481) of the patients had taken at least one medication; 77% (n=372) had used self-medication.
The most frequently used medicines were non-steroid antiinflammatory drugs (61%), antibiotics (34%) and glucocorticoids (2%). No association was found between self-medication and patients' having health coverage (2=13; p=0.08). No significant association was found between educational level and selfmedication (2=10; p=0.22). Nevertheless, the lowest percentages of self-medication were found in subjects with complete university studies (77%; CI95: 60% to 89%), while the highest percentages were found in subjects with incomplete primary education (89%; CI95: 69% to 97%), complete primary education (92%; CI95: 82% to 96%) and incomplete secondary educations (90%; CI95: 84% to 94%).High levels of selfmedication were found in the study population. Although no association was found between educational level and self-medication behavior, the percentage of self-medication was higher among patients with lower educational levels. The high level of self-medication highlights the importance of conducting campaigns to raise awareness about the adequate use of medicines.
Key words: Self-medication; Emergency service; Hospital; Dentistry.
RESUMEN
Los objetivos del presente trabajo fueron: Determinar qué porcentaje de pacientes que concurrió por primera vez al Servicio de Urgencias de la Facultad de Odontología de la Universidad de Buenos Aires consumió medicamentos para aliviar o tratar su dolencia. Determinar qué porcentaje de pacientes fueron automedicados, y cuáles fueron los medicamentos más utilizados. Determinar si existe relación entre la automedicación y el nivel de estudio y entre la automedicación y la presencia de cobertura médica. Se realizó un estudio observacional y transversal. Se relevaron 567 historias clínicas de pacientes que concurrieron entre marzo 2015 y septiembre 2016 y se valoraron los siguientes parámetros: sexo, edad, origen de la consulta, medicación, dosis, intervalo, duración, e indicación. Se indagó el nivel educacional alcanzado y la existencia de cobertura médica. Se calcularon intervalos de confianza al 95% para porcentajes mediante el método score de Wilson. Se realizaron análisis inferenciales mediante la prueba Chi-cuadrado (2). Se fijó un nivel de significación del 5%.
El 85% (n=481) de los pacientes había consumido al menos un medicamento. El 77% (n=372) de los pacientes estaba automedicado. Los medicamentos más utilizados fueron antiinflamatorios no esteoroideos (61%), antibióticos (34%) y glucocorticoides (2%). No se encontró asociación entre la automedicación y la presencia de cobertura médica (x2=13; p=0,08). No se encontró asociación significativa entre el nivel de estudios y la automedicación (x2=10; p=0,22). Sin embargo, los sujetos con estudio universitario completo presentaron el menor porcentaje de automedicación (77%; IC95: 60% a 89%), mientras que los mayores porcentajes se encontraron en sujetos con primario incompleto (89%; IC95: 69% a 97%), primario completo (92%; IC95: 82% a 96%) y secundario incompleto (90%; IC95: 84% a 94%).
Se encontraron niveles elevados de automedicación en la población estudiada. Si bien no se observó asociación entre nivel educativo y la conducta de automedicación, fue mayor el porcentaje de automedicación en pacientes con menor nivel educativo. La alta presencia de automedicación refuerza la importancia de realizar campañas de concientización sobre el consumo adecuado de medicamentos.
Palabras clave: Automedicación; Servicio de urgencia; Odontología.
INTRODUCTION
According to the World Health Organization, selfmedication is the selection and use of medicines by individuals to treat self-recognized diseases or symptoms12.
Acute dental pain is, in many cases, invalidating and is often described as one the most severe a person can suffer in everyday life. In dentistry, patients often recur to self-medication to reduce dental pain, mainly by taking analgesics and sometimes including antibiotics3. This practice has numerous consequences, including an increased risk in untoward effects, drug-drug interactions, increased bacterial resistance to antibiotics, masking of underlying pathologies and/or conditions and reduction of the efficacy of treatment due to inadequate or insufficient use of medicines4.
Self-medication today is still relevant to public health worldwide, with 8% to 13% prevalence in European and North American populations. This high frequency may be attributed to the availability of medicines to society and sometimes to poor coverage in healthcare services5.
In Argentina, a survey conducted by the Argentine Pharmaceutical Confederation found that out of 1500 respondents in the cities of Buenos Aires and Córdoba, 82% take over-the-counter medicines and more than half of the individuals are unaware of the untoward effects they can cause. It is estimated that 11% of all cases of chronic kidney failure are a consequence of the use of analgesics and 40% of high digestive hemorrhage cases can be attributed to acetylsalicylic acid and other non-steroid antiinflammatory drugs (NSAIDs)6.
To date, no study has been published in Argentina reporting the extent of self-medication in situations of urgent dental conditions. We aim here to study the prevalence of self-medication in patients seeking dental care at the Dental Emergency Service of the School of Dentistry at the University of Buenos Aires. We also aimed to determine a possible association between self-medication and type of health coverage and/or patient's educational level.
MATERIALS AND METHODS
A total of 567 clinical histories of patients who spontaneously visited the Dental Emergency Department of the School of Dentistry at the University of Buenos Aires seeking dental care from March 2015 to September 2016 were analyzed. Exclusion criteria were patients younger than 16 years, patients consulting for esthetic reasons and patients failing to provide written informed consent to participate in the study. Before case resolution, clinical histories were prepared, type of urgency determined, and patients were asked to declare any prior care or medicine they have taken whether prescribed or self-indicated. Patients on medication were asked to indicate type of medicine, origin of treatment, dose, route of administration, interval and duration. Self-perceived improvement of patient condition, total duration and/or possible discontinuation of the treatment was also recorded. The sample consisted of 381 males (67.2%) and 186 females (32.8%) with median age 34 and a range between 16 to 89 years.
Confidence intervals of 95% were calculated for percentages using the Wilson score method. Inferential analyses were performed using the Chi-square test (χ2). Significance level was set at 5%.
RESULTS
Of recorded cases, 85% (n=481; CI95: 82% to 88%) had taken at least one medicine, while 15% (n=109; CI95: 12% to 18%) declared no medication related to the dental episode prior to consultation (χ2=275; p<0.05). Of total medicated patients, 77% (n = 372; CI95: 73% to 81%) recurred to self-indication, while 23% (n=109; CI95: 19% to 27%) had taken medicines under professional prescription (82% dentists, 18% physicians).
No significant differences (χ2=1.55; p=0.21) were observed when data was analyzed by gender, with 85 (325/381) and 84% (156/186) medication rates for males and females, respectively.
Among the 567 urgencies treated, the reason for consultation was primarily endodontic in 60% of included cases (n=340; CI95: 56% to 64%), infectious in 16% (n=92; CI95: 13% to 19%), post-surgical problems in 12% (n=67; CI95: 9% to 15%), periodontal in 5% (n=31; CI95 4% to 8%), temporomandibular joint disorders in 1% (n=5; CI95: 0% to 2%), and miscellaneous reasons in 6% (n=32; CI95: 4% to 8%). Fifty-six percent (n=269; CI95: 51% to 60%) of patients had taken one medicine, 36% (n=173; CI95: 32% to 40%) had taken 2, and 8% (n=39; CI95: 6% to 11%) had taken three or more. Self-medicated patients used medicines from a variety of therapeutic classes (χ2>=667; p<0.05). The most frequently used category was NSAIDs (61%; CI95: 57% to 64%), followed by antibiotics (34%; CI95: 31% to 38%), glucocorticoids (2%; CI95: 1% to 3%), and others (3%; CI95: 2% to 5%).
Among NSAIDs, the most frequently used was ibuprofen (45%; CI95: 41% to 50%), followed by ketorolac (33%; CI95: 28% to 37%), diclofenac (11%; CI95: 8% to 14%), and others 11%; CI95: 9% to 15%) (Table 1).
Table 1: Frequency of NSAID use in the self-medicated group.

A wide range of antibiotics was used. Among self-medicated patients, the most frequent antibiotic was amoxicillin (80%, CI95: 75% to 85%), followed by amoxicillin/clavulanate association (10%; CI95: 7% to 14%), azithromycin (6%; CI95: 4% to 10%), cefalexin (2%; CI95: 1% to 5%), and others (2%; CI95: 1% to 5%) (Table 2).
Table 2: Frequency of antibiotic use in the selfmedicated group.

The rate of self-medication was also studied in terms of type of health coverage presented by patients. As shown in Fig.1, when analyzed against health coverage, a trend that did not reached statistical significance (*2=3.18; p=0.08) towards a higher use of medicines without prescription was detected in patients lacking health insurance.
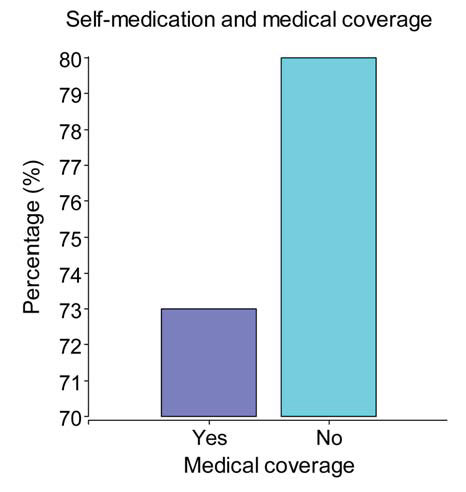
Fig. 1: Percentage of self-medicated patients and medical coverage.
No significant association was found either between educational level and self-medication (*2=10; p=0.22). Nevertheless, the percentage of subjects with complete university studies who used self-medication was lower (77%; CI95: 60% to 89%), as compared to subjects with incomplete primary education (89%; CI95: 69% to 97%), complete primary education (92%; CI95: 82% to 96%) and incomplete secondary education (90%; CI95: 84% to 94%) (Fig. 2).

Fig. 2: Educational level for all patients in the study.
DISCUSSION
Self-medication is a very common habit in Latin America. We report here that 77% of the patients surveyed at the Dental Emergency Service of the School of Dentistry at the University of Buenos Aires incurred in self-medication. Our results agree with those presented by Ramay, et al that reported 79% self-medication with antibiotics in suburban areas and 77% in central areas of Guatemala City9. Other investigators also reported similar results in Bolivia13, with 72% and Peru14,15 with 81 and 69% prevalence of self-medication, respectively. Even higher numbers for self-medication were reported among university students in Brazil11 and medical students in Cuenca, Ecuador12 while a 41% prevalence was informed in Mexico10. Differences in results may be accounted by the type and size of population surveyed and institution in which the study was performed, among other variables. Our study included patients who spontaneously sought attention by the Emergency ward at a Dental University Hospital in central Buenos Aires, Argentina. Our study surveyed also all types of medications related to the dental condition affecting the sampled individuals and is, thus, not limited to a single class of therapeutic agents.
Prescription legislation in Argentina is extensive and current laws were originally established in the 1960s. The fact that 70% of the medicines that enrolled patients declare to use in our study require prescription, shows that neither patients nor pharmacies comply with the enforced regulation. Analgesics were most frequently used by patients, as reported in other studies 4,7,10,12-15. Although not statistically significant, a lower prevalence of selfmedication was detected among patients with complete university studies, something that points out to a possible relationship between instruction and a more responsible use of medication.
Some of the causes of these high figures in Latin America might be deficient healthcare services, long waiting times at urgent care service providers, cost of medical care, media advertising and the role of pharmacists and healthcare professionals. Many patients are unaware of the consequences of self-medication, which include increased risk of untoward reactions to drugs, drug-drug interaction, increase in bacterial resistance, masking of underlying pathologies and/or conditions and reduction in the efficacy of treatment as a result of inadequate or insufficient use of medicines.
CONCLUSION
Strategies should be developed to ensure that physicians, dentists, nurses and pharmacists make rational use of medicines. Other effective strategies may be campaigns to raise awareness among the population regarding the consequences of self-medication and improved access to primary healthcare centers.
CORRESPONDENCE
Dr. Federico Stolbizer
Cátedra de Cirugía y Traumatologia Bucomaxilofacial II Faculatad de Odontología Marcelo T. de Alvear 2142 (C1122AAH) Buenos Aires, Argentina fstolbizer@gmail.com
FUNDING
This study was supported, in part, by a grant form Universidad de Buenos Aires (UbACYT 20020150100172BA) to CFM.
1. World Health Organization. The role of pharmacist in selfcare and self-medication. Report of the 4th WHO Consultative group on the role of the pharmacist. 1998. The Hague, The Netherlands. WHO/DAP/98. URL: http://apps.who.int/ medicinedocs/es/d/Jwhozip32e/ [ Links ]
2. Dahir C, Hernandorena C, Chagas L, Mackern K, Varela V, Alonso I. Automedicación: un determinante en el uso racional de medicamentos. Evid Act Pract Amb 2015; 18:46-4. URL: http://www.evidencia.org.ar/files/0aabef9c6504180b3e8bd3 9807a23a86.pdf [ Links ]
3. Hernandez-Juyol M, Job-Quesada JR. Dentistry and selfmedication: a current challenge. Med Oral 2002; 7:344347. [ Links ]
4. Machado-Alba JE, Echeverri-Cataño LF, Londoño-Builes MJ, Moreno-Gutiérrez PA, Ochoa-Orozco SA, Ruiz-Villa JO. Social, cultural and economic factors associated with self-medication. Biomedica 2014; 34:580-588. [ Links ]
5. Guillem Sáiz P, Francés Bozal F, Gimenez Fernández F, Sáiz Sánchez C. Estudio sobre automedicación en población universitaria española. Rev Clin Med Fam 2010; 3:99-103. URL: http://scielo.isciii.es/pdf/albacete/v3n2/original7.pdf [ Links ]
6. Restrepo APB, Vargas SCM, Cárdenas MMP, Bano ID. Automedicación en pacientes de los servicios de urgencias de odontología del CES, 1995-1996. CES Odontol 2010;9: 98-104. URL: http://revistas.ces.edu.co/index.php/odontologia/ article/view/1194. [ Links ]
7. Marulanda FAT. Estudio sobre automedicación en la Universidad de Antioquia, Medellín, Colombia. IATREIA 2010; 15: 242-247 URL:http://aprendeenlinea.udea.edu.co/ revistas/index.php/iatreia/article/view/3963 [ Links ]
8. Ramay BM, Lambour P, Ceron A. Comparing antibiotic selfmedication in two socio-economic groups in Guatemala City: a descriptive cross-sectional study. BMC Pharmacol Toxicol 2015; 16:11. [ Links ]
9. Castellanos J, Ramirez N, Marquez G. Características de la automedicación en pacientes ingresados en un servicio de urgencias. México: Hospital General Regional 2005. URL: http://www.sld.cu/galerias/pdf/sitios/urgencia/017_-_caracteristicas_de_la_automedicacion_en_pacientes_ingre sados_en_un_servicio_de_urgencias.pdf [ Links ]
10. Damasceno DD, Terra FS, Zanetti HHV, D'Andréia ED, Silva HLR, Leite JA. Automedicação entre graduandos de enfermagem, farmácia e odontologia da Universidade Federal de Alfenas. Rev Min Enferm 2007; 11:48-52. DOI: http://www.dx.doi.org/S1415-27622007000100008 [ Links ]
11. Andrade Izquierdo AV, Arévalo Torres MJ. Características de la automedicación en las y los estudiantes de la Escuela de Medicina, de la Facultad de Ciencias Médicas de la Universidad de Cuenca en el período lectivo 2008-2009. 2009. Tesis de Licenciatura URL: http:/dspace.ucuenca.edu.ec/ handle/123456789/19707. [ Links ]
12. Ortiz AF, Ortuño LP, Ortega MO, Paucara CG. Estudio sobre automedicación en población mayor de 18 años del distrito de Sarcobamba de la Cuidad de Cochabamba. Rev Cient Cien Med 2008; 11:5-9.URL: http://www.redalyc.org/ articulo.oa?id=426041217003 [ Links ]
13. Conhi A, Castillo D, Del Castillo C. Automedicación odontológica de pacientes que acuden a una institución pública y privada, Lima - Perú. Rev Estomatol Herediana 2015; 25:205-210. URL:http://www.scielo.org.pe/scielo.php?pid=S1019-43552015000300005%26script=sci_arttext%26tlng=en [ Links ]
14. Pumahuanca O, Cruz T. Automedicación con AINES por pacientes con odontalgia en la consulta pública y privada. Rev Evid Odontol Clin 2017; 2:30-33 URL:https:// www.uancv. edu.pe/revistas/index.php/EOC/article/download/363/304 [ Links ]
15. De-Paula KB, Silveira LSD, Fagundes GX, Ferreira MBC, Montagner F. Patient automedication and professional prescription pattern in an urgency service in Brazil. Braz Oral Res 2014; 28:1-6. [ Links ]














